|
It is easy to ignore the problem of litter. We "throw out" our waste and once a week the trash collector comes and takes it all away. Since it is out of sight, we seldom question where it goes or realize the waste is not really gone at all. It’s simply been relocated to landfills and incinerators. The average American throws away more than 7 pounds of garbage a day and Americans dispose of an astounding 60 million water bottles daily, which is nearly 700 per minute. Of course, food giants and huge retailers need to stop putting the onus and blame for excessive trash on consumers when they are the ones creating it. They need to dramatically reduce their wasteful packaging of plastic bottles, plastic bags and Styrofoam food containers. Consumers can put pressure on these trash producers, be it Coca-Cola or their local grocery stores, restaurants and dry cleaners. A new RT documentary, “Life Without Litter,” chronicles the efforts of correspondent James Brown to reduce the individual waste he generates every day over a two-week period, with the goal of a zero-waste lifestyle. While Brown, who lives in Moscow, does not arrive at the desirable zero waste state, he is able to greatly reduce his litter production by educating himself, being more conscious about his consumption and thinking ahead before buying or using wasteful products. The Challenges of Recycling in RussiaLike other countries, Russia is awash in packaged food that creates waste, as well as ubiquitous advertising that exhorts people to crave and buy such foods. But unlike some other countries, Russia has few places to recycle the waste, says Brown. In fact, the co-op where he and his wife live has one refuse bin for both non-recyclable and recyclable waste. Ironically, the documentary shows a sign near a garbage collection area that does not segregate recyclable items that says "Love Your Clean City." Recycling in Russia is "still in its infancy," he says.1 At the start of Brown's two-week waste reduction challenge, the documentary follows him throughout his day as he collects the waste he generates. At work, we see him use plastic cups and plastic plates that he would normally throw out but now collects. After work, Brown goes shopping at the grocery store and shows viewers how much litter he has already accumulated, even though he has not cooked anything yet. As he looks over a pile of trash from a single day's activities, he muses over the short usefulness of these items, compared to their long life as garbage. Brown is keenly aware of the plastic pollution caused by grooming and household cleaning products. While he doesn't want to add to the mountains of plastic trash that individual use creates, neither does he want to give up cleanliness for himself and his home. Grooming Products Made Without WasteTo investigate how he can replace cleaning and grooming products that produce waste with low or zero waste products, Brown watches a video of tips by Lauren Singer that includes a demonstration of toothpaste made with coconut oil, baking soda and essential oils. A Women in the World article about Singer, who lives a zero-waste lifestyle, notes that:2
Brown also tries using homemade, no-waste shampoo made from apple vinegar, which he says seems to work satisfactorily, at least on the first day. He also tries washing his clothes in water made from boiled beans. He says he has found a place in Moscow that uses mustard powder to clean dishes. Mindful Shopping Is Just the BeginningAs Brown continues his zero waste experiment, he returns to the grocery store, this time carrying his own bags. He is pleased to discover that the food sellers will gladly deposit the items in his bags rather than in the store's pre-packaging. Nevertheless, Brown still encounters waste he cannot avoid. In fact, he says, the only products he wanted to buy that he could find unpackaged were leeks, parsley and a pineapple. After his mindful shopping, Brown is able to cook his first "waste-free meal" — broccoli cream soup. Brown is pleased that the waste he and his wife produce in one week has gone from five bags to two bags. However, when he invites his friend and eco-activist Sergey Dorkin over to his apartment to analyze the trash, he gets disappointing news. Some of what Brown thinks can be recycled, can't. If "organic waste," usually food, is present, the refuse centers says it is not clean enough for recycling, says Dorkin. Plastic bags that have paper stickers cannot be recycled because the paper "will clog the material when crushed." And finally, while plastic food dishes made of material marked with the resin identification code 2 or 4 are OK to recycle, when plastic is attached to metal foil or composite material, as is often the case with food containers, it cannot be recycled. Sadly, only about 70% of what Brown thinks is recyclable actually is. As it turns out, recycling is not as simple as just separating the plastics. Better Disposal Methods Are Needed“Life Without Litter” shows that it is very difficult to completely eliminate the waste we produce in the way Lauren Singer and others have miraculously done. More education is needed about what is recyclable and more accessible recycling collection centers are necessary, especially for items like plastic bags. However, we can start the process by realizing that when we throw garbage "out," it is not really "out" at all. It’s simply relocated to landfills and incinerators. Landfills sound more environmental than "dumps," but they are hardly the answer to our waste problems and the tremendous amount of waste produced every day. In the 1970s there were 20,000 landfills in the U.S.; by 1986 there were 6,034 active sites.3 In 1997, the U.S. had 3,091 active landfills and over 10,000 old municipal landfills, according to the Environmental Protection Agency.4 In a continuing downward trend of active landfills, in 2009 there were 1,908 in the U.S.,5 as Waste 360 predicted would happen, due to regulations the EPA instituted in 1991. Newer rules implemented by the EPA in 2019 indicate there are now approximately 1,900 landfills6 in the U.S., due to closures of many landfills across the country. However, even though there are fewer active landfills, that doesn’t mean trash accumulation is also going down: For example, New York City now sends its trash to the states of Ohio and Pennsylvania,7 so whatever New York “saves” from its now-closed landfills is actually being shipped out of state. Since many municipal landfills accept hazardous waste, they are dangerous. Their "leachate" or water, which contains pollutants like benzene, pesticides, heavy metals and endocrine-disrupting chemicals, contaminates ground and surface water when the plastic landfill liners and pipes break down. Fortunately, EPA rules implemented in 2017 address leachates with new restrictions and regulations covering how the leachates are handled, collected and removed.8 While these rules also address air emissions, the plain fact remains that landfills also produce hazardous air emissions. Incinerators are equally as dangerous, emitting toxic materials like dioxins, mercury and cadmium and air particulate pollution. Other Important Sources of WasteWhen discussing litter and waste, the world also needs to address "clothes pollution" — clothing produced so cheaply it ends up being viewed as disposable. Electronic products and appliances are also considered disposable these days, and thrown out rather than repaired. To demonstrate the contribution of excessive clothing to pollution, Hugh Fearnley- Whittingstall, an English chef, celebrity and environmental activist, dumped a pile of 10,000 clothing items in the middle of a shopping mall.9 The crowd that gathered was asked how long it would take for Britain to dispose of that amount of clothing. While people in the crowd guessed "one week" or "several days," the correct answer is 10 minutes! Fearnley-Whittingstall said:10
Finally, let's not forget the pollution generated during the holidays. Season’s greeting cards alone could stack a football field 10 stories high, and enough gift ribbon is thrown away to tie a bow around the Earth.11 Too bad ribbon and cards are not generally regifted. Gifts themselves also tend to have excessive packaging. How You Reduce Your Personal WasteThere are signs the world is waking up to the waste problem, however. In 2019, 187 countries added plastic to the Basel Convention treaty that governs the movement of hazardous waste from one country to another.12 As you can see in “Life Without Litter” it is possible to greatly reduce the volume of garbage we generate through education, conscientious purchasing and planning ahead. Here are a few more tips:
from http://articles.mercola.com/sites/articles/archive/2019/12/21/zero-waste-lifestyle.aspx
0 Comments
Chronic fatigue syndrome (CFS), which is thought to affect up to 2.5 million Americans,1 is a debilitating condition in which sufferers experience unrelenting fatigue no matter how much rest they get. Pain and chronic inflammation are other hallmarks. A number of other names are also used for this condition, including:
The most common designation is ME/CFS and, according to the CDC, about 90% of people with ME/CFS have not yet been diagnosed.4 In the past, ME/CFS was typically brushed off as being a psychological problem, but in more recent years, researchers have discovered physiological commonalities between groups of individuals that validate their symptoms. For example, ME/CFS patients tend to have similar changes in gut bacteria, and certain inflammatory biomarkers in your blood appear to correlate with ME/CFS symptoms.5 Most recently, researchers have found additional support for the hypothesis that ME/CFS is rooted in mitochondrial dysfunction, which makes logical sense considering your mitochondria are responsible for energy production. These tiny powerhouses are an interconnected network that rapidly and effectively distributes energy throughout your body's cells.6 Your mitochondria are also responsible for programmed cell death, and serve as important signaling molecules that help regulate the expression of your genes. When your mitochondria do not work properly, low energy is a natural side effect. Knowing this, the remedy becomes clearer as well. A ketogenic diet, high in healthy fats and low in net carbohydrates, with moderate protein, is a key dietary strategy that helps optimize mitochondrial function. What Is Chronic Fatigue Syndrome?Until recently, the diagnosis of ME/CFS has been one of exclusion. This meant all other illnesses mimicking the symptoms of ME/CFS had to first be ruled out before doctors could suggest you were suffering from ME/CFS. Symptoms of ME/CFS can vary widely from one individual to the next. The most common symptom is one of overwhelming exhaustion that worsens with physical or mental energy expenditure and does not get better with rest.7 It may take up to 48 hours after activity to experience the full extent of the exhaustion. Other symptoms of the condition may mimic other medical conditions, and include:8,9,10
