|
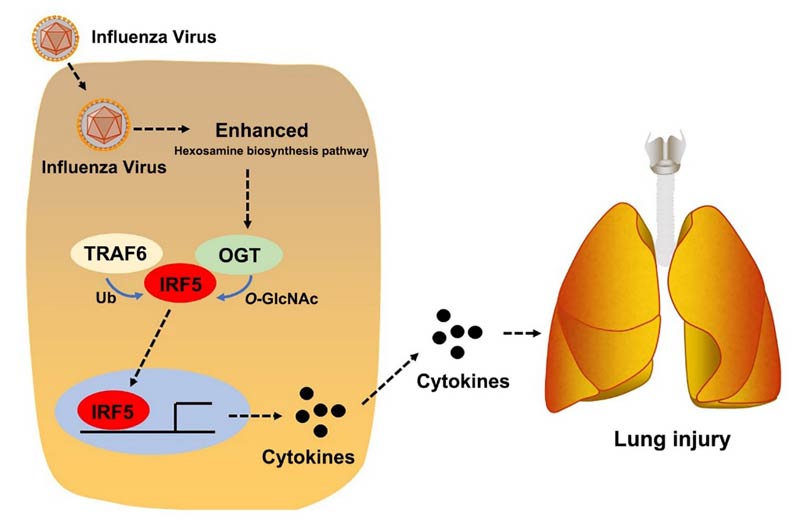
For a limited time only, PBS is streaming a free documentary on America’s diabetes epidemic (it may not be available in all areas; check your local PBS to see if it’s in your area). Coincidentally, diabetes is a comorbidity that can increase your chances of contracting and even dying from COVID-19,1 making this documentary particularly timely. One of the best strategies to beat COVID-19 is to get any underlying chronic conditions under control. Type 2 diabetes and high blood pressure — both of which have been implicated as underlying factors causing serious COVID-19 disease — can often be reversed via healthy diet and lifestyle. According to a January 2019 update by the U.S. Centers for Disease Control and Prevention, more than 122 million American adults have diabetes or prediabetes,2 and the economic ramifications of this condition are enormous. The U.S. spent $350 billion treating diabetes in 2019 alone, according to the film. Also according to the film, projections predict half the American population will be prediabetic or diabetic by 2025. Such predictions reflect poor research because if you use insulin resistance as your definition, 80% of the country is diabetic or prediabetic already.3,4 Glucose Metabolism Influences Cytokine StormsAn April 15, 2020, article5 in The Scientist reviews evidence6,7 that helps explain why obesity and diabetes are such potent risk factors for severe COVID-19 infection. In a nutshell, higher blood glucose levels appear to play a significant role in viral replication and the development of cytokine storms. While the research in question looked at influenza A-induced cytokine storms, these findings may well be applicable in COVID-19 as well. Cytokines are signaling molecules that are released by your immune system in response to foreign invaders. They, in turn, act as messengers that instruct other immune cells to fight the pathogen. In some cases, this immune response goes into overdrive, resulting in what’s known as a “cytokine storm” that can cause severe tissue damage and lead to death. A cytokine storm response is typically the primary reason why people die from infections, be it the seasonal flu, Ebola, urinary tract infection or COVID-19. A critical player in cytokine production is the transcription factor interferon regulatory factor 5 (IRF5). In mice, genetically eliminating IRF5 protects them from influenza-induced cytokine storms.8 Interestingly, “the inflammatory response to influenza infections is also known to drive up glucose metabolism,” The Scientist reports,9 “in part so that immune cells have the necessary energy to mount a strong response, and also because the virus needs the sugar to replicate.” According to researchers at the State Key Laboratory of Virology at Wuhan University, the hexosamine biosynthesis pathway — a glucose metabolism pathway — is responsible for activating IRF5-induced cytokine production in cells and mice. The same pathway is also responsible for viral replication, they say.10,11,12 As reported by The Scientist:13
In a Science Advances press release, co-author Shi Liu states:14
Insulin Resistance Is the Real PandemicSo, the real pandemic here appears to be dysregulated glucose metabolism; in other words, insulin resistance, which is exceedingly prevalent in the U.S.15,16 Insulin resistance, in turn, is a diet-induced condition. Unless addressed, insulin resistance eventually develops into full-blown Type 2 diabetes. As mentioned earlier, if you use sensitive measure for insulin resistance, approximately 80% of the population has this metabolic dysfunction.17,18 Processed foods — which are loaded with added sugars, processed grains and industrially processed omega-6 vegetable oils — are the primary culprits causing insulin resistance, Type 2 diabetes and obesity and, according to FoodNavigator.com,19 doctors are finally starting to talk about the food industry’s role in the COVID-19 pandemic:
Diabetes Is ReversibleAs noted by PBS, Type 2 diabetes can be very difficult to control when relying on drugs alone and not doing anything about the underlying lifestyle factors actually causing the problem. While not addressed in the film, the use of insulin in Type 2 diabetes is particularly problematic. If the underlying lifestyle factors are properly addressed, Type 2 diabetes is entirely reversible in most people, and rather easily so. The reason for this is because Type 2 diabetes is a diet-derived condition. It’s rooted in insulin resistance and faulty leptin signaling, caused by chronically elevated insulin and leptin levels. As such, it can be effectively treated and reversed through dietary and other lifestyle means. For example, as detailed in my 2019 article “Fasting Prevents and Halts Diabetes,” research has shown fasting can improve insulin sensitivity,21 reverse diabetes22 and support your weight management efforts when combined with exercise.23 While “Blood Sugar Rising” discusses the foundational role of diet in this disease, it does not touch on fasting at all. This is unfortunate, considering how effective it can be. In a case series paper24,25 published in BMJ Case Reports, Dr. Jason Fung and associates details how fasting can actually be used as a therapeutic alternative for Type 2 diabetes. As noted by the authors, their paper:
Now, a case series paper is not a controlled study; rather, it simply presents the case history of one or more patients and may propose a hypothesis for why a treatment did or did not work. In this case, three diabetic patients between the ages of 40 and 67 participated in a supervised fasting regimen to evaluate the effects on their insulin requirements. The patients had been diagnosed with Type 2 diabetes for 10, 20 and 25 years respectively, and were taking insulin daily. Of the three patients, two did alternating-day, 24-hour fasts, while one fasted for 24 hours three times a week over a period of several months. The complete manual of the fasting regimen used is described in Fung’s book, “The Complete Guide to Fasting.”26 Two of the patients were able to discontinue all of their diabetes medications while the third was able to discontinue three of his four drugs. All three also lost between 10% and 18% of their body weight. With another similar trial, The Guardian reported on,27 Type 2 diabetics were placed on a severely restricted calorie diet where they ate just 600 calories a day for eight weeks. By the end of their fast, all were disease-free, and three months later, having returned to their regular diet, seven of the 11 participants remained free of diabetes. There’s Hope Even for Severe DiabetesSeveral studies have even found that repeated episodes of fasting can induce cell growth of pancreatic beta cells in mice.28 The growth is associated with an increased expression of Ngn3,29 a protein involved in converting DNA into RNA critical for endocrine cells in the pancreatic islets of langerhans, the cells responsible for producing insulin. The increase in islet beta cells induced through intermittent fasting was accompanied by a marked improvement in blood sugar control in the animals. While individuals suffering from Type 1 diabetes often experience near complete inflammatory destruction of the islet beta cells, the same occurs in the later stages of severe Type 2 diabetes as well. In a BMJ editorial,30 research scientist James DiNicolantonio, PharmD.,31 discusses these results, noting the findings may open the path to reversing Type 2 diabetes in those with “enough discipline and commitment to adopt a lifestyle that would have prevented diabetes in the first place.”32 As a first step, he recommends you first practice a diabetes preventive lifestyle — eating a diet primarily of whole foods, complemented with regular exercise. This will help improve your insulin sensitivity and may prove sufficient for those with a recent diagnosis of diabetes to reverse their condition over time. In those who fail to respond, he recommends a time-restricted eating protocol, which provides many of the same benefits as longer fasting while being much easier to comply with. Supplemental measures may also be implemented to shield the beta cells from toxicity so they retain functional capacity. For example, reducing islet oxidative stress may be accomplished using spirulina, NAC and/or berberine.33 Ultimately, the goal is to achieve normal blood sugar control without drugs and maintain compliance with a diabetic preventive diet and lifestyle. This also includes physical activity. Chronic inactivity such as extended sitting is one of the primary risk factors for insulin resistance and Type 2 diabetes. The reason for this is because sitting shuts down or blocks a number of insulin-mediated systems, including muscular and cellular systems that process blood sugar, triglycerides and cholesterol. Standing up activates all of these systems at the molecular level. Dr. James Levine detailed the science of this in our 2014 interview. Diabetes Takes a Heavy Toll on HealthAs detailed in the film, chronically high blood sugar from poor nutrition and lack of exercise can trigger long-term damage to your body and make you more prone to other chronic health problems and diseases, including but not limited to:34,35,36
Sugar-Rich Diets Are a Primary CulpritWhile PBS largely focuses on the conventional treatment of diabetes, which typically involves insulin and other drugs, it thankfully highlights the fact that sugar- and carb-rich diets are a primary driver.37 Research38 shows that once you reach 18% of your daily calories from sugar, there’s a twofold increase in metabolic harm that promote prediabetes and diabetes. As a standard recommendation, I strongly advise keeping your total sugar consumption below 25 grams per day, which is about 6 teaspoons. If you have signs of insulin resistance such as hypertension, obesity or heart disease, you’d be wise to limit sugar to 15 grams or less until your weight and other health conditions have normalized. Sadly, as noted by PBS, “the game is rigged.” Food products are allowed to state “sugar free” on the package, even though they’re loaded with carbohydrates and sugar alternatives. As noted in the film, it’s not just sugar itself that must be avoided, but anything that turns into sugar in your body as well, most notably grains. In short, a high-grain, low-fat diet is a perfect prescription for diabetes, yet these kinds of foods are allowed to make a number of health claims. This kind of misleading labeling is causing many to think they’re making wise food choices when in fact they’re not. It would help to remember that just about all processed foods are best avoided. Rather than trying to decipher labels, ditch the processed foods and fast food restaurants and cook from scratch using whole, unprocessed foods. This is by far the easiest and most effective way to improve your diet. Soybean Oil Promotes DiabetesOne dietary factor not directly addressed in the film is processed vegetable oils. These may actually be worse than fructose in terms of the metabolic harm they cause.39 Soybean oil in particular has a questionable safety profile, and processed foods are positively loaded with it. Whether partially hydrogenated, organic or genetically modified to be low in linoleic acid, soybean oil can cause dysfunction at a cellular level. Unfortunately, many health authorities have insisted omega-6-rich vegetable oils like soybean oil are healthier than saturated animal fats such as butter, lard and coconut oil, and this myth has been a tough one to dismantle, despite the evidence against it. Most recently, research40,41,42 published in the January 2020 issue of Endocrinology found soybean oil — the most widely consumed cooking oil in America — can cause metabolic changes associated with:
According to the authors, both conventional and genetically engineered soybean oil caused dysfunction in about 100 different genes in the hypothalamus, including genes associated with “inflammation, neuroendocrine, neurochemical and insulin signaling.” Similar results were reported in a 2015 study,43 in which soybean oil was found to increase weight gain, body fat, diabetes, glucose intolerance and insulin resistance. Here too, soybean oil diets upregulated genes involved in diabetes, obesity, inflammation, mitochondrial function and cancer. Ketogenic Diet Improves Insulin SensitivityAside from fasting or time-restricted eating, a cyclical ketogenic diet is an effective way to improve your insulin sensitivity and reverse diabetes. A cyclical ketogenic diet — as detailed in my book “KetoFast” — shifts your body's metabolic engine from burning carbohydrates to burning fats. Your cells have the metabolic flexibility to adapt from using glucose for fuel to using ketone bodies, which come from the breakdown of fats, hence, the name "ketogenic." Another term for this is nutritional ketosis. One of the fastest ways to prevent nutritional ketosis is by consuming sugar or refined carbohydrates. A ketogenic diet calls for 50% to 70% of your daily calories to come from beneficial fats such as coconut oil, grass-pastured butter, organic pastured eggs, avocado or ketone producing fats like MCT oils, particularly C-8, while restricting your carbohydrates to 30 or 40 grams per day. Along with an appropriate amount of protein, this is typically enough to get you into ketosis. Watch ‘Blood Sugar Rising’“Blood Sugar Rising” provides an eye-opening glimpse into the very real struggles of Type 2 diabetics, as well as the around-the-clock challenges faced by those with Type 1 diabetes — a genetic condition in which your body produces no insulin at all — and groundbreaking inventions such as a bionic pancreas that automatically delivers the appropriate insulin dose as needed. The film also reviews the real-world ramifications of skyrocketing insulin prices. The two types of diabetes differ in terms of their origin, and while insulin is typically ill advised for Type 2 diabetics,44 Type 1 diabetics die without it. It also highlights the role of food as a cultural component, and how food-centered cultures can be guided to make healthier choices. For example, saying you have to abstain from rice, pasta or potatoes can be nearly impossible in certain families and cultures. Instead, you may need to approach it in terms of better and worse ways of preparing these foods, and restricting the amounts. Diabetes, or more accurately insulin resistance with metabolic inflexibility, is a health accident waiting to happen, but it’s important to realize that you have control and can do something about it. In virtually all cases, it will require making more or less drastic changes to your diet and lifestyle, but the payoff goes beyond preventing diabetes. Concomitant with that, you’re also protecting your vision and lowering your risk of most of the chronic diseases that lead to an early grave. from http://articles.mercola.com/sites/articles/archive/2020/04/30/blood-sugar-rising.aspx
0 Comments
You may know visceral fat by another name — belly fat. In fact, it goes by several names such as "beer belly" and "middle-age spread." While many see it as an aesthetic problem, carrying extra weight in your midsection has a significant effect on your physical health, including your brain. You have two basic types of fat. Subcutaneous fat is found just under the skin and is the type that jiggles and dimples. Visceral fat is found under the abdominal muscle, wrapped around your internal organs. This type is more dangerous as it's linked to the production inflammatory cytokines and is considered biologically active.1 Visceral fat also increases insulin resistance and your risk for metabolic syndrome. It plays a role in the development of Type 2 diabetes, heart disease, breast cancer, colorectal cancer and Alzheimer's disease.2 While many consider their body mass index (BMI) as an indication of whether they fall into a category of overweight or obesity, it is your waist measurement in combination with your waist-to-hip ratio that is a better indication of health. This measurement of visceral fat helps predict your potential risk for chronic disease and even mortality. Where fat deposits on your body has a distinct impact on your health. Deposits in the hips and thighs result in a pear shape that has a lower potential risk for chronic disease than those with fat deposits in the abdomen, described as an apple shape. Visceral Fat Associated With DementiaOne of the first studies3 in which researchers evaluated the association between belly fat and dementia was published in 2008. An analysis was conducted of 6,583 people in Northern California. Abdominal measurements were taken and 36 years later researchers looked for recorded diagnoses of dementia in the participants. Of the cohort, 15.9% were diagnosed with dementia. Researchers compared those with lowest abdominal girth against the highest and found the highest had a three-fold increased risk. In the past decade the terms "normal weight metabolic obesity," "skinny fat" and "normal weight obesity" have been used to describe those who have a normal BMI but have metabolic characteristics of being obese.4 These individuals carry excess belly fat. One of the risks associated with a high waist-to-hip ratio, even when having a normal weight, is declining cognitive function. But not all studies yield straightforward results linking the two conditions. In a cross-sectional autopsy study,5 researchers evaluated 234 participants with abdominal visceral fat measured on autopsy. They looked for associations between visceral fat and cognitive impairment as defined by clinical dementia. What they found were those who had higher amounts of central obesity had a lower risk of dementia later in life. Although the authors of other studies found a relationship between obesity and cognitive impairment, the researchers expected those findings since the measurements were made at the same time and the samples were mainly of older adults. In past studies scientists have demonstrated a link between obesity and a higher risk of cognitive function decline, yet when measured later in life the results are conflicting. The researchers reported on several studies that used a direct measurement of abdominal visceral fat and had demonstrated the same relationship found in this study. In one, a significant reduction in BMI later in life increased the risk of developing dementia in the following three years by 118%. Study Finds a Pathway That Visceral Fat Affects CognitionIt's not enough to know a link exists. Scientists also want to know what happens at a molecular level. Researchers from Augusta University recently published a study6 that showed, for the first time, one pathway visceral fat may use as it damages your brain cells. The effect influences the microglia, or immune cells in the brain, to change behavior and then trigger functional damage to your neurons.7 The results are important, as one of the researchers commented in a press release from the University:8
The signal is a proinflammatory protein called interleukin-1 beta that doesn't often enter the brain. However, visceral fat "generates high, chronic levels of the signal that in turn over-activate the usually protective microglia, the resident immune cells in our brain." Research has demonstrated these reactions were problematic and this offers evidence as to how they are triggering problems. Using an animal model, the researchers studied the effect on cognitive function and inflammation. These findings help to add pieces to the puzzle of how interleukin-1 beta may affect actions in the central nervous system. Bigger Belly Predicts Heart Disease Better Than BMIAfter a lifetime of exposure to pathogens and toxins, a weakened and overactive immune system may trigger chronic inflammation.9 When the inflammatory response triggered by visceral fat is added to this burden it may be a better predictor of heart health than your overall weight. This means those who are normal weight with visceral fat carry a greater risk than they may imagine. Two studies that were released almost simultaneously revealed similar results — those who carry a spare tire have a greater risk of heart failure or heart disease. The first from the Norwegian University of Science and Technology was a meta-analysis of 23 studies with 650,000 participants. They looked at BMI and the risk of heart failure, finding the risk rose 41% with a rise of five BMI units and accelerated with greater weight gain.10 Those who were obese had a risk two to three times greater than their normal weight counterparts. The researchers also noted for every 10 centimeters (approximately 4 inches) of an increase in a participant's waist measurement, there was a 29% increased risk of heart failure. The leaders of several of the studies had adjusted for factors that affect heart health, such as high blood pressure, diabetes and a poor lipid profile, but those with a higher waist circumference continued to have a greater correlation. One of the scientists from the study commented:
The second study from the Intermountain Medical Center Heart Institute and Johns Hopkins Hospital evaluated the risks of central obesity as a predictor of heart disease in those also suffering Type 1 or Type 2 diabetes without previous symptoms of heart disease.11 The team started with 200 participants who met the criteria and discovered that independent of total body weight, central obesity "was strongly associated with regional left ventricular dysfunction, which is a common cause of heart disease, including congestive heart failure." The results were presented at the 2016 American College of Cardiology Scientific Session. The co-director of research from Intermountain Medical Center Heart Institute, Dr. Brent Muhlestein, commented on the results of the study and the implications it has on assessment and treatment.12
Stomach Fat Affects Mental HealthVisceral adipose tissue is also linked to mental health conditions such as depression and anxiety. In one study of postmenopausal women, those with abdominal obesity were more likely to struggle with depression than those without. This led the researchers to conclude that "visceral fat accumulation was an independent and positive factor significantly associated with the presence of depressive symptoms."13 Men also suffer from a higher risk of depression with abdominal obesity, as demonstrated by a study of 2,502 men and women. The researchers measured leptin levels and visceral fat and used either an assessment scale or antidepressant prescription to measure depression.14 They found higher levels of leptin increased the risk of depression in men, leading this team to conclude:
The link between abdominal obesity and depression may be related to the inflammatory response the active fat triggers. Inflammation has a link to depression as demonstrated in several studies. In a literature review15 of 30 studies with 1,610 participants, researchers found anti-inflammatory agents reduced symptoms of depression when compared to a placebo. These results support other evidence finding a link between inflammation and depression.16,17 Unfortunately, mental health screening may overlook this factor. Evaluate Your Risk With Waist-to-Hip RatioAs demonstrated in this short video, using a waist-to-hip ratio is a more reliable indication of your future risk of chronic disease, heart disease and mental health. A higher ratio is suggestive of more visceral fat accumulation around your abdominal organs, which is far more hazardous to your health than the subcutaneous fat located directly under your skin. To determine your waist-to-hip ratio you'll want to measure both areas. Start by measuring your waist using a spring-loaded or cloth tape measure. Find your waist, which is your midpoint between your last rib and your iliac crest. These are the bones on the front of your abdomen, as shown in this video. Measure the area in the middle without pulling the tape measure too tight. Take a couple of measurements, allowing 30 seconds between each one to allow your skin and subcutaneous tissue to return to normal. Be sure to take the measurement at the same place each time. Using just your waist circumference, your risk categories are:
Your hip measurement is taken at the widest part of your buttocks, again without pulling the tape too tightly and taking at least two measurements for accuracy. You get your ratio by dividing your waist measurement by your hip measurement. These are the waist-to-hip ratio norms:
Approaches to Addressing Belly FatAs I've written before, doing spot reducing exercises won't burn through subcutaneous or abdominal fat. You may build strong core muscles, but they'll still be hidden under subcutaneous fat. People use the term "spot reduction" to refer to the idea you can affect layers of fat in one area of the body by exercising muscles in that area. Visceral fat is more dangerous than subcutaneous fat but is also easier to gain and to lose. Along with practicing intermittent fasting and eating a ketogenic diet to support your mitochondrial health and weight loss efforts, these strategies may help you lose both subcutaneous and visceral fat: • Reduce stress -- Located on top of each kidney are your adrenal glands. Cortisol is a steroid produced by these glands related to your "fight or flight" response. When you're under chronic stress cortisol increases fat distribution to your abdominal area.18 Consider some of the steps in my article, "How Stress Affects Your Body, and Simple Techniques to Reduce Stress and Develop Greater Resilience." • Stay hydrated -- Drinking water may be one of the easiest ways to reduce psychological and physical stress. Your body is made of more than 60% fluid and your kidneys require fluids to flush toxins from your body. When you're dehydrated it affects the release of cortisol and alters metabolism.19 You'll know you're well hydrated by the color of your urine, which should be light straw-colored. • Quality sleep -- Maintaining adequate amounts of quality sleep will help you control stress. Loss of sleep may alter your production of hormones, including cortisol, and leave you vulnerable to the effects of daily stress. Sleep deprivation may lead to an increase in cortisol20 leading to a compromised immune system and disruption in metabolism and cognitive impairment. • Control insulin level -- Your body produces insulin in response to eating carbohydrates, which works with cortisol to help regulate your blood sugar levels.21 By reducing your carbohydrate intake you'll reduce your insulin secretion and may help reduce the accumulation of visceral fat. • Optimize vitamin C -- Vitamin C offers resilience against stress22 and plays a role in stabilizing blood sugar, which contributes to the production and release of cortisol. When you eat multiple servings of vegetables and fruit each day, you help maintain your levels of vitamin C. Remember, fresher produce tends to have higher concentrations of vitamins. from http://articles.mercola.com/sites/articles/archive/2020/04/30/effects-of-visceral-fats.aspx During