ME/CFS Is a Side Effect of Cellular ExhaustionAs mentioned, researchers have now identified what appears to be a root problem: exhaustion at a cellular level. This study11 was published in PLOS One at the end of October 2017. Immune cells in the blood of patients diagnosed with ME/CFS "show clear signs of low energy production," Science Alert reports.12 This strongly suggests mitochondrial dysfunction, as the mitochondria are responsible for energy production. As noted in the featured article:13
In short, ME/CFS patients lack the ability to compensate for increased stress on a cellular level, and the debilitating fatigue they experience is due to the inability to produce the cellular energy needed to keep the body fully functional. Their mitochondria are simply unable to produce enough ATP to maintain an energy gradient across their cell membranes. As noted by the authors:
ME/CFS Also Linked to Lack of Microbial Diversity in GutAnother study published in the journal Microbiome evaluated the blood and stool of 48 people diagnosed with ME/CFS and compared the results to those from 39 healthy people.14,15 Here, differences were found in both stool and blood samples. Using DNA sequencing, a process of determining the precise order of nucleotides in a DNA molecule, they found a distinct lack in diversity in the gut microbiome in affected individuals. Although these changes could not be clearly identified as either the cause or consequence of ME/CFS, researchers were heartened by the presence of these markers in 83% of the sample, and the possibility of treatment options to reduce symptoms. Quoted in the Washington Journal, professor of molecular biology and genetics at Cornell University, Maureen Hanson said:16
Addressing Leaky Gut May Help ME/CSF PatientsThe researchers theorize the inflammatory markers in the blood could be the result of a "leaky gut from intestinal problems that allow bacteria to enter the blood."17 Indeed, other recent research18,19 has confirmed the presence of more than a dozen inflammatory cytokines in blood that closely correlate with reported symptom severity in patients suffering from ME/CFS. This confirms a suspicion of some researchers that symptoms of fluctuating flu-like symptoms and body aches associated with ME/CFS is linked to an inflammatory response.20 It's important to realize that there is a distinct link between leaky gut and the foods you eat. Probably the single most important factor here is the herbicide glyphosate, which is pervasive. Between 1974 and 2014, over 3.5 billion pounds of glyphosate were used in the U.S. alone.21 Worldwide in 2017, 4.4 billion pounds (2 billion kilograms) of glyphosate were being used annually.22 Glyphosate will decimate tight junctions and contribute to leaky gut. Fortunately, you can radically reduce your exposure by eating organic and avoiding processed foods, which are usually contaminated. You can also check your glyphosate level with a simple urine test, to see how badly you've been exposed. Grains and lectins, even organic non-GMO, are particularly troublesome. Research shows that gluten stimulates a protein molecule in your gut called zonulin, which triggers the opening of junctures between the cells in your gut lining. In essence, it makes your gut more permeable, allowing food particles to escape into your bloodstream, causing inflammation, immune reactions and raising your risk of various autoimmune disorders. Certain plant lectins may also contribute to leaky gut by binding to receptor sites on your intestinal mucosal cells, thereby interfering with the absorption of nutrients across your intestinal wall. As such, they act as "antinutrients" and can have a detrimental effect on your gut microbiome by shifting the balance of your bacterial flora. Among the worst culprits are wheat germ agglutinin (WGA), found in wheat and other seeds in the grass family. In fact, according to Dr. Steven Gundry, author of "The Plant Paradox: The Hidden Dangers in ‘Healthy’ Foods That Cause Disease and Weight Gain," gluten is a minor problem compared to WGA. Evidence suggests lectins are strongly associated with autoimmune disorders in general, so anyone struggling with a dysfunctional immune system may want to seriously consider experimenting with a low-lectin diet. As for ME/CFS, leaky gut is not an automatic precursor. However, healing and sealing your gut and reducing the inflammatory response in your body may result in a significant reduction in chronic fatigue symptoms by supporting your immune system. Ketogenic Diet May Speed Resolution of Chronic FatigueIn 2015, Dr. Courtney Craig, a chiropractor and nutritionist, wrote about her personal experience with the ketogenic diet. Diagnosed with CFS in her teen years, she's been able to control her condition using a number of integrative health strategies, including intermittent fasting and nutritional ketosis. Describing a particularly harrowing relapse, she goes on to discuss how switching to a ketogenic diet helped her rapidly recover. She writes, in part:23
Indeed, when your body is able to burn fat for fuel, your liver creates water-soluble fats (ketones) that:
The Importance of Cyclical KetosisNutritional ketosis is the metabolic state associated with an increased production of ketones in your liver; i.e., the biological reflection of being able to burn fat, and is defined as having blood ketones in the range of 0.5 to 3.0 millimoles per liter. As a general guideline, a dietary intake of 20 to 50 grams (or less) per day of net carbs (total carbohydrates minus fiber) while also keeping protein low-to-moderate is usually low enough to allow you to make the shift to nutritional ketosis. However, once you achieve metabolic flexibility and are able to generate ketones with nutritional ketosis, it's important to include higher carb intakes every now and then. For all its benefits, continuous ketosis actually has some downsides that are easily avoided by implementing a cyclical "feast and famine" regimen. I detail the reasons for this in my book, "Fat for Fuel." In summary, long-term uninterrupted ketosis can trigger a rise in blood sugar by driving your insulin level too low. This paradoxical situation can occur because the primary function of insulin is not actually to drive sugar into the cell but rather to suppress the production of glucose by your liver (hepatic gluconeogenesis). Cycling in and out of nutritional ketosis will effectively prevent this rise in blood sugar in the absence of high glucose. So, once you are able to burn fat as fuel, having a day or two each week where you eat more net carbs and protein is important, especially when you're doing strength training, to prevent sarcopenia. After a day of "feasting," you then cycle back into nutritional ketosis (the "fasting" stage) for the remainder of the week. By periodically pulsing higher carb intakes, consuming, say, 100 or 150 grams of carbs opposed to 20 to 50 grams per day, your ketone levels will dramatically increase and your blood sugar will drop. Chronic Fatigue Patients Need Mitochondrial SupportIn this 2016 interview, I discuss the importance of mitochondrial function and how it may impact your symptoms of chronic illnesses like ME/CFS. It stands to reason that a condition that triggers an inflammatory response and gut dysfunction, and that results in overwhelming fatigue, will respond favorably to treatment strategies that reduce inflammation, heal your gut microbiome and support mitochondrial function and energy synthesis. Diet-wise, a cyclical ketogenic diet would be a foundational strategy. The following dietary recommendations will also help heal and seal your gut, lower inflammation and support healthy energy production. You can also read more about supporting your gut health in "Nourishing Your Gut Bacteria is Critical for Health and Mental Well-Being."
Other Strategies to Help Reduce Chronic Fatigue SymptomsThere is no known cure for ME/CFS, but there are strategies that can help alleviate symptoms,25 over and beyond the dietary recommendations already mentioned. My full metabolic mitochondrial therapy program is described in my book, "Fat for Fuel." Cold thermogenesis, photobiology, detoxification, exercise and avoiding electromagnetic fields are all strategies that will help improve mitochondrial health and function. When it comes to exercise, work out according to your ability, with a focus on increasing the amount of exercise you can handle. Research shows that a combination of aerobic activity and strength training can improve pain and fatigue symptoms. Gentle exercise such as yoga can also be an excellent part of your program, and yoga benefits your mind as well as your body. You may also want to address your mental outlook. In addition to talk therapy, I would recommend trying The Emotional Freedom Techniques (EFT) to help normalize your bioenergetic circuitry. Emotionally traumatic events can leave "energy blockages" for many years, which then interfere with your overall health, including immune function. There are many different techniques that can be used, but EFT is my favorite, and it's easy to learn and apply. from http://articles.mercola.com/sites/articles/archive/2019/12/20/cyclical-ketogenic-eating-for-chronic-fatigue.aspx Making cinnamon tea is a rather simple process — All you need to do is take a cinnamon stick (or two) and then boil it in water for a few minutes, and you'll have a spicy beverage that may have antimicrobial, antioxidant and anti-inflammatory effects,1 to name just a few of its benefits. Learn how a cup of cinnamon tea may help boost your health by reading this article. What Is Cinnamon Tea?As mentioned, cinnamon tea is a drink made by infusing cinnamon in hot water. Cinnamon is a spice with a long history in Ayurvedic medicine, having been used for more than 6,000 years. It comes from a plant genus called Cinnamomum, in which 250 trees and shrubs fall under, most of them native to Australia and Asia.2 According to Medical News Today, though, it's also native to South America and the Caribbean.3 Cinnamon appears either as a powder or as curled and fragrant brownish sticks — in fact, they come from the bark of cinnamon trees. According to the Smithsonian.com, this spice is harvested by "scoring and peeling sections of bark from trees and then scraping off the outer portion, revealing the light reddish brown inner bark."4 Peels that come from shoots and the smaller twigs are then dried — these are the curled sticks that you're likely familiar with. Larger cinnamon pieces, however, are processed and ground into powdered spice.5 Spice Advice describes cinnamon as having a sweet and woody fragrance.6 The flavor depends on the type of cinnamon you're getting, because there are actually two types of cinnamon — cassia cinnamon and Ceylon cinnamon.7 According to an article in Bon Appetit, cassia cinnamon has a darker color and rougher texture, and is rolled in thick sheets that are much thicker than Ceylon cinnamon. There are three types classified according to their place of origin: Indonesia, China and Saigon.8 Indonesian cassia, the most common variety in the U.S., is said to have the mildest and sweetest flavor, while Chinese cassia has a strong and bitter flavor; its use is more medicinal than culinary. Saigon is spicy, with an intense flavor and fragrance. Ceylon cinnamon, on the other hand, is dubbed "true" cinnamon. Compared to cassia, its flavor and aroma are more delicate and milder, described as having floral notes. The cinnamon sheets are hand-processed and rolled in thin and flat layers, much finer in texture compared to the other type. Because of this, Ceylon cinnamon is much more expensive and harder to find in stores.9 Most of the world's supply of this spice comes from Sri Lanka and the south part of the India.10 5 Health Benefits of Cinnamon TeaAside from the three potent essential oils in this spice, namely cinnamic acid, cinnamaldehyde and cinnamate, cinnamon also contains these beneficial compounds:11