the COVID-19 pandemic, many are asking how they can strengthen their immune system to reduce the potential of getting sick, and how they can support their body if they have a viral infection. As Dr. Roger Seheult explains in this video, natural killer cells are part of your immune response. While there is no known drug or medication that kills a virus, there are nutraceuticals that have an effect on them. Some of the nutraceuticals support your immune system, while others have the ability to reduce your viral load, as discussed by Mark McCarty and James DiNicolantonio.1 Solar ultraviolet-B radiation2 and supplemental vitamin D3 have also been shown to reduce pandemic fatality rates; this makes sense considering how important vitamin D is for controlling infections and lowering your risk for influenza and the common cold. How Your Body Uses Natural Killer CellsNatural killer cells are part of a larger group of cells called lymphocytes. These play a key role in your immune response and defense against viral infections. Inside the cytoplasm of natural killer cells are lytic granules,4 such as granulysin, perforin and granusyme A and B.5 Natural killer cells work by recognizing stressed cells and then using cytotoxic abilities to kill the abnormal cell.6 Once recognized, natural killer cells secrete the granules into a synapse delivering the granules to a target cell. These then trigger apoptosis in the infected cell. Defects in this system are related to fatal diseases,7 such as Griscelli syndrome type 2.8 This rare, inherited condition affects the immune system, leaving individuals prone to recurrent infections. Natural killer cells control infection by limiting tissue damage and spread and they help control tumor growth by limiting the spread of abnormal cells.9 They also regulate cells engaged with macrophages, T cells and endothelial cells. Additionally, they can mediate the immune response. As Seheult explains in the video, natural killer cells are part of the innate immune system, which is the first line of defense against pathogens.10 The next step is adaptive immunity, also called acquired immunity. This response is specific to the pathogen that enters your body. When you build up an immunity to a pathogen, it is the function of your adaptive immune response. A Forest Walk May Boost Your Body’s Ability to Fight VirusesScientific evidence shows that walking in a forest, also called forest bathing, can help enhance your natural killer cell activity, including the number of cells and the length of activity. Research has been done in men and women involving field trips to the forest. In this first study,11 researchers engaged 12 healthy men who normally worked at large companies in Tokyo. The participants were taken on a three-day, two-night trip to three different forests. On the first day, they walked for two hours; on the second day they walked for two hours both in the morning and afternoon; and on the third day they left for home. Blood was drawn in the morning before any intervention and after the first and second days of walking. The study team analyzed natural killer cell activity and the proportion of lytic granules and natural killer cells. On the last day, 11 out of 12 of the subjects had 50% higher activity compared to their levels before entering the forest. The researchers believed:12
Later, the same team performed the same intervention on 13 healthy women.13 Blood and urine samples were also collected seven days and 30 days after the trip was completed. The team also measured concentrations of phytoncides in the forest, which are airborne chemicals emitted by the plants. The results of this study showed natural killer cell activity remained raised for more than seven days, as did the number of natural killer cells and the “levels of intracellular anticancer proteins.” The team questioned whether the effects on the natural killer cells was representative of being outdoors, due to exercise or related to the trees. They designed and executed another study14 with two groups of men who visited two different forests or a city for three days and two nights. The intervention was the same with blood drawn and urine samples collected before the study began, each day and on Days 7 and 30 after the intervention was complete. During this study they also measured the phytoncides in the forest and the city. As you might expect, measurements in the forest were high, but in the city, most levels were so low they couldn’t be measured. The researchers concluded:15
Can You Repeat These Results at Home?Once the researchers had identified phytoncides as the probable reason individuals were experiencing a higher measure of natural killer cell activity, they designed a follow-up study.16 In this they attempted to recreate the boost in natural killer cells using essential oils from trees. They engaged 12 healthy men who stayed in a city hotel for three nights between 7 p.m. and 8 a.m. In the morning they returned to work in the city. During the night, researchers ran a humidifier with stem oil from the hinoki cypress tree. “Blood samples were taken on the last day and urine samples were analyzed every day during the stay,” they reported. Phytoncide measurements in the room were also taken. The study team found there was a statistically significant jump in natural killer cell activity after sleeping in the hotel room, despite the fact they returned to work in the city each day. Urine was analyzed for adrenaline and noradrenaline, since the presence of adrenaline reduces the number of natural killer cells. Although there was a statistically significant difference in the measurement of adrenaline in the urine of those who stayed in the forest,17 the same difference did not occur in all who stayed in a hotel with stem oil diffused in the room.18 When the data were analyzed together, there wasn’t a statistically significant drop in the excretion of adrenaline in the urine. However, when the researchers separated the samples into those where the adrenaline increased and those where it decreased, there was a statistically significant difference in the reduction of adrenaline in the urine. They concluded that, while there was beneficial activity to short-term exposure, prospective studies in people exposed to phytoncides long-term would be needed to confirm the effect. You Also Benefit From Green SpacesIf you don't have a local forest, you can still benefit from exposure to green spaces. In one meta-analysis of 143 studies,19 scientists noted statistically significant reductions in blood pressure, heart rates and levels of cortisol secretion measured in saliva. They also identified decreased incidences of diabetes and all-cause and cardiovascular mortality. The researchers from the University of East Anglia20 analyzed studies looking at postoperative recovery time. In all, there were 290 million participants across all 143 studies from 20 different countries. When they correlated the amount of time individuals had spent in green areas with 100 health measurements, they also found that women who were pregnant had a reduced risk for preterm birth and a lower risk of delivering a baby who was small for gestational age. The relationship may be related to a higher level of physical activity that often comes in green spaces. It could also have something to do with social interaction or greater exposure to sunlight. The researchers concluded:21
Develop Habits to Support Your Immune SystemDeveloping healthy habits is important to support your immune system, reduce the potential for viral infections and lower your risk of chronic disease. While there are multiple choices you make each day, the following factors are foundational to creating a strong health plan. • Gut microbiome -- Your gut microbiota is key to your immune system and digestive health. Fermented food and fiber are vital to repopulating your gut with beneficial bacteria and providing the necessary nutrients for them to thrive. • Exercise -- Research evidence underscores the benefits of exercise to your immune health. Seek to raise your heart and breathing rate for 30 minutes each day in addition to moving out of your chair frequently. Your body requires both exercise and movement to stay healthy. • Sleep -- The quality and quantity of your sleep has a regulatory effect on your immune system.22 Developing good sleep habits requires just a little effort. If you struggle with getting to sleep or staying asleep, consider the tips I share in “Top 33 Tips to Optimize Your Sleep Routine.” • Vitamin D -- This is another powerful component to supporting your immune system and the prevention and treatment of viral infections, including COVID-19. To read more about maintaining appropriate levels and how it may help reduce your risk of COVID-19, see “Vitamins C and D Finally Adopted as Coronavirus Treatment.” from http://articles.mercola.com/sites/articles/archive/2020/04/29/forest-bathing.aspx A curious thing is happening amid the COVID-19 pandemic: As COVID-19 cases and deaths mount, hospital admissions for other acute ailments are markedly dropping. In an April 6, 2020, New York Times article, Dr. Harlan Krumholz — professor of medicine at Yale and director of the Yale New Haven Hospital Center for Outcomes Research and Evaluation — notes:1
Drastic Reduction in Emergency AdmissionsIn an informal Twitter poll, created by Angioplasty.org, an online community of cardiologists, 45.4% reported a 40% to 60% reduction in hospital admissions related to heart attacks, and 22.4% reported a reduction greater than 60%.2 Other emergencies, including acute appendicitis and gallbladder disease have also dropped, according to unofficial reports from medical professionals.3 What’s more, according to Krumholz:4
We still do not have an explanation for these statistics. Krumholz hypothesizes that patients may be avoiding face-to-face medical care for fear of contracting COVID-19. If this is the case, their condition may significantly worsen, and lives may be unnecessarily lost.
This isn’t the only possibility, however. As Krumholz notes, natural triggers of heart attacks and strokes may simply have been removed by the imposed social distancing, eating at home and having more time for physical activity. He’s not convinced that this theory is the most likely explanation, though, considering respiratory infections tend to increase the risk of heart attack. The fear and stress of the situation should theoretically also have led to an increase in heart attacks, as depression, anxiety and frustration “are all associated with a doubling or more of heart attack risks.”5 Delaying Necessary Care Could Cost YouThe same story is also reported in an April 19, 2020, article6 in The Washington Post, which notes that:
All-Cause Mortality Is Still UncertainWhatever the reason for the drastic decreases in hospital admissions for ailments other than COVID-19, time will tell whether the decrease has actually resulted in increased all-cause mortality or not. As reported by The Washington Post:7
Some do claim all-cause mortality has risen during this pandemic. According to an April 14 report by The New York Times:8
The New York Times’ claim that the deaths occurred as a result of COVID-19 “overwhelming the health care system” seems suspect, however, in light of so many doctors saying their hospitals are nowhere near capacity. These conflicting reports show just how difficult it is to tease out the truth without proper data collection and distribution. Without accurate and complete data, it’s virtually impossible to draw any definitive conclusions. Is Mortality Actually Going Down?Two interesting graphs created by I. Ratel9 — who freely admits he’s not a statistician or doctor but has degrees in industrial management and automotive technology and whose interest in this is fueled by the fact that he’s immunocompromised — suggest a downturn in both pneumonia deaths and all-cause mortality. Although final data won’t be released until 2021, I did find in my own research that pneumonia deaths in the current flu season (2019-20) are down compared to 2018-19,10 so I’m including Ratel’s calculations here for anyone interested in diving deeper into his data gathering. Ratel explains the graphs:11
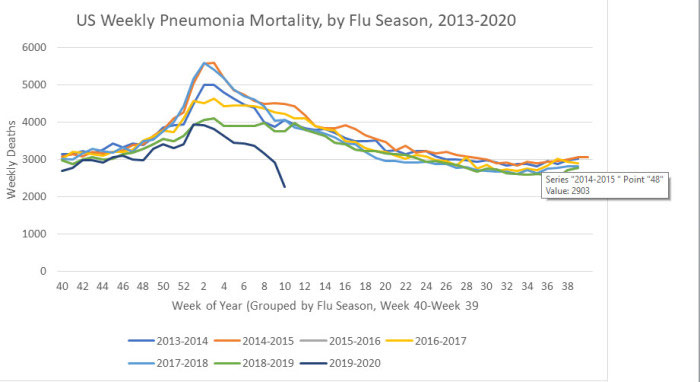
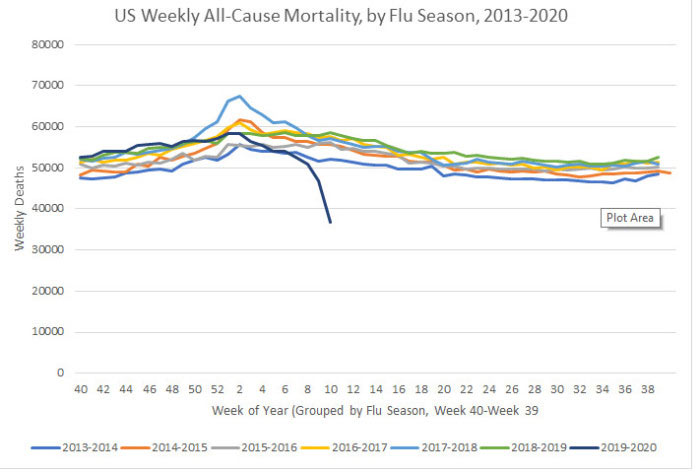
Avoiding Hospitals Might Lower Death TollThat said, previous research has shown that when conventional medical intervention is reduced, mortality often goes down. For example, back in 2000, all-cause mortality in Israel dropped during a time when Israeli doctors at public hospitals went on strike.12 One of the reasons for this is because medical care itself tends to be a risky business. Research13 published in 2014 found nearly 1 in 5 elderly Medicare patients are injured by their medical care. The most common medical injuries included receiving the wrong medication, having an allergic reaction to medication given, and receiving treatment that led to more complications. As a result of these injuries, they also had a death rate nearly double those who were not injured by their care. Other research14 published in 2013 concluded 210,000 Americans are killed by preventable hospital errors each year, and when deaths related to diagnostic errors, errors of omission, and failure to follow guidelines were included, the number skyrocketed to an estimated 440,000 preventable hospital deaths each year. One in 25 patients in the U.S. also contracts some form of infection while hospitalized, and an estimated 205 Americans die from hospital-acquired infections every day. The unfortunate truth is that once you’re hospitalized, you’re immediately at risk for medical errors that might cost you your life. That’s not to say you should never go to the hospital, though. If you suspect you’re having a heart attack, stroke or appendicitis, for example, you should seek immediate care. Many other ailments that people seek treatment for, however, may simply place them at increased risk for complications. The difficulty is determining what you might be able to address at home and what’s an actual emergency. If you have access to a holistic physician you trust, calling them for a consultation would be a good idea. COVID-19 Deaths Jump Due to ReclassificationWhile other ailments appear to have declined (at least based on hospital admission rates, which may present a false picture of the situation), COVID-19 deaths in the U.S. have undergone a sudden jump mid-April. While some use this as a sign that the infection is spreading and perhaps more lethal than suspected, the real reason for this sudden jump is simply the reclassification of COVID-19 deaths to include “probable” cases. While the U.S. Centers for Disease Control and Prevention15 separates confirmed COVID-19 deaths from all-cause mortality, pneumonia deaths, influenza deaths and deaths with both pneumonia and COVID-19, it has issued guidance to states on how to document COVID-19 deaths on death certificates, indicating that COVID-19 should be indicated if “the disease caused or is assumed to have caused or contributed to death.”16 By not requiring COVID-19 deaths to be laboratory confirmed, the death rate can easily become skewed. New York City has officially transitioned its record keeping to include suspected COVID-19 cases,17,18 and as you’d expect, when suspected or “probable” deaths are counted without any proof that SARS-CoV-2 infection was involved at all, the numbers dramatically increase. Ultimately, there is no way to tell what the real impact of the pandemic actually is when using this system. Looking at the data19 collected for NYC between March 11, 2020, and April 13, 2020, 23.5% of deaths involving residents between the ages of 45 and 64 are in the “probable” category, as are 23.6% of those among 65- to 74-year-olds and 49.9% of those over the age of 75. As noted by The New York Times20 on April 14, 2020, New York City’s addition of thousands of “probable” cases increased the alleged death rate from COVID-19 by 17% overnight. 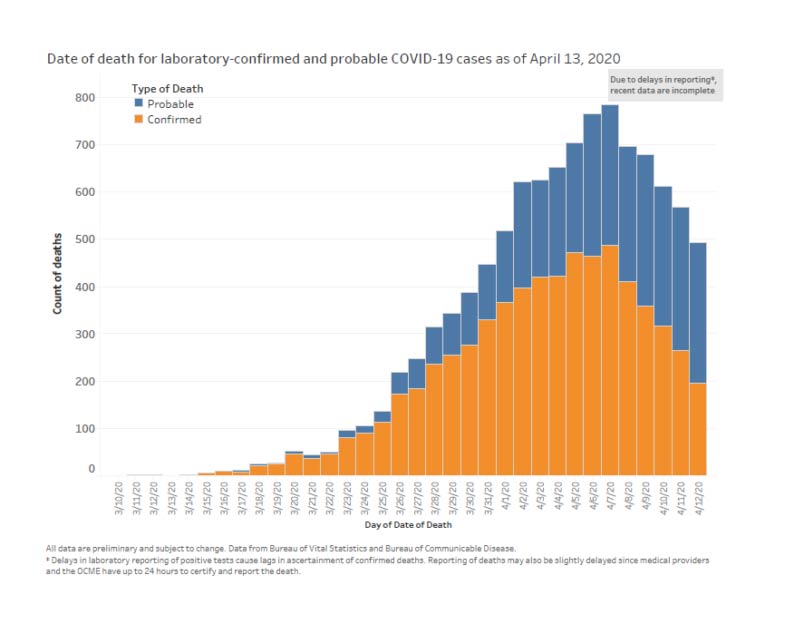
Signs of Suicide Epidemic EmergeWhether all-cause mortality is in fact going up or down, as predicted we are now starting to see a rise in suicides. Suicide statistics reliably follow economic trends, with financial downturns triggering higher rates of depression and despair. According to an updated March 27, 2020, report by The Sacramento Bee:21
According to a spokeswoman for the national Crisis Text Line, text conversations were double that of the normal volume during the week of March 15.22 Google also reports that searches for “panic attack symptoms” have doubled compared to last year.23 The CDC, meanwhile, appears to take things in stride, noting that “Fear and anxiety about a disease can be overwhelming and cause strong emotions in adults and children,” but that “Coping with stress will make you, the people you care about, and your community stronger.”24 While true as a general statement, the current pandemic has delivered a perfect storm of challenges that is sure to bring many to a breaking point. We’re not just talking about fearing a disease. We’re also talking about the very real challenges of keeping a roof over our heads and feeding ourselves and our families when the entire country has been shut down and millions of workers have been laid off. According to reports by The Federalist25 and Red State,26 suicides exceeded COVID-19 deaths in Tennessee the week of March 20. The Regional Forensic Center in Tennessee was investigating nine suicides as of March 27, eight of which took place in Knox County — one of the few areas in Tennessee where businesses were ordered to close. The suicides, which occurred within a 48-hour period, account for 10% of the 2019 suicide rate for the region.27 Meanwhile, only six patients died from COVID-19 in the entire state that week. In a statement, Knoxville, Tennessee Mayor Glenn Jacobs said:28
Similar warning signs are starting to be noted in other states as well, including Oregon. In a March 24 local news report,29 Portland police chief Jami Resch said suicide threats or attempts are 41% higher now than this time last year, and there’s been a 23% increase since the 10 days before a state of emergency was declared in Portland. Unfortunately, this is likely the beginning of what is most certainly only going to worsen with time, as many financial experts are predicting a depression worse than the Great Depression of the 1930s.30 Suicide Prevention ResourcesClearly, we’re facing an unprecedented challenge, and it’s hard to know exactly what the right thing to do is. There are risks and benefits to every choice. However, I’ve argued since the very beginning that ignoring the human cost of economic collapse is a serious mistake. It’s an equally serious mistake to spread fear unless fear is truly warranted. Mainstream media have a lot to answer for in this regard. While the future is certainly unsure, I urge you to do what you can to keep yourself on an even keel going forward. Do your best to moderate your fears. And, if you need help, don’t hesitate to reach out to family, friends or any of the available suicide prevention services:
from http://articles.mercola.com/sites/articles/archive/2020/04/29/coronavirus-mortality.aspx As the world deals with the scope of the COVID-19 pandemic, scientific articles have zeroed in on who is most vulnerable to the virus. It appears those who are elderly, overweight and suffer from an underlying health condition like diabetes or high blood pressure are most at risk. But the consumption of ultraprocessed food is increasingly seen as a risk factor for contracting COVID-19, too. Ultraprocessed foods increase the risk of conditions like obesity, cancer, Type 2 diabetes, cardiovascular disease and gallstones, which make you more vulnerable to illnesses like COVID-19. In fact, eating over four servings of ultraprocessed foods daily increased the risk of premature death by 62% in a 2019 study.1 When it comes to fighting off COVID-19, ultraprocessed foods pose another health danger: They compromise the gut microbiome, which has a crucial role in your body’s immune response to infection and in maintaining overall health. Even before the virus that causes COVID-19 surfaced, ultraprocessed foods were a bad idea but during the current pandemic they are especially dangerous. Beware of Ultraprocessed FoodsWhat are ultraprocessed foods, sometimes referred to as UPFs? According to the NOVA Food Classification system, designed by the Center for Epidemiological Studies in Health and Nutrition, they are:2
Ultraprocessed foods, aggressively marketed by giant food producers for their profitable potential, constitute around 25% to 60% of daily energy intake in many countries, according to Science Daily. They include:3
While it is tempting to dismiss the dangers of UPFs by saying that all foods, to some extent, are "processed," food writer Bee Wilson says that is not the case:4
Moreover, cautions Wilson, food giants deliberately mislead consumers. When fat was misleadingly considered the cause of obesity, she says, the food industry rolled out low-fat products. When sugar became the culprit, food giants manipulatively marketed artificially sweetened drinks.5 UPF manufacturers have also launched successful campaigns to convince the public that obesity is not caused by their products, but by lack of exercise. Coca-Cola is among them, and, toward that end, has provided funding to universities and a wide spectrum of medical groups including the American Heart Association, the American Lung Association, the American College of Cardiology and the American Academy of Pediatrics.6 You can't help but wonder if that is why Harvard Medical School/Partners in Health, a recipient of Coca-Cola funding, writes this about obesity:7
Obesity is increasingly linked to serious cases of COVID-19 that require hospitalization, even among young people, according to The New York Times.8 The reasons are not entirely clear, but abdominal obesity can cause compression of the lungs and diaphragm, which impairs breathing ability. Other factors that could explain the link between obesity and serious cases of COVID-19 could include pre-existing respiratory conditions, a greater amount of circulating, pro-inflammatory cytokines and low-grade inflammation, which are all correlated with obesity. Almost 80 million Americans — 42 percent of the population — are obese.9 A report released by the Intensive Care National Audit and Research Centre on 196 patients critically ill with COVID-19 found 56 patients had a body mass index (BMI) of 25 to 30, which is classified as overweight.10 Fifty-eight had a BMI of 30 to 40, which indicates obesity, and 13 had a BMI of 40 or higher, which is severely obese. In the study, 71.7% of the critical patients were overweight, obese or severely obese.11 Ultraprocessed Food Impairs the MicrobiomeTwo studies published by The BMJ in 2019 cast ultraprocessed food as a threat to global public health. In a linked editorial, Australian researchers add that the negative effects of UPFs on the gut microbiome must be explored.12 Science has increasingly revealed the huge effect of diet on the human microbiome and its ability to ward off disease. The more diverse with healthy microorganisms a microbiome is, the better it supports the immune system, according to Tim Spector, professor of genetic epidemiology at King's College in London — especially as COVID-19 has spread all over the world. Writing in The Conversation, Spector says:13
Fermented foods and probiotics are the best route to optimal microbiome health, if they are traditionally made and unpasteurized. Healthy fermented choices include lassi (an Indian yogurt drink), fermented, grass fed organic milk (kefir), fermented soy or natto and different types of pickled fermentations of cabbage, turnips, eggplant, cucumbers, onions, squash and carrots. Unless antibiotics are absolutely necessary, they should be avoided and, if avoidance is not possible, counteracted with fermented food and probiotics. Be aware that conventionally-raised meats are also a source of antibiotics because animals are routinely fed the medications. Genetically engineered grains and chlorinated and/or fluoridated water can also destroy gut flora. UPFs Have Put Millions at Risk for COVID-19Ultraprocessed food is designed to be sensually appealing, hyperpalatable and habit-forming, thanks to additives, crafty packaging and marketing and "convenience." Yet UPFs fill you up without the vitamins, minerals, live enzymes, micronutrients, healthy fats and high-quality protein your body needs. UPFs increase how fast people eat and delay how "full" they feel, causing obesity and metabolic dysfunction. Dr. Aseem Malhotra is an honorary consultant cardiologist at Lister Hospital in Stevenage, England.14 According to an article he wrote in European Scientist, UPFs cause:15
Kristin Lawless, author of the book, "Formerly Known As Food: How the Industrial Food System Is Changing Our Minds, Bodies, and Culture," also sees correlations between metabolic dysfunction and succumbing to COVID-19:16
While the millions who suffer from metabolic syndrome from UPFs are not seen as urgent like COVID-19 is, the problems are one and the same, according to Malhotra. Governments, in addition to telling people to stay home to save lives during the COVID-19 pandemic, should address diet, he asserts. He writes:17
UPFs Are Especially Harmful to Poor CommunitiesPeople living in poverty, whether in developing or advanced countries, are especially vulnerable to health problems from ultraprocessed foods and COVID-19. According to Malhotra:18
Even before the COVID-19 pandemic, food giants have targeted those with low incomes with aggressive marketing of UPFs. Following initiatives by Brazil to fight the trend, Ecuador, Uruguay and Peru have urged citizens to avoid UPFs in favor of natural foods.19 Food deserts further the dietary exploitation of the poor, according to Lawless:20
The USDA defines a food desert as a low-income tract where many residents do not have easy access to a supermarket or large grocery store.21 In addition to a lack of food outlets offering healthy food, residents' lack of transportation to get to stores is a big factor. Residents who have to walk with their groceries or take the bus can carry fewer groceries, and transporting perishable items is especially difficult. According to the USDA, many types of organizations like businesses, local governments and nonprofits are eligible for assistance to address the problems created by food deserts.22 However, like discouraging the consumption of UPFs, such changes take time and certainly will not occur during the COVID-19 pandemic. Other Environmental Causes of COVID-19A diet of UPFs puts people at risk for COVID-19 because of the metabolic, immune system and microbiome degradation it causes. But the coronavirus pandemic also has environmental causes and repercussions, says Lawless:23
Whether people whose vulnerability to disease has been increased by Big Agriculture or viruses spread from its excesses, most experts agree we need a radical overhaul of the entire food production and distribution system. According to Lawless:24