These essential oils, which may be found in cinnamon tea (albeit in trace amounts), are responsible for the many health benefits linked to this popular spice. Using this spice or sipping on cinnamon tea may have positive effects on the following conditions: • Type 2 diabetes -- A 2010 study claimed that cinnamon and its components "have been shown to have beneficial effects on essentially all of the factors associated with metabolic syndrome, including insulin sensitivity, glucose, lipids, antioxidants, inflammation, blood pressure, and body weight."12 • Parkinson's disease -- A 2014 animal study found that cinnamon may benefit patients with this illness, as oral intake led to "dopaminergic neuronal protection, normalized striatal neurotransmitters, and improved motor functions" among the test subjects.13 • Alzheimer's disease -- In one study, an extract taken from Ceylon cinnamon was found to help inhibit hallmarks of this illness. This means that cinnamon may have a potential role in the discovery of therapeutic remedies for Alzheimer's disease.14 • Multiple sclerosis -- A 2015 study conducted on mice found that treatment with cinnamon may help "modify the pathological features" among the test subjects that have the animal model of this disease. These features include "widespread inflammation, loss of regulatory T cells (Tregs), hyperactivity of autoimmune Th1 and Th17 cells, breakdown of blood-brain barrier (BBB) and blood-spinal cord barrier (BSB), and loss of neuroprotective molecules in the [central nervous system]."15 • Cancer -- A study in the journal Molecules found that trans-cinnamic aldehyde, which is a key compound responsible for the potency of this plant's essential oil, may help reduce the risk of colorectal cancer.16 How to Make Cinnamon TeaCinnamon tea is one of those drinks you can make and enjoy at any time of day. The best way to prepare this is to use whole cinnamon sticks. Here's a basic recipe from WikiHow you can try:17 Procedure 1. Place the water in a medium saucepan (a glass kettle also works), along with the cinnamon stick. Cover and place on the stove. For a stronger tea, break the cinnamon stick into a few smaller pieces. 2. Turn the stove to medium low and bring the water to a slow boil. This slow process allows the flavor of the cinnamon to better leach out of the stick. This should take around 15 to 25 minutes. It takes a bit of time to darken, though, so if you see the water turning only a pale yellow color even upon reaching full boil, don't worry. 3. Remove the pot or saucepan from the stove once it's come to a complete boil. Allow the tea to cool slightly, around 15 minutes. During this time, the rest of the cinnamon's flavor will be released from the stick. You'll see it turn a golden red color. 4. Strain the tea using a fine mesh strainer and serve. Drink it right away. If you want the tea to be hotter, put it back in the pot and reheat it over the stove. Cinnamon Tea Recipes: Other Variations to TryOne of the best things about cinnamon is that it goes well with a variety of other flavors. You can infuse the tea with other herbs and spices, or even add some citrus juice. Here are a few cinnamon tea recipe options you can try. Ginger and Cinnamon Tea Ingredients Procedure 1. Put the cinnamon, ginger and four cups cold water in a saucepan, over high heat and allow to boil. 2. Reduce heat to low once the water has boiled, and then let simmer, without cover, for five minutes, so flavors will develop. 3. Strain the mixture in a heatproof jug. Mix in the honey and stir. Set aside until slightly cooled and then drink. (Recipe from Taste.com.au18) Apple and Cinnamon Tea Ingredients Procedure 1. Put the apple peels in a small pot of boiling water. Add the cinnamon stick and honey. 2. Leave to simmer for about 10 minutes. 3. Strain out the peels and drink. This recipe makes two servings. (Recipe adapted from Tasty19) Cinnamon Honey Tea Ingredients • Hot water • 1 tablespoon raw honey • 1 teaspoon cinnamon powder or 1 cinnamon stick Procedure 1. If you're using cinnamon powder, mix the honey and cinnamon in the bottom of a cup until you form a paste. If using a cinnamon stick, add the honey to the bottom of the cup and then put the cinnamon stick on top of it. 2. Add the hot water. 3. Stir well until the mixture is well-blended. If using the powder, make sure it's dissolved. Enjoy! (Recipe adapted from Old Fashioned Families20) Cinnamon Tea Side EffectsOf the two types of cinnamon mentioned above, Ceylon cinnamon tends to be recommended, as it does not contain high levels of coumarin. This phytochemical can be potentially dangerous, as it has hepatotoxic and carcinogenic properties, meaning it can harm the liver and increase your risk of cancer.21 Cassia cinnamon has as much as 1% coumarin, but Ceylon cinnamon only has 0.004%.22 So if buying this spice to make cinnamon tea, make sure to choose Ceylon cinnamon, so you can avoid the side effects of this substance. Frequently Asked Questions About Cinnamon TeaQ: What is cinnamon tea good for? A: Cinnamon spice is known for its anti-inflammatory, antioxidant, antidiabetic, anticancer and antimicrobial properties.23 It may also help lower your risk of cardiovascular diseases. These benefits may be passed on to cinnamon tea. Q: Can I drink cinnamon tea while pregnant? A: In small amounts, cinnamon and cinnamon tea may be safe for pregnant women and breastfeeding mothers. However, do not consume this in large quantities, as the safety of this spice in high doses is not known.24 Always drink cinnamon tea, or any herbal tea, in moderation. Q: Can cinnamon tea help you lose weight? A: Mixing cinnamon and honey in a drink is gaining popularity as a weight loss solution, but don't be so quick to jump on this trend. As Medical News Today notes, "no studies prove conclusively that cinnamon and honey can help you lose weight."25 Instead, focus on modifying your diet and adjusting your lifestyle to include exercise to help you shed unwanted fat and moderate your weight. from http://articles.mercola.com/sites/articles/archive/2019/12/20/xdjm18-teas-18mcsa-cinnamon-tea.aspx During an acute stress response, your body undergoes chemical changes that enable you to run from predators or take down prey. It's known as the flight-or-fight response. Unfortunately, some of those same life-saving chemical reactions used to protect you from danger may also be triggered as a coping response to perceived societal dangers, like dealing with a problem with a coworker or addressing the fear of public speaking. In other words, there are times your body finds it difficult to turn off the stress response. This chronic stress is one of the biggest challenges faced by U.S. adults. Many report stress has a negative impact on their physical and mental health. In a 2015 survey by the American Psychological Association, results revealed a sizable number felt they were not doing enough to manage their stress levels. Just half said they engage in stress management activities a few times a month or less and 18% said they never did. Some reported overeating or choosing unhealthy foods in response to stress, while 46% said they lie awake at night because their stress levels were so high. Robert Sapolsky is a professor at Stanford University. Every year he spends a few weeks in the Kenyan wilderness studying baboons. He discovered those who had higher levels of stress experienced higher heart rates and blood pressure measurements. The arteries of the baboons under stress were filled with plaque, restricting blood flow to the heart. This was the first time stress was scientifically linked to deteriorating health in wild primates. As it turns out, stress has the same effect on other primates — for example, us! Fortunately, the damaging effects of stress may be alleviated in part by relaxation, meditation and Emotional Freedom Techniques (EFT). Another potential trigger for a chronic stress response is suboptimal levels of vitamin D, magnesium and omega-3 fatty acids — and there is something we can do about that, too. Vitamin D Improves Symptoms of Depression and AnxietyVitamin D, otherwise known as the sunshine vitamin, is really a hormone produced by your body after exposure to UVB rays from the sun. The vitamin plays a significant role in several health conditions in your body. Deficiency in childhood may increase your risk of high blood pressure, and deficiency in adulthood may increase your risk of cancer and all-cause mortality. Insufficiency and deficiency may lead to a number of other negative health effects, which I cover in my past article, “Top 5 signs of Vitamin D Deficiency.” Vitamin D also has an effect on other daily struggles, including mood and emotional health. Research published in the Journal of Diabetes Research1 evaluated the effect of vitamin D supplementation on women with Type 2 diabetes who were currently experiencing symptoms of depression. The data revealed a significant decrease in the symptoms of depression and anxiety and an improvement in mental health status with the administration of vitamin D supplementation. They found the women who had the best response to the supplementation were not taking other medications for mood disorders, such as antidepressants or anxiolytics. Another published study2 compared blood results of men and women who suffered from depression to those of a control group. The researchers found significantly lower levels of calcidiol, a vitamin D analog found in the liver, in those suffering from depression and anxiety than in the control group without mental health conditions. In an evaluation of the relationship between vitamin D and animal neuronal cells, one research team3 found vitamin D maintains the extracellular mood-regulating neurotransmitter serotonin in the brain, which may explain the role it plays in neuropsychiatric disorders. How Much Vitamin D Do You Need?A simple math error4 is one reason for the inaccuracies in levels of vitamin D believed to be necessary to maintain good health. The error resulted in underestimation by a factor of 10. If corrected, the official recommendation would become 6000 IUs a day for adults, not 600. Data published in the Archives of Internal Medicine show 75% of American adults and teens are deficient when a sufficiency level of 30 nanograms per milliliter (ng/mL) is used. The only way to accurately measure how much vitamin D you need is to have your levels tested, preferably twice a year. According