If ever there were a time to consider our eating habits and the domination of harmful agricultural systems it is during this coronavirus pandemic. from http://articles.mercola.com/sites/articles/archive/2020/04/29/ultraprocessed-food-makes-you-vulnerable-to-covid-19.aspx Dr. Anthony Fauci, director of the National Institute for Allergy and Infectious Diseases (NIAID) told Americans on April 1, 2020 that modeling reports suggested COVID-19 infections could eventually "kill 100,000 to 240,000 Americans,"1,2,3 which was considerably less than the worst case 1.7 million mortality figure the U.S. Centers for Disease Control and Prevention (CDC) talked about on March 13,4 and a fraction of the doomsday 2.2 million mortality figure projected by a scientist at Imperial College London.5,6 The next day, Fauci called for an all-state nationwide lockdown7 and CDC officials instructed Americans to cover their faces with cloth masks if they have to leave their homes to buy food or seek medical care.8 On April 6, University of Washington modeling experts, who influenced the setting of current federal and state "social distancing" policies, lowered U.S. COVID-19 mortality estimates from the worst case 162,000 fatalities they predicted on March 26 to about 82,000 deaths.9,10 Two days later, on April 8, they lowered U.S. mortality estimates even further to 60,415 deaths by August 4, but included the caveat "assuming full social distancing through May 2020."11 With the U.S. economy in meltdown, Dr. Fauci warned that, until a COVID-19 vaccine is available, we have to prepare for a new normal. He said:12
COVID-19 Deaths by the NumbersBy April 12, 2020, there had been nearly 22,000 COVID-19 related deaths reported in the U.S. population of 325 million people and over 110,000 deaths in a global population of 7.8 billion people.13 According to the CDC, most cases are asymptomatic or mild, including in children,14 unless an individual has an underlying chronic health problem like asthma, obesity, diabetes, autoimmunity, immune suppression, high blood pressure, chronic obstructive pulmonary disease (COPD) or heart disease.15,16,17,18 There are large mortality variations among different countries and similar wide variations in mortality among populations living in different states in the U.S.19 At least one study published on April 5 has found that air pollution subjecting individuals to long term exposure to fine matter particulates greatly increases the risk for death from COVID-19, noting that, "The majority of the pre-existing conditions that increase the risk of death for COVID-19 are the same diseases that are affected by long-term exposure to air pollution."20 A small increase in long-term exposure to PM2.5 [fine particulate matter] leads to a large increase in COVID-19 death rate, with the magnitude of increase 20 times that observed for PM2.5 and all-cause mortality. The study results underscore the importance of continuing to enforce existing air pollution regulations to protect human health both during and after the COVID-19 crisis. A March 30 report in The Lancet estimated the overall case fatality ratio in China has been 1.38%, but is substantially higher in those over 60 years old.21 Recent published data from the CDC also confirms that mortality in the U.S. is much higher among senior citizens over age 65, rising to 10% to 27% for those over age 85.22 The CDC continues to state that individuals at higher risk for serious illness from COVID-19 infection are those over age 65 and "people of all ages with underlying medical conditions, particularly if not well controlled."23 US COVID-19 Mortality Statistics: Science or Assumptions?On March 24, the director of Division of Vital Statistics, National Center for Health Statistics (NCHS) operated by the CDC issued a COVID-19 memo alert with Q&A instructions informing doctors and coroners that "a newly-introduced ICD code [UO7.1 COVID-19] has been implemented to accurately capture mortality data for Coronavirus Disease 2019 (COVID-19) on death certificates." When determining the underlying cause of death listed on the death certificate, the memo states that:
CDC officials make it clear that on cases where the death certificate indicates uncertainty about the cause of death, there will likely be no follow up and the death will be listed as COVID-19:
Finally, answering the question, "Should COVID-19 be reported on the death certificate only with a confirmed test?" the CDC's memo emphasizes that lab confirmation of COVID-19 is unnecessary to list the cause of death as COVID-19 on the death certificate:
In an April 9 NBC Today Show interview, Dr. Fauci was asked whether some deaths are being falsely counted as COVID-19 deaths when they are really due to other causes. He replied:24
Economic and Social Meltdown ContinuesMore than two months after the World Health Organization (WHO) declared the outbreak of COVID-19 in China as a "Public Health Emergency of International Concern,"25 which was followed the next day by the CDC's January 31 declaration of a national Public Health Emergency in the U.S.,26 it appears that the government's pandemic planning efforts spanning four decades failed to prepare federal and state health agencies to respond quickly,27,28,29,30,31 despite federal legislation32 that ensured substantial annual congressional appropriations to the U.S. Department of Health and Human Services (DHHS) since 2006 for pandemic planning.33,34 Right now, COVID-19 testing kits are slowly rolling into the states but in limited quantities,35,36 and health care workers are continuing to report critical shortages of personal protective equipment (PPE) and medical supplies.37,38,39 With almost every state government following federal guidelines and either requesting or ordering residents to quarantine themselves at home — whether they are healthy or sick — families are facing unprecedented economic losses.40 On April 3, the U.S. Bureau of Labor Statistics (BLS) reported huge declines in employment in the leisure and hospitality industries — mainly in food and beverage — but also in health care, social assistance, professional and business services, retail trade, and construction.41 Unemployment in the U.S. rose by almost a full percentage point to 4.4%, the largest over-the-month rate increase since 1975, with the number of unemployed persons rising from 1.4 million to 7.1 million in March. The BLS report said the sharp unemployment increases reflects the "efforts to contain" the coronavirus in the U.S. Lower income families without savings and dependent upon hourly wages and part-time work in service professions are hit especially hard.42 Understaffed social service support systems are struggling to cope with significant increases in depression, spousal and child abuse, and calls to suicide hotlines.43,44,45 However, some scientists,46,47 doctors48 and politicians49 want quarantines to stay in effect beyond April 31, even though the managing director of the International Monetary Fund Kristalina Georgieva warned on April 9 that the economic fallout of shutdowns is approaching that of the Great Depression.50 We are still faced with extraordinary uncertainty about the depth and duration of this crisis. It is already clear, however, that global growth will turn sharply negative in 2020, as you can see in our World Economic Outlook. In fact, we anticipate the worst economic fallout since the Great Depression. Bill Gates Calls for 10-Week Nationwide ShutdownIn an OpEd in The Washington Post published March 31, Microsoft founder and philanthropist social reformer Bill Gates called for a nationwide federally enforced quarantine for all states that would last "10 weeks or more:"
Several days earlier in a TED interview, Gates talked about how the strict social distancing and quarantine measures in place in the U.S. are designed to prevent a majority of the U.S. population from being infected with and recovering from COVID-19, which confers natural immunity and contributes to herd immunity in human populations. He also stated there will be a need for people to have "certificates" that prove they have either recovered from the infection or have been vaccinated once a vaccine is produced. He said:53
Fauci Agrees: COVID-19 Natural Herd Immunity Not WantedAt a White House briefing of the Coronavirus Task Force held April 6, Dr. Fauci confirmed that strict social distancing and quarantine measures are at least partially in place to prevent populations from developing natural herd immunity. He said:54
In an April 9 interview on National Public Radio (NPR), Bill Gates returned to the message that some "social distancing" measures have to stay in place "until we get a vaccine that almost everybody's had." He said:
Governments Make Fast-Tracked COVID-19 Vaccines Main PriorityImmediately after the January 30 WHO declaration that a novel coronavirus outbreak in China posed a "public health emergency of international concern," press releases were issued by the Gates Foundation55 and World Health Organization (WHO)56 informing the world that experimental coronavirus vaccines already in development would be put on a fast track to licensure for global use. On March 9, WHO released its COVID-19 R&D roadmap that, according to BioWorld, had been endorsed by "400 experts" and included funding from the European Commission (37.5 million euros), German government (10 million euros) and an additional 46 million euros from the U.K. government, with 20 million euros going directly to the Coalition for Epidemic Preparedness (CEPI) for vaccine development. CEPI committed $100 million to speed up licensure of COVID-19 vaccines but said it was trying to raise $2 billion more to speed vaccines to market.57 The WHO's R&D plan stated there was an "urgent need" to fill in scientific knowledge gaps about the "basic biology" of COVID-19 infection and clinical evolution of COVID-19 and its epidemiology, as well as the need to develop appropriate animal models for research because some previous SARS and MERS vaccine studies in animals showed enhanced respiratory disease can occur in vaccinated animals after exposure to the live virus. The WHO roadmap stated, "Evaluating the potential for enhanced disease in humans is critical before [vaccines] can be assessed through larger-scale studies."58 By mid-March and early April, the WHO, National Institutes of Health,59 universities,60 and global pharmaceutical corporations61 had announced development of more than 50 experimental COVID-19 vaccines.62,63 Using vitamin and supplement therapies or currently licensed prescription drugs64,65,66,67,68,69 has taken a back seat to an aggressive push to keep restrictive "social distancing" measures in place until fast tracked experimental vaccines are licensed.70,71,72 Maintaining that the only solution to dealing with the new coronavirus is universal use of a new vaccine,73,74 this single solution approach guarantees even bigger profits in the exploding global vaccine market that has doubled over the past decade from $20 billion in 201075 to $42 billion in 2018.76 Dominated by the U.K.'s GlaxoSmithKline, France's Sanofi and U.S. drug giants Merck and Pfizer, the vaccine market is projected to double again by 2026 to over $93 billion.77 There are already reports from Wall Street predicting big gains in biotech stocks based on multiple companies developing COVID-19 vaccines and new drugs.78 One company, Moderna, which is partnering with the National Institute of Allergy and Infectious Diseases (NIAID) headed by Dr. Fauci, has seen a 78% increase in its stock price since it announced in February that its experimental messenger RNA vaccine was ready for clinical trials.79 The company's CEO has become a new billionaire overnight.80 Big Pharma Getting More Money to Deliver COVID-19 VaccinesResponding to the call by public health officials to lockdown the U.S. with in-home quarantines, Congress passed the CARES Act signed into law on March 27, 2020 that will cost American taxpayers over $2 trillion. The federal legislation includes $27 billion for development of COVID-19 vaccines, drug therapies and purchase of pandemic medical supplies. The legislation did not include a cap placed on how much money drug companies can charge and profits they can make on the COVID-19 vaccines and drug therapies they develop with the use of money from the government. Already, there are questions being raised about just how far the price gouging will go when those COVID-19 drugs and vaccines are licensed by the FDA and recommended by the CDC.81 On March 30, the DHHS Assistant Secretary of Preparedness and Response announced that the government is taking steps to "speed the development and manufacturing of vaccines to prevent COVID-19."82 The same day, Johnson & Johnson issued a press release stating that the Biomedical Advanced Research and Development Authority (BARDA) had awarded J&J's Janssen Pharmaceutical Companies $1 billion to establish new U.S. vaccine manufacturing capabilities and additional production capacity outside the U.S and produce a global supply of more than 1 billion doses of the COVID-19 vaccine using AdVac® and PER.C6® technologies.83 J&J plans to initiate human clinical studies in September 2020 and deliver the first batches of vaccine for emergency use authorization in early 2021.84 BARDA was created by Congress in 2006 under the Pandemic and All Hazards Preparedness Act,85 legislation that has given billions of dollars to DHHS since then to develop "bioterrorism" and pandemic influenza vaccines.86 That federal legislation also removed all civil liability from pharmaceutical companies for injuries and deaths caused by vaccines and drugs manufactured in response to declared public health emergencies, such as pandemics.87 According to a March 30 Reuters report, Moderna, Inc. "also signed a deal with the Biomedical Advanced Research and Development Authority (BARDA), part of the DHHS. The arrangements are part of the federal government's effort to encourage drugmakers to be able to produce massive amounts of COVID-19 vaccines even before any are proven to work."88 Earlier in March, the NIAID headed by Dr. Fauci issued a press release on March 16 announcing that a Phase1 human clinical trial conducted by Kaiser Permanente Washington Health Research Institute in Seattle has begun to evaluate an experimental mRNA vaccine for COVID-19 (mRNA-1273) co-developed by NIAID scientists and scientists at Moderna, Inc, based in Cambridge, Massachusetts. The Coalition for Epidemic Preparedness (CEPI) helped fund the manufacturing of the vaccine for the Phase 1 clinical trial.89 Moderna and NIAID are conducting human trials of the experimental mRNA-1273 COVID-19 vaccine without first conducting animal trials, which has always been an important part of the vaccine licensing process.90 On March 30, Moderna stated that its COVID-19 vaccine might be ready for emergency use in some people, including healthcare workers, by the fall of 2020:91