to Vitamin D Council standards, you are aiming for a level between 60 and 80 ng/mL, with 40 ng/mL being the lowest cutoff for sufficiency.5 In fact, new research in 2018 showed that the optimal levels for cancer prevention are between 60 and 80.6 Magnesium Helps Regulate Neurological Function and MoodMagnesium is the fourth most abundant mineral in your body, playing an important role in the health of nearly every one of your cells. A magnesium deficiency can have a wide range of consequences including constipation, muscle spasms, migraines and high blood pressure. Sufficient amounts of magnesium can reduce your risk for heart disease, high blood pressure and migraines as well as help you sleep better and enjoy greater mental and physical relaxation. Researchers have found a deficiency in magnesium is associated with the experience of subjective anxiety, and that supplementation may help mediate those symptoms. In a systematic review of research,7 including some unpublished studies, scientists found existing evidence magnesium is beneficial on subjective anxiety in those who are vulnerable to the condition. As with vitamin D, many Americans are deficient in magnesium, and often unaware of it. Some statistics report the deficiency numbers may be as high as 75% of adult and teenage Americans. Unfortunately, your body uses more magnesium while you're under stress, so a deficiency can create a vicious cycle. You can counteract this by eating magnesium-rich foods such as Brazil nuts, cashews, dark leafy greens like spinach and swiss chard, avocados and seeds. During particularly stressful times of the year you may want to consider using a supplement, as many of the world's growing soils have become severely depleted. There is no simple routine blood test to determine your magnesium level so it may be best to get a magnesium red blood cell test to give you a reasonable estimate while tracking and evaluating your symptoms. Your body requires magnesium for hundreds of biochemical reactions each day. Magnesium also plays a role as a catalyst for serotonin. You’ll discover more about this important mineral and how to optimize your levels in my past article, “Top Reasons to Make Magnesium a Priority.” Neuroprotective Activity of Omega-3 May Help AnxietyYour body requires dietary fat to keep your skin, hair and neurological system healthy. Fat helps you absorb certain vitamins and insulates your body to keep you warm. Although it’s harmful to eat too much of one or not enough of other types, without healthy fat your body doesn’t work properly. Polyunsaturated fats (PUFAs) are essential, meaning you must eat them since your body doesn't make them. The two main types are omega-3 and omega-6 fatty acids. Although both are essential, it's also crucial to good health that you eat them in the right ratio. After fat tissue, the brain has the highest concentration of fat. Also called lipids, omega-6 and omega-3 PUFAs are well represented in the brain. In one literature review8 scientists focused on addressing the question of the impact PUFAs have on anxiety and depression, an area of nutritional neuroscience. The researchers found evidence to support that a low intake of omega-3 fatty acid is associated with depression and anxiety, including studies of subjects diagnosed with depression or anxiety who presented with low levels of omega-3 and high levels of omega-6. Using an omega-3 index, a measurement of omega-3 on your red blood cells, researchers have been able to identify a range that may reduce your risk of heart disease. The reduction in inflammatory response associated with higher levels of omega-3 may also reduce symptoms of asthma and reduce your risk of Parkinson's disease, multiple sclerosis and depression. Vitamin D, Vitamin K-2, Magnesium and Omega-3 Work TogetherYour body is a complex organism that relies on what you eat to function at its best. Without a well-balanced intake of vitamins, minerals, fats and other nutrients, your body doesn’t have the tools it needs to function, and disease may result. But, none of these essential nutrients works in a vacuum. In other words, many of them need others to perform their jobs. For optimal functioning you'll want to ensure you get vitamin D3, vitamin K2 MK-7, magnesium and omega-3 fatty acids to protect your brain health and prevent depression and anxiety. GrassrootsHealth is offering a dual test kit to measure your omega-3 and vitamin D3 levels. Participation in this project is giving researchers the opportunity to learn how these two nutrients function together. I offer this test kit as a convenience since I don't benefit or participate in the research. Proceeds go directly to GrassrootsHealth. However, I believe deficiencies in these nutrients have a significant effect on health, and I’ve encouraged our staff to use the project to determine their best supplementation levels. The authors of two studies identified interactions between vitamin D and magnesium. The results reveal that low magnesium levels negatively impact your ability to use vitamin D, even when you have adequate levels in your body. By simply consuming optimal amounts of magnesium, you could lower your risk of vitamin D deficiency, thus reducing your dependency on vitamin D supplements. Vitamin K is a fat-soluble vitamin with significant influence over your health. Vitamin K2 works in tandem with vitamin D and magnesium to impact bone and heart health. While it is not integral to boosting your mood, if you are taking a vitamin D3 supplement, it's necessary to include vitamin K2 to reduce the potential for atherosclerosis. Vitamin D helps improve bone development by increasing your absorption of calcium while vitamin K2 directs the calcium into your skeleton, preventing it from being deposited in the arteries. from http://articles.mercola.com/sites/articles/archive/2019/12/19/stress-busting-supplements.aspx In his popular and oft-cited book, "Why We Sleep: The New Science of Sleep and Dreams,” professor Matthew Walker, Ph.D., founder and director of the University of California Berkeley’s Center for Human Sleep Science, details many supposed benefits of longer sleep. I’ve frequently referenced Walkers book in a number of my previous articles about sleep, which is why I became more than a little curious when I came across the work of Alexey Guzey.1 He claims to have spent more than 130 hours over the course of two months investigating the claims presented in only one chapter of Walker’s book, “Why We Sleep,” coming to the conclusion that the chapter, and likely the book, is “riddled with scientific and factual errors.”
While I do not have the kind of time required to duplicate Guzey’s double-checking of Walker’s work, I decided to present some of Guzey’s findings here so that you can review them for yourself. Certainly, I believe optimizing your sleep is crucial for mental and physiological health. The evidence for this is overwhelming. The question is how much sleep one actually needs, and whether more sleep equates to better health and increased longevity. Guzey’s findings contradict some of these assumptions. Will Longer Sleep Increase Your Life Span?On page 4 in “Why We Sleep,” Walker states — without corroborating references — that “the shorter your sleep, the shorter your life span.” According to Guzey, this claim does not conform to findings in the medical literature, most of which show a U-shaped relationship between the length of sleep and longevity. In other words, life span decreases at both ends of the spectrum, and Guzey cites three studies3,4,5 demonstrating this nonlinear association. He points out that “The studies typically find that people who sleep 7 hours have the highest longevity.” Figure 1 below is from a 2016 meta-analysis6 of 35 studies, published in Scientific Reports, which illustrates the nonlinear impact of sleep duration on all-cause mortality risk. The solid black line in the middle is the estimated relative risk, while the two dashed black lines on either side represent the 95% confidence interval. Guzey added the red dashed lines to highlight the lowest risk zone. 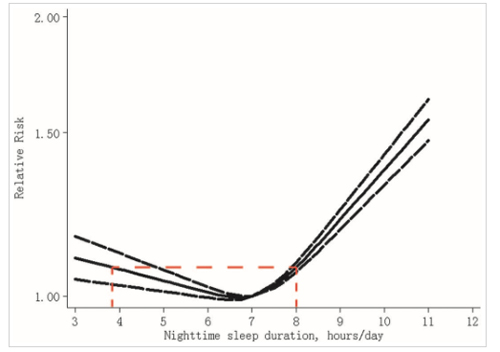
Based on this meta-analysis, the lowest all-cause mortality was just short of seven hours of sleep per night, with rates rising sharply after seven hours. The estimated relative risk (solid black line) actually appears to be near-identical at four hours and eight hours of sleep. Can Lack of Sleep Kill You?Interestingly, while it’s generally accepted that all animals sleep — which would support the idea that there’s a definitive biological need for it — this turns out to be false as well. Guzey points out that Walker contradicts himself on this issue in “Why We Sleep” — in one instance stating that “Every species studied to date sleeps,” while citing the “Encyclopedia of Sleep,” a 2,736-page book that states “many species reduce sleep for long periods of time … and that others do not sleep at all, in the way sleep is conventionally defined.”7 Guzey also has a problem with Walker’s claim that fatal familial insomnia (FFI) is evidence that lack of sleep can kill you. FFI is basically a genetically inherited prion disease, causing severe brain damage and organ failure. While chronic insomnia is a symptom, “It is reckless to claim that people with FFI die because of lack of sleep, given the amount of damage across the brain that accumulates in the course of the disease,” Guzey says.8 What’s more, the “Encyclopedia of Sleep” Walker cites actually states “There is little evidence that sleep induced by sedation can greatly extend life in FFI patients,” which would suggest the lack of sleep has little to nothing to do with the demise of these patients. Other research9 also notes that, ultimately, neurodegeneration appears to be the cause of death among FFI patients. So, on the whole, it’s probably not a good idea to draw any particular conclusions about the importance of sleep based on this disease. Will Short Sleep Double Your Risk of Cancer?In his book, Walker also claims that “Routinely sleeping less than six or seven hours a night demolishes your immune system, more than doubling your risk of cancer.” Guzey points out that this claim is, again, unsupported. Walker actually doesn’t cite any research for this statement, and “There do not appear to exist any experimental studies or studies that would reasonably be able to establish causality, that would support this claim,” Guzey says.10 Meanwhile, epidemiological evidence — which cannot show or establish causality — seem to refute the idea that sleeping less than six hours a night might significantly increase your cancer risk. Guzey cites a 2018 systematic review11 of 65 studies published in BMC Cancer — which included a total of 1,550,524 participants and 86,201 instances of cancer — that suggest the cancer risk remains near-identical for those sleeping between 5.5 hours and eight hours per night. Beyond eight hours a night, the cancer risk slowly increases, but not by much. Ditto for less than 5.5 hours of sleep. On his website,12 Guzey presents the following graph from that BMC Cancer review13 (again with the red dotted lines added for clarity). 
However, Guzey’s analysis also leaves some things out, as the BMC Cancer study14 he quotes does, in fact, state that subgroup analysis revealed that “short sleep duration increased cancer risk in Asians” by 36%, while “long sleep duration increased the risk of colorectal cancer.” People Consistently Overestimate Their Sleep TimeThe problem with epidemiological studies is the lack of verifiable accuracy, since most use self-reported data, and people can easily misjudge how much sleep they actually get on a regular basis. Guzey cites a study15 published in the journal Epidemiology, which found that people consistently over-reported their subjective sleep time. According to the authors:16
For this reason, it’s unclear just how meaningful epidemiological findings really are. As noted by the authors of this Epidemiology study, “The true associations between sleep duration and health may differ from previously reported associations between self-reported sleep and health.”17 So, while these kinds of studies can offer some general clues about correlation, one should remember that results are easily skewed, and when it comes to sleep, that people across the board tend to over-report the amount of sleep they believe they’re getting. Guzey applies this finding to Figure 1 (above) from the 2016 meta-analysis18 that found those with the lowest mortality slept right around seven hours, pointing out that if you take this over-reporting tendency into account, the lowest mortality would actually end up being around six hours.19 Is Sleep Deprivation at Epidemic Proportions?Next, Guzey tackles Walker’s claim that “The World Health Organization (WHO) has now declared a sleep loss epidemic throughout industrialized nations,” on page 4 of “Why We Sleep.” As far as Guzey could determine, WHO has never made such a declaration, and the source for Walker’s claim is the National Geographic documentary “Sleepless in America,” which also does not mention WHO. What’s more, most of the sources making this claim actually use Walker as their source, Guzey points out. My own online search, while not comprehensive, revealed the following: • A 1997 article in JAMA titled “World Health Organization Targets Insomnia” discusses the Worldwide Project on Sleep and Health, “a 20-year global mission to improve the treatment of sleep disorders under the aegis of the World Health Organization (WHO) and World Federation of Sleep Research Societies (WFSRS).” • The SAGE-INDEPTH study20 is a multi-center health and well-being survey led by WHO, which includes questions about sleep.21 A 2012 report22 in the journal Sleep, titled “Sleep Problems: An Emerging Global Epidemic? Findings From the INDEPTH WHO-SAGE Study Among More Than 40,000 Older Adults From 8 Countries Across Africa and Asia,” points out that “A large number of older adults in low-income settings are currently experiencing sleep problems, which emphasizes the global dimension of this emerging public health issue.” While the inclusion of a question mark in that title prevents it from being a direct statement, this paper could potentially be a source for Walker’s statement that WHO “has now declared a sleep loss epidemic.” At bare minimum, WHO’s sleep data are the basis for the researcher’s suggestion that sleep problems could be a global epidemic. • A 2014 paper23 in PLOS ONE also covered the results of WHO’s sleep data, stating that “the prevalence of severe/extreme sleep problems to be as high as 43.9% among Bangladeshi women, with prevalence figures higher than 25% observed also in Vietnam and South Africa, suggesting that there may be an under-recognized emerging global epidemic of sleep problems.” So, that’s two papers suggesting WHO’s data point to a global epidemic of sleep problems. What’s still missing is a reference for the “throughout industrialized nations” part of Walker’s statement, as Africa and Asia are unlikely to represent industrialized nations. As for WHO recommendations on sleep duration, I’ve not found any, either. A WHO technical meeting on sleep and health document24 from January 2004 discusses the health ramifications of insufficient sleep, but does not include any specific recommendations on adult sleep duration. WHO does, however, have guidelines for sleep duration for children under the age of 5. In its 2019 report,25 “Guidelines on Physical Activity, Sedentary Behavior and Sleep for Children Under 5 Years of Age,” WHO recommends infants aged 4 to 11 months get 12 to 16 hours of good quality sleep including naps; infants aged 1 to 2 should get 11 to 14 hours; and children aged 3 to 4 need 10 to 13 hours. Insufficient Sleep Is Likely RampantAll of that said, other researchers have stressed there’s a global sleep loss epidemic afoot, and that public health could indeed be improved were people to sleep a bit more. For example, a March 2019 review published in the journal Healthcare, states:26
Do a Majority of Adults Not Get Recommended Amount of Sleep?Walker’s claim that two-thirds of adults in developed nations fail to get the recommended amount of sleep appears to have a similar sourcing problem. Guzey writes:27
What Harm Can Walker’s Book Do?Considering the importance of sleep for biological and psychological functioning, which I cover in “Sleep — Why You Need It and 50 Ways to Improve It,” one might argue that Walker’s book can do no harm by, perhaps, overstating the risks and encouraging eight hours of sleep. Guzey disagrees, saying, in part:30
Unsourced, Unsupported Data Entering Scientific LiteratureGuzey also points out the problem with Walker’s book becoming a source in itself, given it doesn’t appear to stand on solid scientific ground. “This is how academic urban legends are created,” he says, citing academic papers that use “Why We Sleep” as sources for statements such as “All known forms of animal life must sleep,” and “the World Health Organization has pointed to a ‘global epidemic of sleeplessness’ with roughly two-thirds of adults sleeping less than 8 h a night” — statements of “facts” that Guzey show are either false or unsupported. Perhaps even more problematic, Walker sources his own book in his own academic papers; one published in The Lancet in 2018 and one in Neuron in 2019. As noted by Guzey, “the quoted statistics from ‘Why We Sleep’ are unsourced and we have no way to see how or where Walker got these numbers. Via The Lancet and Neuron, they have now entered the scientific literature, while lacking a primary source.” To Sleep More or Not Sleep More, That Is the QuestionAt the end of the day, how much sleep you need is quite personal, and you are probably the best person to assess whether your sleep habits are harmful or helpful. How do you feel when you wake up? How are your energy levels while driving to and from work? When do you get sleepy? Sleepiness during the day is a telltale sign of insufficient sleep. Ditto if you’re really dragging your heels in the morning and need multiple cups of coffee to get yourself into a productive space. In the evening, do you heed your body’s call for sleep, or do you push through and stay awake another hour or more? The key, I think, is being truly honest with yourself. Do you look, feel and behave your best after five, six, seven or eight hours of sleep? How much sleep do you need to be truly productive the next day? Take into account your mood too. Short-temperedness and getting easily frustrated are other telltale signs you’ve not slept enough. That said, guidelines are typically helpful, provided they’re based on decent science. In 2015, the National Sleep Foundation updated their sleep guidelines based on a review of more than 300 studies published between 2004 and 2014 that looked at the sleep duration required to maintain health. As noted earlier, the adult recommendations (ages 26 through 64) remained unchanged at between seven and nine hours, with an average of eight. The recommendation for seniors over 65 is seven to eight hours. Now, it would take an enormous amount of time to double-check those 300 studies to determine how many were based on self-reported sleep, and thus likely over-estimated the needed amount of sleep to maintain health and prevent disease. So, your best bet is to simply remember that sleep recommendations are not hard and fast. They’re guidelines, and if you’re sleeping like a prince or princess on seven hours and feel great, then forcing yourself to sleep more could be a mistake. If you’re not feeling good emotionally or physically, however, or if you’re struggling with an acute or chronic health problem, increasing your sleep time may be part of your answer. Experiment and see what makes you feel your best. Chances are, you’re not going to put yourself in jeopardy if you’re following your body’s cues. from http://articles.mercola.com/sites/articles/archive/2019/12/19/sleep-debunking-walker.aspx Your biological age can provide a good clue about your longevity, far more so than your chronological age. Your biological age refers to the state of your cells — they can be younger or older than your calendar age, which means you’re aging slower or faster than expected. Environmental exposures have a lot to do with biological or cellular aging and, according to a December 2019 study1,2 published in The Journals of Gerontology, lead, mercury and perfluorooctanesulfonic acid (PFOS) are the three toxins shown to have the greatest impact on your life span. While glyphosate was not included in this study, my guess is it would probably be a top contender as well, considering it disrupts normal body functions, especially your gut, and appears to enhance the damaging effects of other toxins. According to Stephanie Seneff, Ph.D., a research scientist at the Massachusetts Institute of Technology, glyphosate worsens virtually all modern diseases which, of course, will shorten your life. That said, lead, mercury and PFOS have repeatedly been identified as significant contributors to chronic ill health and are certainly among the most pervasive and concerning toxins out there. The Dangers of Lead Are Well-RecognizedAs one might expect, the December 2019 study3 found that “biological age was elevated relative to actual age in people who had chronic disease,” while those participating in a wellness program showed signs of slowed aging. “This observation suggests that biological aging is modifiable,” the researchers note, and that lowering your biological aging rate is “a sign of healthy aging.” Strong predictors of biological age were measures of metabolic health, inflammation and toxic accumulation, with lead, mercury and PFOS being the most influential predictors. In “The Heroes Who Sunk Lead,” I review the history of lead and its impact on organ function, especially your brain. Importantly, there is no known safe exposure to lead, which often affects young children and lower socioeconomic groups the hardest. Epidemiological studies have revealed African-American children have a higher incidence of lead poisoning, potentially from a slightly different way of metabolizing the heavy metal. Lead and calcium are chemically very similar, making lead a competitor at the cellular level and disrupting many different bodily systems.4 In your neurological system, it may disrupt neurons that use calcium to transmit information.5 The presence of lead will cause some neurons to fire more and decrease the signals in others. This may alter neurological development in the brains of children who have absorbed lead from