An April 3 Philadelphia Inquirer article trumpeting that "Coronavirus has created a new golden age for vaccines and Philly is at the heart of it,"92 pointed out at least part of the heavy financial investments the U.S. government has made in vaccine development through BARDA since 2006:
Experimental COVID-19 Vaccines Using Eight Different PlatformsCoronaviruses are a group of diverse, single-stranded, enveloped RNA viruses that cause a wide range of respiratory, gastrointestinal and neurologic illnesses with varying severity in animals and humans. Most coronaviruses, including those causing the common cold, are not associated with significant mortality, with the exception of Severe Acute Respiratory Syndrome (SARS-CoV), which emerged in China in 2002, and the coronavirus causing Middle East Respiratory Syndrome (MERS-CoV), which was identified in Jordan and Saudi Arabia in 2012.93 COVID-19 is referred to in the medical literature as severe acute respiratory syndrome coronavirus 2 (SARS-CoV2) or COVID-19.94 Drug companies and government agencies racing to be the first to license a COVID-19 vaccine, are using different technology platforms to create experimental vaccines: inactivated virus; attenuated virus; protein subunit; virus-like particle, DNA, RNA and non-replicating vector.95 Traditional vaccines contain attenuated or inactivated viruses and bacteria or proteins, as well as adjuvants, such as aluminum, to stimulate an immune response that produces artificial immunity. For example, older viral vaccines for smallpox and measles vaccine contain live attenuated viruses; injectable influenza vaccines contain inactivated viruses; the recombinant hepatitis B virus vaccine is a protein subunit vaccine, while the newer human papillomavirus (HPV) virus vaccine contains virus like particles. For the past two decades, researchers have been experimenting with new technology platforms, notably ones that introduce foreign DNA and RNA into cells of the body, to develop experimental vaccines for SARS, MERS, HIV and other diseases but, so far, none have been proven effective and safe for humans.96 DNA and mRNA Vaccines: Flying Blind Into Uncharted TerritoryGene-based vaccines encode a viral protein from a pathogen (like COVID-19) in human DNA or mRNA. DNA vaccines deliver pieces of DNA into human cells to stimulate the immune system to create antibodies specific to pathogenic proteins without causing disease. DNA vaccines require no culture or fermentation for production and no refrigeration after production because they are made in a lab using synthetic processes, and can be produced in large quantities for less money than traditional vaccines.97 Messenger RNA (mRNA) vaccines inject human cells with mRNA, usually within lipid nanoparticles, to stimulate cells in the body to become manufacturers of viral proteins.98,99 In March 2020, a virologist at Imperial College London told Chemistry World that one advantage of using mRNA technology to make vaccines for humans is that, "Rather than generating proteins in a manufacturing plant and purifying them, you are getting the muscle to do the job and make the protein itself."100 Like DNA vaccines, mRNA vaccines can be produced in the lab using faster and less expensive process than traditional vaccines. RNA vaccines can be delivered with syringes, nasal spray or needle-free into the skin (patches). Although neither DNA or mRNA vaccines have been tested in large-scale clinical trials, an April 3 article in Chemical and Engineering News highlights the breakneck speed at which COVID-19 vaccines "are moving new technologies from the computer and into the clinic at an unprecedented rate." What should be separate pre-licensure phases for proving safety and effectiveness — preclinical animal models, clinical testing, and manufacturing — are now "happening all at once."101
But will spending lots of money to cut corners and speed up licensing of COVID-19 vaccines using experimental DNA and mRNA technology — or other types of new technology — end up putting millions of people at risk for vaccine failures and reactions leading to chronic illness? There are nagging questions about DNA102 and mRNA103 vaccine platforms and they are not trivial. According to a 2011 article in Harvard College Global Health Review, DNA vaccine safety concerns include such potential side effects as:104
According to researchers at University of Pennsylvania and Duke University, mRNA vaccines also have potential safety issues:105
Top COVID-19 Vaccine Candidates Being TestedFollowing is a selection of companies identified by MarketWatch that are among those leading the race to be the first to get a COVID-19 vaccine licensed for global use:106,107
from http://articles.mercola.com/sites/articles/archive/2020/04/28/covid-19-windfall-for-pharma-meltdown-for-families.aspx The symptoms of COVID-19 — fever, cough, shortness of breath, chills, muscle pain — are widely reported via the media and public health organizations. Less publicized, however, is the fact that a sizable number of people with COVID-19 do not experience symptoms at all. Even the U.S. Centers for Disease Control and Prevention (CDC), in their about-face regarding the usage of masks to slow the spread of COVID-19, stated, "We now know from recent studies that a significant portion of individuals with coronavirus lack symptoms ("asymptomatic") …"1 One of those studies found that in a family of three who had all tested positive, only one — a 35-year-old man — had symptoms. The other two family members, a 33-year-old woman and 3-year-old boy, were asymptomatic.2 Since widespread testing hasn't been done in the U.S., and most of those who have been tested had symptoms, it's largely unknown how many people may have already had, and recovered from, COVID-19 but didn't know it because they didn't have symptoms. The few studies that have been done toward this end, however, are providing revealing data showing that 87.9% of one group that tested positive had no symptoms.3 Majority of Pregnant Patients With COVID-19 Had No SymptomsA hospital in New York City began universal screening for SARS-CoV-2, the virus that causes COVID-19, among pregnant women admitted for delivery. Between March 22, 2020, and April 4, 2020, 215 were screened on admission for symptoms of COVID-19 and tested for the virus. Only four of the women had fever or other COVID-19 symptoms, and all four tested positive. Of the remaining women who were tested even though they had no symptoms, 13.7% — 29 — were positive. This means that, overall, 87.9% of the 33 women who tested positive for SARS-CoV-2 had no symptoms.4 Among those who tested positive without symptoms, three women (10%) developed fever before they were discharged from the hospital (within about two days). However, two of these women were treated for endomyometritis, a pregnancy complication that causes fever, while only one was presumed to have developed a fever due to COVID-19. In one additional woman who had initially tested negative, symptoms developed after delivery and she tested positive three days after the initial test. The study authors explained:5
Study co-author Dr. Dena Goffman, with the Columbia University Irving Medical Center, told CBS News, "If we're not checking, we really do risk missing people who are carrying the virus."6 And therein lies the point — most people aren't being tested for COVID-19, especially those without symptoms, so it's anyone's guess how much of the population may have already had it. Symptoms 'Uncommon' During COVID-19 Outbreak at ShelterAnother example of COVID-19's apparent stealth came from a large homeless shelter in Boston. After a cluster of COVID-19 cases was observed there, researchers conducted symptoms assessments and testing among all guests residing at the shelter over a two-day period.7 Of 408 people tested, 147, or 36%, were positive, and although the positive individuals were more likely to be male, there were no other distinguishing characteristics. That being said, symptoms were conspicuously absent. Cough occurred in only 7.5% of cases, shortness of breath in 1.4% and fever in 0.7%. All were "uncommon among COVID-positive individuals," the researchers noted, adding that because COVID-19 can apparently be transmitted rapidly in a homeless shelter setting without a corresponding rise in symptoms, universal testing, rather than a symptom-triggered approach to testing, may be a better strategy for identifying cases. In Chelsea, Massachusetts, a city across the Mystic River from Boston, many cases are also occurring without symptoms. As of April 17, 2020, Chelsea had the highest rate of confirmed COVID-19 cases in Massachusetts — 32%, although the actual rate is probably higher.8 In a pilot study by physicians at Massachusetts General Hospital, 200 participants who "generally appeared healthy" were tested to see if they had antibodies made by their immune system to fight off COVID-19, which would suggest they'd been previously infected and may not have known it. Among them, 32% tested positive for antibodies linked to COVID-19. However, only about half said they'd experienced at least one COVID-19 symptom in the past four weeks. Chelsea's city manager, Thomas Ambrosino, told the Boston Globe, "[I]t's kind of sobering that 30 percent of a random group of 200 people that are showing no symptoms are, in fact, infected."9 While studies are hinting that the majority of COVID-19 patients in some populations could be without symptoms, the CDC has also confirmed that asymptomatic COVID-19 cases exist. "One of the [pieces of] information that we have pretty much confirmed now is that a significant number of individuals that are infected actually remain asymptomatic," CDC director Dr. Robert Redfield, told NPR. "That may be as many as 25%."10 Further, as reported in a correspondence article in The Lancet, in which researchers made a case for mass testing of both symptomatic and asymptomatic health care workers:11
Is Half the Population Potentially Already Part of the Herd?When the majority of people have had an infectious disease and naturally acquired long lasting natural immunity, herd immunity is said to have developed. Could it be that natural herd immunity is developing for COVID-19, with many not even realizing they've already had it? Yes, according to a hypothetical modeling study by researchers at Oxford University's Evolutionary Ecology of Infectious Disease lab, which suggests up to half of the U.K. population may have already been infected.12 They suggested that, according to public health theory, SARS-CoV-2, assuming it elicits protective immunity, will conform to the three distinct phases that typically occur when a novel infectious agent elicits protective immunity:13
The hypothetical modeling used data on COVID-19 deaths from the U.K. and Italy, and assumed that such deaths occur only in a vulnerable fraction of the population. As reported by New York magazine, under this scenario:14
That is, the U.K. initially planned to suppress the spread of COVID-19 but not completely eliminate it, allowing it to spread among younger, less vulnerable populations while protecting the elderly and immunocompromised.15 They since changed strategies, in part because of reports suggesting up to 250,000 people could die using the suppression plan, to one adopted by most other countries, involving case isolation, social distancing and widespread closures. "I am surprised that there has been such unqualified acceptance of the Imperial model," said lead researcher Sunetra Gupta, calling for immediate large-scale antibody testing to determine what stage of the pandemic we're currently facing.16 The researchers further noted:17
Vaccines for Everyone — Don't Become Naturally Immune!Biotech company Moderna began the first clinical trial for a COVID-19 vaccine in March 2020. Biotech company Inovio, which is funded by the Bill & Melinda Gates Foundation, is the second company to start testing an experimental COVID-19 vaccine in humans in the U.S.18 At least 70 COVID-19 vaccines are under development,19 each of them likely attempting to be fast-tracked to the market.20 Under normal circumstances, a vaccine may take five to 10 years to be developed, and pushing rapid progress comes with significant safety concerns. The Bill & Melinda Gates Foundation is funding the construction of factories to produce seven vaccine candidates,21 with the winning vaccine being produced en masse, to vaccinate the world's population. Foundation chief executive Mark Suzman said, "There are 7 billion people on the planet. We are going to need to vaccinate nearly every one. There is no manufacturing capacity to do that."22 The Bill & Melinda Gates Foundation is the biggest funder of the World Health Organization (WHO), by the way, and in a Washington Times opinion piece, published March 31, 2020, Gates calls for the complete shutdown of all U.S. states and quarantining of all Americans "until the case numbers start to go down … which could take 10 weeks or more."23 While Gates can undoubtedly afford it, few working-class Americans would be able to survive without income for months on end and could face serious mental health repercussions as a result. So Gates, a key funder of WHO, is calling for a 10-week or longer shutdown of the U.S. and the rapid building of brand-new vaccine manufacturing facilities to handle the manufacturing of billions of doses of COVID-19 vaccine — which would be rendered useless if it turns out that the majority of the population has already been exposed to the virus by going about their daily lives, and thereby acquired herd immunity naturally. from http://articles.mercola.com/sites/articles/archive/2020/04/28/asymptomatic-covid-19-cases.aspx NewsGuard has classified mercola.com as fake news because we have reported the SARS-CoV-2 virus as potentially having been leaked from the biosafety level 4 laboratory in Wuhan City, China, the epicenter of the COVID-19 outbreak. NewsGuard’s intern Nina Zweig (edited by deputy editor John Gregory) referred to my February 4, 2020, article, “Novel Coronavirus — The Latest Pandemic Scare,” in which I stated:
According to NewsGuard,5 “There is no evidence that the Wuhan Institute of Virology was the source of the outbreak, and genomic evidence has found that the virus is ‘96% identical at the whole-genome level to a bat coronavirus.’” Evidence Suggests SARS-CoV-2 Is a Modified Bat CoronavirusSure, as detailed in my April 26, 2020, interview with bioweapons expert Francis Boyle, who drafted the Biological Weapons Anti-Terrorism Act of 1989, SARS-CoV-2 started out with a bat coronavirus, but scientific evidence has revealed much more about this virus, none of which NewsGuard is bothering to take into account before classifying and censoring reports as “misinformation.” Importantly, there’s compelling scientific evidence published in many prominent scientific journals showing this virus was indeed created in a lab and not zoonotically transmitted (transmitted naturally from animal to human). As explained by Boyle, SARS-CoV-2 appears to be a bat coronavirus6 that was modified to integrate spike proteins that allow the virus to enter human cells by attaching to ACE-2 receptors. It’s also been modified to integrate an envelope protein from HIV called GP141, which tends to impair the immune system. Additionally, Boyle strongly suspects nanotechnology was used in its creation as well, as its exceptional ability to stay airborne for long periods of time is a nanotech hallmark.7 NewsGuard’s arbitrary dismissal of my February 4 article as fake news is equally inappropriate even if the virus is “all natural” and zoonotically transmitted. As reported by The Daily Mail, April 11, 2020:8
Governments Are Not Dismissing Possibility of a LeakAn April 14, 2020, report9,10 by The Washington Post highlighted the fact that U.S. State Department cables from two years ago warned there were inadequate safety precautions and procedures in place at Wuhan’s BSL4 facility, and April 15, 2020, Fox News reported11 that “State Department leaked cables renew theories on origin of coronavirus.” Yet NewsGuard, the thought police advertising front group for industries like Big Pharma and tobacco, simply dismisses and wants to bury this information. Such censorship has no room in a democratic and free society. I would argue that shutting down conversations about the origin of SARS-CoV-2 is a direct threat to democracy and indeed to science itself. Will NewsGuard classify The Washington Post’s and Fox News’ articles as “misinformation” as well? Fox News quotes Gen. Mark Milley, chairman of the Joint Chiefs of Staff12
As you may have noticed, in my “flagged” February 4 article I didn’t even make an assertion, I merely asked the question: “Is it pure coincidence that Wuhan City is now the epicenter of this novel coronavirus infection?” February 16, 2020, Chinese scientists even raised the possibility that SARS-CoV-2 is the result of bioweapons research leaked from the Wuhan Institute of Virology. See the video below for this report. Since my February 4 article, I’ve become increasingly convinced — through reviewing the scientific literature that NewsGuard ignores or is unaware of — that SARS-CoV-2 may in fact be a synthetic virus, likely created and released (inadvertently or not) from one or more laboratories that worked on weaponizing SARS and bat coronaviruses. According to an April 5, 2020, article13 in Daily Mail, British government officials are also considering the possibility that SARS-CoV-2 leaked from the Wuhan facility, stating the possibility of this “is no longer being discounted.” Will NewsGuard classify Daily Mail as a misinformant? Will they accuse Gen. Milley of spreading fake news? How about Federal Communications Commission chairman Brendan Carr, who tweeted14 an April 16 Fox News report15 about SARS-CoV-2 being leaked from the Wuhan lab “as part of China’s efforts to compete with U.S.”? Ironically, Carr even commented, “I’m old enough to remember when posting this would get you deplatformed.” Apparently, the abusive power of censorship that Twitter and other tech platforms have has not escaped the FCC. Is NewsGuard Protecting Chinese Interests?Interestingly, an April 16, 2020, report16 by CNN reveals the censorship of articles mentioning the possibility that SARS-CoV-2 may have leaked from the Wuhan BSL4 facility appears to come from China, which means NewsGuard is functionally protecting Chinese interests and inhibiting scientific inquiry. CNN writes:17
US Funded Wuhan LaboratoryAs I mention in my interview with Boyle, while the biosafety level 4 (BSL4) lab in Wuhan may have leaked the virus, the U.S. may have played a role in its creation. For starters, the chairman of the Harvard department of chemistry, nanoscience expert, Charles Lieber, Ph.D., was arrested earlier this year by federal agencies, suspected of illegal dealings with China.19 Lieber has denied the allegations. Lieber allegedly oversaw the Nano Key Laboratory, a joint collaboration by the Wuhan University of Technology and Harvard, although Harvard officials claim they had no knowledge of the lab before 2015. In our interview, Boyle dismisses the idea that Harvard was unaware Lieber was working on nanotechnology for biological materials with the Chinese as “preposterous.” NPR, which summarized the allegations as being centered around a Chinese recruitment program, added even more serious allegations, saying Lieber:20
Lieber’s attorney declined to comment on the charges, NPR said. It’s also noteworthy that both the U.S. National Institutes of Health and the Canadian Institutes of Health Research have funded research at the Wuhan BSL4 facility, including research on bat coronaviruses.21,22 Arizona senator Martha McSally told Fox news,23 “The NIH must immediately stop deploying American tax dollars to China for this dangerous research.” Justin Goodman, vice president for advocacy and public policy for the White Coat Waste Project added:24
April 14, 2020, Florida Congressman Matt Gaetz tweeted,25 “At best, Americans are funding people who are lying to us. At worst, we’re funding people who we knew had problems handling pathogens, who then birthed a monster virus onto the world.” NewsGuard Also Promotes Censorship via Public LibrariesNewsGuard has set itself up as the self-appointed global arbiter of what information is “trustworthy” based on nine “credibility and transparency” factors, not only for information viewed on private electronic devices, but also for information accessible in schools and public libraries26 — more than 700 libraries across the globe so far.27 Librarians will even provide instructions to patrons on how to install the NewsGuard extension on their personal computers, tablets and cell phones. Once you’ve installed the NewsGuard browser plugin on your computer or cellphone, the NewsGuard icon rating will appear on all Google and Bing searches and on articles featured in your social media news feeds. The NewsGuard ratings are meant to influence the reader, instructing them to disregard content with cautionary colors and cautions. Fake news is certainly a problem. But determining who should have the final word on credibility and what is “truth” is not a simple one. Who is going to verify the credibility and transparency of the verifiers, i.e., NewsGuard? NewsGuard Protects Big IndustriesTo understand NewsGuard’s agenda, you need to know something about its creation and funding. Aside from internet giants Microsoft28 and Google, NewsGuard is backed by companies that are involved in advertising and marketing of pharmaceutical products, cigarettes and unhealthy junk food to kids. NewsGuard's $6 million startup was funded in part by the Publicis Groupe,29 the “third largest global communications group” according to the Publicis website.30 Publicis was founded in 1926 by Marcel Bleustein-Blanchet, a French entrepreneur, with the goal of improving the image of advertising and turning it into “a real profession.” In fact, Publicis Groupe’s name is derived in part from the French word for advertising.31 The Publicis Groupe has been manipulating what people think about commercial products for nearly a century. Over that century, this advertising and communications firm bought or partnered with targeted advertising avenues, beginning with newspapers, followed by radio, TV, cinema and the internet. With revenue avenues secured, Publicis’ clients and partners built a global presence that dominated the advertising world. Be it tobacco or sugar, Publicis Groupe found a way to promote and strengthen big industries. In 1983, Publicis introduced the concept of global communication driven by marketing. Within the Publicis Groupe are four networks serving its clients,32 including Publicis Health,33 which once boasted on the website that its clients are "some of the biggest and most exciting names in health and wellness,” but has now taken that claim down and moved it to job postings.34 Publicis Scoops Up Top Vaccine CompaniesThe list of clients that once appeared on the health site’s wallpaper has also been taken down, but were proudly listed in an October 2019 Business Wire news release on Publicis’ third quarter revenue report — which, by the way, was up an impressive 17.3%.35 The report shows that Merck, GlaxoSmithKline, Sanofi Pasteur and Regeneron, just to name a few, have come onboard — showing that Publicis is now working for Big Pharma’s top dogs: vaccine companies. By happenstance, Regeneron just announced that it’s working on a coronavirus vaccine and treatment.36 Regeneron is also partnering with Sanofi to find a COVID-19 treatment; Sanofi is independently working on its own COVID-19 vaccine.37 The Publicis Health board also consists of a power pack of high-profile individuals with Big Pharma position backgrounds or affiliations.38,39,40,41,42,43 Leo Burnett, the ad company famous for creating the Marlboro man ad campaigns that made Marlboro the best-selling cigarette in the world and led to the nicotine addiction of millions, many of whom died from smoking, is also part of Publicis.44,45 To put icing on the cake, Publicis has also added Google and Facebook Messenger to their repertoire.46 When you consider that Publicis now describes its business model approach as putting clients and their needs and objectives at the center of all they do so their clients can “win and grow,” it’s easy to see what’s driving NewsGuard. What You Can Do to STOP This AbuseOverall, NewsGuard is just another big business aimed at keeping the chemical, drug and food industries, as well as mainstream media, intact by discrediting and eliminating unwanted competitors and analysts who empower you with information that runs counter to any given industry’s agenda. You can learn more about NewsGuard in my previous articles, “Beware: New Plan to Censor Health Websites” and “Thought Police NewsGuard Is Owned by Big Pharma.” If you’re as disturbed by censorship as I am, be sure to contact your local library today to find out if they’re one of the more than 700 libraries using NewsGuard. If they are, then ask them if they’re aware of NewsGuard’s censorship of truthful news that is now encroaching on scientific freedom and threatening the very roots of our democracy. If your local library is using NewsGuard, it would be helpful to start a campaign to get it removed. Contact your neighbors and let them know what is happening so they can kick out this public health threat. from http://articles.mercola.com/sites/articles/archive/2020/04/28/newsguard-fake-news.aspx 1 What does a zinc ionophore do?