their environment. The Public Health Heroes Who Fought to Lower Lead ExposureOne of the leaders in the fight against lead was Dr. Herbert Needleman, a pediatrician who saw firsthand the damage lead does to children. After years of treating children and observing the long-term effects of exposure, he maintained that a slow buildup of lead in the system could trigger symptoms even in the absence of overt poisoning. As lead-based paint and gasoline were the biggest contributors to lead poisoning in children, Needleman and public health expert and colleague Dr. Philip Landrigan began lobbying to remove lead from these products. The industry fought back using paid experts to pick apart and publicly lambast the research. The industry also went after Needleman personally, trying to discredit him and destroy his career. Another prominent player was geochemist Clair Patterson, Ph.D., who fought the oil companies to have lead removed from gasoline. Even when it was added to gas in the 1920s it was known to cause neurological damage. Still, the process was pursued as it enabled the oil companies to net greater profits. In 1965, Patterson published the book, “Contaminated and Natural Lead Environments of Man,”6 in an attempt to bring the dangers of lead gasoline on health and environment to light. Again, the industry brought to bear its influence to discredit the science and the man in an effort to maintain profits at the cost of human health. But despite the overwhelming odds, Patterson ultimately succeeded and was instrumental in bringing forth the 1975 U.S. mandated option of unleaded gas at the pumps. In 1986, Patterson’s persistence triggered the removal of lead from all gasoline in the U.S. altogether. As a result, Americans’ blood lead levels dropped nearly 80% by the late 1990s. In my view, Patterson is one of the greatest unrecognized public health heroes of the 20th century. Lead Exposure Continues To Be a ConcernThe elimination of leaded gasoline didn’t get rid of all lead exposures, however. As noted in a June 26, 2019, article7 in The Guardian, “hundreds of thousands of children in the U.S. remain at risk of exposure to lead, which causes cognitive and behavioral deficits.” Of the 31 states that have reported statistics on the percentage of children with elevated lead levels, Louisiana and Kentucky are among the worst.8 The U.S. Department of Housing and Urban Development estimates as many as 24 million U.S. residences built before 1978 still contain lead hazards, and in June 2019 announced $330 million in grants will be distributed to clean up lead and other safety hazards in low-income housing communities.9 A 2017 study10 also noted that many children with elevated lead levels remain undiagnosed. An estimated 1.2 million cases of elevated blood lead levels were thought to have occurred between 1999 and 2010, yet only 606,70911 were reported to the U.S. Centers for Disease Control and Prevention during that time, suggesting significant underreporting. According to the authors, “Based on the best available estimates, undertesting of blood lead levels by pediatric care providers appears to be endemic in many states.” Indeed, many pediatricians are likely to overlook factors such as lead exposure when faced with neurologically challenged children. This is a travesty, as your child’s condition will surely continue to decline unless the lead accumulation is addressed and reduced through a comprehensive detoxification program. Strategies to Avoid Lead PoisoningThe issue of preventing lead poisoning is a pressing matter, whether you have young children in your home or not. Harvard Medical School offers the following suggestions to protect yourself and your family against lead exposure:12
The Dangers of MercuryWhen it comes to mercury, two of the most prevalent sources are dental amalgam and seafood. Amalgam emits mercury vapor even after it is implanted into the body. This mercury is bioaccumulative and crosses the placenta to accumulate in fetuses, as well. Dental amalgam’s mercury is a known health risk, especially for children, fetuses, nursing infants and people with impaired kidney function. Mercury-based dental amalgam also pollutes water via dental clinic releases and human waste; air via cremation, dental clinic emissions, sludge incineration and respiration; and land via landfills, burials and fertilizer. Once in the environment, dental mercury converts to its even more toxic form: methylmercury and becomes a major source of mercury in the fish people eat. For several years now, I’ve been working with Charlie Brown and the Consumers for Dental Choice to eliminate the use of amalgam in the U.S. and around the world. Europe paved the way for global change by banning the use of amalgam fillings in pregnant or nursing women and children under the age of 15 as of July 1, 2018.15 In the U.S., the Food and Drug Administration has been dragging its feet, but there are finally signs of movement. November 13, 2019, a scientific advisory panel gathered to review the science on mercury. Consumers for Dental Choice brought several talented speakers to testify. The science committee, by consensus, called on FDA to end its silence on amalgam, and to start getting information about amalgam's risks to American patients, especially to vulnerable populations. The question now is whether the agency will continue protecting the amalgam business at the expense of public health — which it has done for decades — and ignore the conclusions of its own scientific body. To learn more about this and for instructions on how you can submit a public comment to the FDA, see “Dentists Are Breaking Toxic Mercury Laws.” Avoid Amalgam at All CostRegardless of what the FDA decides, it’s crucial to avoid amalgam if you want to protect your health and that of your children. Here are some general tips and guidelines: 1. Find another insurance company or plan that pays for mercury-free fillings in all teeth, without exceptions or LEAT clauses. 2. If your current dentist is still using mercury in his or her practice — even if they also offer mercury-free options — seek out a dentist that offers only mercury-free fillings for all patients. And, be sure to inform your dentist about the reason you’re transferring. The reason for this is because dentists who still use amalgam end up using it on people who rarely have any other choice, either because they cannot afford to pay the difference, or their state or government program dictates they can only receive mercury. This unfair practice needs to end, and the quicker we can get all dentists to go 100% mercury-free, the sooner these programs will be forced to change. So, selecting a 100% mercury-free dentist is an altruistic choice on your part, which will help those whose voices are so often ignored. 3. If you have mercury fillings, be sure to consult with a biological dentist who is trained in the safe removal of amalgam. For more information and guidance, see “How to Find a Biological Dentist That Can Treat You Holistically.” PFOS Contamination Is PervasivePer- and polyfluoroalykyl substances16,17 (PFAS) are widely used chemicals that make products water-, oil-, grease- and stain-resistant. The chemicals are also used in firefighting foam. One type, perfluorooctanoic acid (PFOA), is commonly found in older nonstick cookware. PFOA and its cousin PFOS are associated with a wide array of health problems, including cancer, immune and thyroid dysfunction, low birth weight and more.18 Making matters all the worse, these chemicals take thousands of years to degrade and are found in groundwater across the country.19,20 As such, they’re a considerable environmental threat. Research21 by the U.S. Centers for Disease Control and Prevention published in 2007 found PFAS chemicals in the blood of more than 98% of Americans tested. PFOS was phased out starting in 2000.22,23 However, thanks to their persistence in the environment, they’re still showing up in the strangest places — including food. How do they get into your food? One is by way of sewage sludge, applied to farmland. Documents24 obtained by The Intercept reveal 44 samples of sewage sludge tested by the Maine Department of Environmental Protection all contained at least one PFAS chemical. Another route is nonstick food wrappers. Research25,26 published in 2017 revealed 33% of fast food wrappers and containers contain fluorine, which suggests perfluorinated chemicals (PFCs) were used to give the paper that slick surface, and earlier studies27,28,29 have confirmed fluorinated chemicals can migrate from the packaging into the food. More recently, food testing by the FDA (performed in 2017 as part of its Total Diet Study30 and presented at the 2019 meeting of the Society of Environmental Toxicology and Chemistry) reveals PFAS chemicals are in the U.S. food supply,31,32,33,34,35 and at levels far exceeding the advisory limit for PFOA and PFAS in drinking water (there’s currently no limits in food). Of the 91 foods tested for 16 types of PFAS, 10 were found to contain the chemicals.36 As reported by PBS:37
How to Avoid Toxic PFCsTo minimize your family’s exposure to toxic PFCs, avoid products that are stain-resistant, waterproof or nonstick, or that have been treated with flame retardant chemicals. The Environmental Working Group’s “Guide to Avoiding PFCS”38 offers many helpful tips. Other suggestions that will help you avoid these dangerous chemicals include avoiding:
Live Longer by Lowering Your Biological AgeIf you’re interested in living healthy for longer, minimizing toxic exposures is a crucial component, and the three toxins reviewed here — lead, mercury and PFOS — appear to have the greatest impact on biological aging. That said, other basic lifestyle factors such as diet cannot be overlooked. As demonstrated in the featured study42 in The Journals of Gerontology, things like HbA1c also play an important role. High HbA1c is indicative of insulin resistance and Type 2 diabetes, both of which take a tremendous toll on your health and longevity. Insulin resistance is at the heart of most chronic disease, and once it transitions into full-blown diabetes, you open yourself up to a variety of complications, including an increased risk for heart disease and Alzheimer’s. So, in addition to avoiding toxic chemicals and heavy metals, you’ll also want to avoid foods high in sugar and synthetic chemicals. This means ditching processed foods and most restaurant food for home cooked whole food, ideally organic. You can also optimize your insulin sensitivity through resistance training (blood flow restriction training being particularly effective) and time-restricted eating. from http://articles.mercola.com/sites/articles/archive/2019/12/18/environmental-exposures-health-risks.aspx Color is used to market products and services, including those which affect our health. It appears that the first color used in art drawings was red, derived from ochre.1 The painting has been dated at 100,000 years old. Red often evokes feelings of strength, virility and fertility. Blue seems to be the world's favorite color according to various surveys. It may be a result of the calming effect the color has. Students who were given IQ tests with blue color covers had results of a few points higher than those given with red covers. Green is associated with the natural world but is also linked to envy, jealousy and illness. Purple was the first color in synthetic form when in 1856 a chemistry student did an experiment to cure malaria. The experiment failed but produced a permanent purple dye. Color plays a large part in graphic design as it can help set a mood or drive a point home. Women have been using hair color to change their look for centuries. By the same token, food manufacturers have been using food dye to improve the visual presentation of processed foods in hopes of making them more visually appealing. However, while color is a powerful means of presenting a product or changing emotions, when the dyes are not natural, the end result often does not have the positive experience you were seeking. Dyes May Have a Negative Effect on BehaviorIs it safe to assume eating petroleum products has no effect on health and behavior? The FDA believes this is the case. Despite their own statement acknowledging there may be a link between behavioral issues and specific artificial dyes,2 they continue to allow them in foods, medications and beverages. Interestingly, certain colors are only allowed in specific foods, such as orange B, which is approved only for hot dogs and sausage casings. This also begs the question, why does the opaque casing of sausage need color? Many children do not appear to be affected by the color dyes — but the operative word is "appear," since only those children whose parents have identified overt behavioral issues after consuming foods with color dyes have brought the issue to the forefront. The FDA exempts colors produced naturally from vegetables, minerals or animals from certification factors:
One parent identified several long- and short-term "effects" from the dyes in her son, Alex Bevans. Bevans' mother spoke to KQED3 and recounted a time when he was 7 years old when she found him "shredding his clothes and scratching himself on his bed. "He looked at me and said, 'Please get me a knife. I want to kill myself. I don't want to live like this anymore.'" She went on to explain the symptoms they have been able to correlate with the different colored dyes:
Bevans may have more symptoms than most, but Lisa Lefferts, scientist at the Center for Science in the Public Interest (CSPI), says he is not alone. Although the organization has been slow to act in the past, they are currently lobbying the FDA to follow regulations similar to those used in Europe.4
Food Dyes Not Adequately Tested for SafetyWarning labels are applied to all foods using artificial colors in Europe. Most European companies choose to use natural colored dyes so they don't have to use a warning label related to chemical dyes. A few American companies are using this strategy but have found that natural, healthier dye is more expensive and not as stable on the shelf. The FDA has approved nine colors made from petroleum, which are found in 90% of candies, fruit flavored snacks and drink mixes aimed at children. Joel Nigg, Ph.D., researcher from Oregon Health and Science University, finds past studies may show a cause and effect relationship between behavior changes and artificial dye if the data are taken at face value. The American Academy of Pediatrics reversed a previous position and issued a policy statement in 2018 in which they said,5 "Artificial food colors may be associated with exacerbation of attention deficit/hyperactivity disorder symptoms." Dr. Leonardo Trasande, involved in writing the AAP statement, said:6
Nigg believes more robust data are needed to make a delineation between behavior and artificial food dyes, but it is clear they are not benign. He went on to say,
Link Found Between Permanent Hair Dye and Breast CancerIt is reasonable to assume that if artificial colors have an adverse effect on children, they will also have adverse effects in adults. Scientists who published a recent study in the International Journal of Cancer7 acknowledged many hair products contain endocrine-disrupting chemicals and carcinogenic compounds that are potentially relevant to breast cancer. The researchers used a national prospective cohort to look at any associations among the use of hair dyes, chemical relaxers and straighteners in relation to breast cancer risk, by ethnicity. Participants were engaged from the Sister Study, including 46,709 women ages 35 to 74 who had a sister diagnosed with breast cancer but were cancer free themselves. When the participants were enrolled, 55% reported having used permanent hair dye, which was associated with a 45% higher risk of breast cancer in black women and a 7% higher risk in white women. In all participants, using hair straightener every five to eight weeks was associated with a 30% higher breast cancer risk.8 Nonprofessional application of semi-permanent dye or hair straightener on someone else also increased the risk of breast cancer. Dr. Otis Brawley, who served as executive vice president of the American Cancer Society from 2007 to 2018, was not surprised. When speaking to Newsweek, he said: "Many of us have worried that the chemicals in especially the permanent hair dyes and hair straighteners have the potential to cause cancer." Straighteners and Dyes Disproportionately Affect GroupsThe disparity in risk potential between black and white women increased further to 60% in those who used hair dye heavily, defined as application once every five to eight weeks. By contrast, the same risk for white women using the same application rate rose from 7% to 8%. When the researchers factored dye color, dark dye was linked with a 51% increase in black women and an 8% increased danger in white women. The same discrepancy existed in those who used light hair dye. Black women had a 46% increased risk for breast cancer, while white women had a 12% increased risk. The racial variations may have been linked to the way the dye is used or the differences in the products marketed to different audiences. Dr. Stephanie Bernik, chief of breast surgery at Mount Sinai Hospital, told Newsweek that black women begin with an increased risk of breast cancer, making it difficult to draw a clear association between hair product use and cancer risk. She went on to say:9
Lifestyle Choices Affect Risk for Breast CancerThere are several modifiable factors that may increase your risk of breast cancer, including being overweight or obese after menopause, taking hormones, drinking alcohol and being physically inactive.10 Factors you can't change are advancing age, personal and family history, genetic mutations and past radiation treatments. As you might expect, diet can also help prevent and play an important role in the treatment of breast cancer. The nutritional approach with the strongest scientific support is time-restricted eating, which increases metabolic autophagy, lowers insulin resistance, radically increases metabolic flexibility and improves your mitochondrial function. When exercise is added during the fasting window, these benefits increase. However, the vast majority have adapted to burning carbohydrates as a primary fuel as opposed to fat. One of the most effective strategies to become an effective fat burner is fasting 16 to 18 hours each day. Since cancer is a metabolic disease rooted in mitochondrial dysfunction, cancer cells require glucose for fuel and are unable to exist by burning fat. Cells must be healthy and normal to burn fat, so a high-fat, low-sugar diet will essentially starve cancer cells. See "What to Do if You Are Diagnosed With Breast Cancer," for further discussion on prevention and treatment options. from http://articles.mercola.com/sites/articles/archive/2019/12/18/artificial-color-health-effects.aspx You likely have heard that vaping is safe, or at least safer than smoking traditional combustible cigarettes. This myth may be easily perpetuated by the lack of offensive odor associated with traditional cigarettes. Currently, e-cigarettes are the most popular nicotine products used in high school and middle school. Statistics reveal that since 2011, teenagers have been smoking less but vaping more. In early 2019 reports of lung damage linked to vaping began reaching experts. By August there were 193 recognized cases. This rose to 2,291 who were hospitalized and 48 who died by early December.1 The latest numbers do not include those who became sick but were not hospitalized. This is only one of several dangers now associated with vaping as researchers are identifying more toxins inhaled with each puff. Researchers have discovered that flavors in vape juice damage the cardiovascular system and deliver heavy metals. Additionally, the cartridges are testing positive for evidence of fungi. Exposure to fungi is associated with asthma and a reduction in lung function. Other scientists have found that those who vape suffer from impaired activity of macrophages in the lungs, damaging vital immune cells. Regarding the most recent reports of lung damage, 80% said they vaped THC (the psychoactive ingredient in marijuana).2 Diversity among the products reported by patients makes it highly unlikely one brand was responsible for the outbreak. Instead, federal and state scientists have discovered Vitamin E oil is a likely suspect. Regarding e-cigarettes and vaping, the CDC said,3 "Vitamin E acetate has been identified as a chemical of concern among people with e-cigarette, or vaping, product use associated lung injury (EVALI)." Insurance Companies Unwilling to Take Vaping RiskInsurance companies use underwriters to evaluate the anticipated risk of insuring an individual or item. Underwriters help determine whether the company will profit from providing insurance. They determine the risk, which is used to determine a premium. Reinsurance is a form of insurance purchased by insurance companies to mitigate their own risk.4 With the rising numbers of deaths and injuries related to vaping, reinsurers are warning life insurance companies to place pressure on the underwriters to charge higher rates for specific groups who vape; these rates may be higher than those for smokers. Companies may even deny insurance altogether. Reinsurance companies use a body of research to inform their client model risk. They offer broad-based advice to insurance companies regarding certain topic areas rather than specific policies. However, if the insurance company does not take the advice of their reinsurance company, the reinsurer may refuse to provide reinsurance or raise their own premiums to the insurance company. In the recent past, most insurance companies have looked at those who smoke and those who vaped as one and the same. Smokers and those who vape often could pay double the amount of premiums for life insurance policies as those who do not partake in either habit. Currently, three major reinsurance companies are warning their clients about covering those who vape, while others are considering a new approach. Hannover Re has asked their clients to be cautious about insuring young adults under age 25 due to the large number of lung injuries. Some Insurance Companies Consider Pulling OutOther companies are questioning whether or not coverage should even be offered for this high risk group. The French reinsurer SCOR recommends their clients exclude people who vape products that U.S. authorities believe will trigger lung conditions. They name these products as those containing THC, while ignoring the more likely suspect of lung damage — vitamin E acetate. Reuters contacted 13 life insurance companies in Europe, South Africa and the U.S.; 12 said premiums for those who vape are the same as those who smoke. To highlight the cost difference, Justin Harper, head of protection marketing of a British insurer, shared estimated premiums. For a 35-year-old, a 20-year policy that would pay out $128,300 (£100,000) for life insurance coverage and the same for critical illness, the individual would pay $15.62 (£11.89) per month if they don't smoke or vape and $27.01 (£20.56) per month if they do. While lifestyle choices have always been associated with risk assessment for insurance companies, this current trend may start the industry down a slippery slope since it appears that choices may cause a company to begin to refuse coverage. As life insurance companies grapple with the risks of vaping, it may not be long before health insurance companies question the affordability of covering a rising number who spend weeks hospitalized in the ICU and months recovering. Juul Labs Purposefully Sold Contaminated ProductsAdding insult to injury, a recent lawsuit brought by Siddharth Breja, past senior vice president for global finance for Juul Labs, alleges that the company sold at least 1 million polluted mint flavored nicotine pods past the expiration date. The former employee claims Juul would not recall the defective products and he was told to charge the supplier $7 million to recover the cost of the contaminated batches. Breja alleges he was fired in retaliation for criticizing the sale. The lawsuit did not reveal the type of contamination within the nicotine pods but, according to The New York Times,