2 How did Bill Gates gain such tremendous political power?
3 Which of the following supplements is now recommended by researchers to reduce your risk of COVID-19 infection and death?
4 During World War II, in order to supply their own fruits and vegetables, many Americans:
5 Why does the COVID-19 virus appear so frightening?
6 Which of the following is a selective inhibitor of highly damaging peroxynitrites and hydroxyl radicals?
7 What type of virus causes COVID-19?
from http://articles.mercola.com/sites/articles/archive/2020/04/27/week-127-health-quiz.aspx The debate about whether the antimalarial drug hydroxychloroquine is an effective treatment for COVID-19 continues, as a Chinese trial1,2,3,4 comparing clinical outcomes of those treated with the drug and those receiving standard of care alone reports “disappointing” results. Hydroxychloroquine Trial Reports Disappointing ResultsSeventy-five COVID-19 patients at 16 Chinese treatment centers received 1,200 milligrams of hydroxychloroquine in addition to standard of care for the first three days of treatment, followed by a maintenance dose of 800 mg per day for two weeks in mild to moderate cases and three weeks for severe cases. Another 75 patients received standard of care only. The primary endpoint was a 28-day negative conversion rate of SARS-CoV-2 (viral load reduction). Secondary endpoints included improvement rate of clinical symptoms and the normalization of C-reactive protein and blood lymphocyte count within 28 days. According to the authors, the hydroxychloroquine group only had a 28-day negative conversion rate of 85.4% compared to the control group’s rate of 81.3%. No difference in the alleviation of symptoms was observed between the two groups. Adverse events were also higher in the hydroxychloroquine group (30%) compared to controls (8.8%). You can find a listing of the adverse events in Table 2 of the study.5 The most common adverse event, at 10%, was diarrhea. That said, the authors point out that:6
Limitations of This StudyA few things are worthy to note about this study. Aside from its small size, the patients received a far higher dose of hydroxychloroquine than typically used in the U.S. — 1,200 milligrams for the first three days, followed 800 mg per day for two to three weeks, compared to the U.S. Food and Drug Administration’s suggested dosage of 800 mg on Day 1, followed by 400 mg per day for four to seven days, depending on severity.7 Secondly, most patients had mild disease with little hypoxemia, and thirdly, treatment was administered quite late, on average 16 to 17 days after the onset of disease. Commenting on the findings, Josh Fargas, associate professor of pulmonary and critical care medicine at the University of Vermont writes:8
This Study Failed to Use ZincPerhaps most importantly, however, is the absence of zinc, which Fargas does not mention. We now know that chloroquine and hydroxychloroquine act as zinc ionophores,9,10 meaning they shuttle zinc into your cells, and zinc appears to be a “magic ingredient” required to prevent viral infection.11 If given early, zinc along with a zinc ionophore should, at least theoretically, help lower the viral load and prevent the immune system from becoming overloaded. Without zinc, hydroxychloroquine may be more or less useless. So, in my view, I doubt this study is worth placing too much stock in, seeing how it did not administer supplemental zinc. As noted in the preprint paper, “Does Zinc Supplementation Enhance the Clinical Efficacy of Chloroquine / Hydroxychloroquine to Win Todays Battle Against COVID-19?” published April 8, 2020:12
Chloroquine Trial Stopped Due to Side EffectsIn related news, a Brazilian chloroquine trial13,14 stopped the high-dose arm of the study early due to patients developing ventricular tachychardia, a dangerous heart rhythm problem. As reported by Live Science:15
As explained in my previous article, “Antimalarial Medications: A COVID-19 Treatment Option?” chloroquine and hydroxychloroquine have been shown to be effective in the lab against the SARS coronavirus that appeared in 2003.16,17,18 Laboratory testing also suggests chloroquine is effective in cell cultures against COVID-19 when combined with an antiviral drug, remdesivir.19 However, chloroquine (Aralen) appears to be a more hazardous choice than hydroxychloroquine (Plaquenil), which is a derivative of chloroquine.20 Both use the same pathway, but hydroxychloroquine is thought to be about 40% less toxic21 and, overall, has a safer side effect profile.22,23 Quercetin — A Safer Alternative to Hydroxychloroquine?Considering the risks of chloroquine and hydroxychloroquine, and the evidence suggesting the reason these drugs work for COVID-19 is because they act as zinc ionophores, it’s worth questioning whether other more natural zinc ionophores can be used. One prime example would be quercetin, which is a naturally occurring zinc ionophore.24 As reported by the Green Stars Project,25 “Researchers from Oak Ridge National Lab used the world’s most powerful supercomputer, SUMMIT, to look for small molecules that might inhibit the COVID-19 spike protein from interacting with human cells and, interestingly, quercetin is fifth on that list.”26 Quercetin is one of only three natural products found to inhibit the SARS-CoV-2 spike protein. The only natural product found to be slightly more effective is luteolin, a polyphenol found in radicchio, green peppers, serrano and green hot chili peppers, chicory, celery and many other foods.27 Quercetin is another flavonols compound found in a variety of foods, including apples, Brassica vegetables, capers, onions, tea and tomatoes, just to name a few. It’s also contained in medicinal products such as Ginko biloba, St. John’s Wort (Hypericum perforatum) and elderberry (Sambucus canadensis). Research has already demonstrated that quercetin is a powerful immune booster and broad-spectrum antiviral. As noted in a 2016 study28 in the journal Nutrients, quercetin’s mechanisms of action include the inhibition of lipopolysaccharide (LPS)-induced tumor necrosis factor α (TNF-α) production in macrophages. TNF-α is a cytokine involved in systemic inflammation, secreted by activated macrophages, a type of immune cell that digests foreign substances, microbes and other harmful or damaged components. Quercetin also inhibits the release of pro-inflammatory cytokines and histamine by modulating calcium influx into the cell.29 According to this paper, quercetin also stabilizes mast cells and has “a direct regulatory effect on basic functional properties of immune cells,” which allows it to inhibit “a huge panoply of molecular targets in the micromolar concentration range, either by down-regulating or suppressing many inflammatory pathways and functions.”30 Another 2016 study31 concluded it helps modulate the NLRP3 inflammasome, an immune system component involved in the uncontrolled release of pro-inflammatory cytokines that occurs during a cytokine storm. In vitro studies32,33,34 have shown quercetin exerts antiviral activity against SARS-CoV, and preliminary findings35 suggest quercetin can inhibit the SARS-CoV-2 main protease as well. You can get even more details about the anti-inflammatory and antiviral powers of quercetin in “Quercetin Lowers Your Risk for Viral Illnesses.” Quercetin Being Studied for Its Use Against COVID-19The good news is researchers are in fact planning to study the use of quercetin against COVID-19.36 As reported by Maclean’s,37 Canadian researchers Michel Chrétien and Majambu Mbikay began investigating quercetin in the aftermath of the SARS epidemic that broke out across 26 countries in 2003. They discovered a derivative of quercetin provided broad-spectrum protection against a wide range of viruses, including SARS.38,39 The Ebola outbreak in 2014 offered another chance to investigate quercetin’s antiviral powers and, here too, they found it effectively prevented infection in mice, “even when administered only minutes before infection.” So, when the COVID-19 outbreak was announced in Wuhan City, China, in late December 2019, Chrétien contacted colleagues in China with an offer to help. In February 2020, Chrétien and his team received an official invitation to begin clinical trials. According to Maclean’s:40
Dosage Recommendations for Quercetin and ZincWhile the COVID-19 pandemic is in full swing — and for any future influenza season — supplementing with quercetin and zinc may be a good idea for many, in order to boost your immune system’s innate ability to ward off infectious illness. As for dosage, here are some basic recommendations: • Quercetin -- According to research from Appalachian State University in North Carolina, taking 500 mg to 1,000 mg of quercetin per day for 12 weeks results in “large but highly variable increases in plasma quercetin … unrelated to demographic or lifestyle factors.”41 • Zinc (and copper) -- When it comes to zinc, remember that more is not necessarily better. In fact, it can backfire. When taking zinc, you also need to be mindful of maintaining a healthy zinc-to-copper ratio. As noted by Chris Masterjohn, who has a Ph.D. in nutritional sciences,42 in an article43 and series of Twitter posts:44
How Much Zinc Do You Need?Masterjohn goes into even greater detail in his zinc article, discussing maximum absorption rates and much more.45 In summary, he recommends taking 7 mg to 15 mg of zinc four times a day, ideally on an empty stomach, or with a phytate-free food. The recommended dietary allowance in the U.S is 11 mg for adult men and 8 mg for adult women, with slightly higher doses recommended for pregnant and breastfeeding women,46 so we’re not talking about taking significantly higher dosages. Additionally, you can take one zinc acetate lozenge per day, which will provide you with an additional 18 mg of zinc. If you’re exposed to the virus, take one additional lozenge after the exposure. Masterjohn stresses that you’ll want to keep your total zinc intake below 150 mg per day to avoid negative effects on your immune system. He also recommends getting at least 1 mg of copper from food and supplements for every 15 mg of zinc you take. Keep in mind that there are many food sources of zinc, so a supplement may not be necessary. I eat about three-fourths of a pound of ground bison or lamb a day, which has 20 mg of zinc. I personally don’t take any zinc supplement other than what I get from my food, which is likely in an optimal form to maximize absorption. from http://articles.mercola.com/sites/articles/archive/2020/04/27/is-quercetin-safer-alternative-to-hydroxychloroquine.aspx |
Nia Pure NatureThe Provider of premium Quality Health Products To Live Better Lives Archives
March 2022
Categories |

 RSS Feed
RSS Feed