Juul denied firing Breja in retaliation for his comments and said they regarded the product safety charges as meritless. However, these allegations are increasing the spotlight on a company named in at least 50 lawsuits and under investigation by the FDA, Federal Trade Commission, five state attorneys general and several congressional committees. The popularity of vaping has been attributed to slick marketing campaigns that appear to be aimed at those under 18 years. Unfortunately, young people are continuing to show up in emergency rooms with symptoms of EVALI; some require mechanical ventilation for weeks. Addiction Raises Risks of Other Addictive BehaviorsAs the number of teens who become addicted to vaping increase precipitously, the risk of using highly addictive JuulSalts becomes more apparent. The company has positioned itself as a "genuine alternative to cigarettes" delivering a "nicotine hit that is much more like smoking a cigarette than other e-cigs." JuulSalts makes nicotine delivery less harsh to inhale and readily absorbed directly through the mucous membranes in your mouth. The nicotine is easier for the body to access and the cartridges contain up to twice the amount of nicotine as a pack of cigarettes. This combination increases the addictive nature of the product. Researchers have found high school seniors who had never smoked traditional cigarettes and who vape are four times more likely to pick up a cigarette in the following year. In animal studies, early addiction to nicotine has been associated with increased risks for future addictive behaviors. Researchers from the University of Pennsylvania found rats exposed to nicotine during adolescence grew up to drink more alcohol than those who were not exposed. It appeared to change the neurological circuitry in the brain within the reward center, which potentially explains how exposure at a younger age can increase the potential for addictive behavior later in life. Teen Vaping Rises Precipitously but No Treatment AvailableUnfortunately, teens have no place to turn for treatment options. Federal law prohibits the sale of devices to those under 18, yet many high school students report getting them from older students, purchasing them online or obtaining them from siblings. The rapid rise in addicted youth appears to have taken many by surprise; to date there has been little discussion about how to treat nicotine addiction in young children. The harshness of inhaling cigarette smoke has sometimes discouraged teenagers from the habit but this deterrent does not exist with vaping. The current medications on the market for nicotine withdrawal are not approved for use in children or young teens, which leaves them without a medical option to kick the habit. Until other options are available, it's important that parents and teens recognize quitting a nicotine habit requires patience, discipline and a willingness to follow a treatment plan. These strategies are not easily accepted by teenagers who are not fully cognitively developed, which may make addiction treatment more difficult for teens and their parents. Dr. Susanne Tanski, a tobacco prevention expert with the American Academy of Pediatrics, commented:5
Recognize the RiskThe industry claims vaping is a short-term solution to quitting traditional cigarettes but marketing campaigns have been squarely aimed at children and young adults, many of whom never smoked traditional cigarettes. Vaping delivers an appalling amount of heavy metals and toxic chemicals, including diacetyl, formaldehyde, diethylene glycol, tobacco-specific nitrosamines and highly reactive free radicals. In one study, scientists found e-cigarette flavors may induce early signs of cardiovascular disease leading to heart attack, stroke and death. Changes appear almost immediately at the cellular level and vapor from e-cigarettes boost production of inflammatory chemicals and impaired macrophages. This leads researchers to conclude it damages vital immune system cells. This type of damage increases the vulnerability of lung cells to dust, bacteria and allergens, which increases the risk of chronic obstructive pulmonary disease. Dr. Deepa Camenga, who is board certified in pediatrics and addiction medicine, recommends you talk to your children early on about e-cigarettes:
Suchitra Krishnan-Sarin, Ph.D., is co-leader of the Yale Tobacco Center for Regulatory Science. She recommends parents do not purchase e-cigs under the misconception they may prevent their children from smoking traditional cigarettes, and says:
from http://articles.mercola.com/sites/articles/archive/2019/12/18/vaping-life-insurance.aspx In the U.S., about 1 in 5 adolescents and 1 in 4 young adults has prediabetes, according to a study by U.S. CDC scientists. Prediabetes is a condition characterized by higher-than-normal blood sugar levels, which increases your risk of developing Type 2 diabetes, chronic kidney disease and cardiovascular disease.1 Its prevalence has increased in U.S. adolescents in the last decade, leading researchers to survey 5,786 youth to monitor the trend. Among adolescents aged 12 to 18, 18% had prediabetes, as did 24% of young adults, who were between the ages of 19 and 34.2 Prediabetes Affects an Alarming Number of YouthIn the U.S., the incidence of Type 2 diabetes is on the rise, projected to increase more than fourfold in the coming decades.3 Prediabetes is a warning sign of Type 2 diabetes, one that can be reversed before lasting damage is done if attention is made to healthy diet and exercise. A number of concerning findings were revealed in the study, which used data from the 2005 to 2016 National Health and Nutrition Examination Survey, including:4,5 • Adolescents and young adults with prediabetes were more likely to be male; in fact, males were nearly twice as likely to have prediabetes than females • Those with obesity were more likely to have prediabetes ((25.7% versus 16.4% in adolescents and 36.9% versus 16.6% in young adults)6 • Prediabetes was more common in Hispanic young adults than white young adults • Those with prediabetes had higher rates of other risk factors for Type 2 diabetes and heart disease, including high blood pressure, increased abdominal fat and lower insulin sensitivity
Prediabetes Is DiabetesA diagnosis of prediabetes may be a matter of semantics, as the majority of Americans are likely prediabetic and suffering from what the late Dr. Joseph Kraft, author of "Diabetes Epidemic and You: Should Everyone Be Tested?" called "diabetes in situ." Prediabetes is defined as an elevation in blood glucose over 100 milligrams per deciliter (mg/dl) but lower than 125 mg/dl, at which point it becomes full-blown Type 2 diabetes.8 According to the CDC, an estimated 84 million American adults — about 1 in 3 — are prediabetic, and most (90%) are unaware of this fact.9 That being said, any fasting blood sugar regularly over 90 suggests insulin resistance in my book. What's more, Kraft suggested 80% — 8 out of 10 — of Americans are insulin resistant. Based on data from 14,000 patients,10 Kraft, former chairman of the department of clinical pathology and nuclear medicine at Presence Saint Joseph Hospital, developed a powerful predictive test for diabetes.11 He would have the patient drink 75 grams of glucose and then measure their insulin response over time, at half-hour intervals for up to five hours. Interestingly, he noticed five distinctive patterns suggesting a vast majority of people were already diabetic, even though their fasting glucose was normal. Only 20% of patients had a pattern signaling healthy post-prandial insulin sensitivity and low diabetes risk, which means 80% were prediabetic or had "diabetes in situ." As explained by IDMProgram.com:12
What Are the Risks of Prediabetes?There are no obvious symptoms of prediabetes, an early state of insulin resistance known as impaired glucose tolerance; this is why so many people are affected but don't know it. There are, however, risk factors for the condition, which include:13
Having a large waist size (larger than 40 inches for men or 35 inches for women) or eating a diet high in processed grains and sugars is also associated with a higher risk of prediabetes.14 One of the greatest risks of prediabetes is that it increases your risk of developing Type 2 diabetes, which is a leading cause of death in the U.S. In fact, life expectancy recently declined in the U.S. for the first time in two decades,15 and Type 2 diabetes is a major factor in the decline.16 Researchers noted, "Diabetes may represent a more prominent factor in American mortality than is commonly appreciated, reinforcing the need for robust population-level interventions aimed at diabetes prevention and care."17 However, prediabetes can also be dangerous even if you haven't progressed to Type 2 diabetes. Prediabetes is associated with unrecognized heart attacks and kidney damage, for instance,18 and also means you're at least mildly insulin resistant. The higher your insulin resistance, the worse markers such as fasting insulin, triglyceride-HDL ratio and HbA1c will be, suggesting you're at increased risk for a number of chronic diseases, including not only diabetes but also heart disease, metabolic syndrome, cognitive decline and cancer. The good news is that insulin resistance, and thereby prediabetes, is one of the easiest health problems to correct. How to Determine if You're PrediabeticIf you're reading this and aren't sure what your fasting insulin and glucose levels are, these are blood tests I recommend receiving annually. Your fasting insulin level reflects how healthy your blood glucose levels are over time. A normal fasting blood insulin level is below 5, but ideally you'll want it below 3. A fasting glucose level below 100 mg/dl suggests you're not insulin resistant according to conventional recommendations, but I recommend aiming for a fasting (when you wake up) level below 90 mg/dL. A fasting level between 100 and 125 confirms you have prediabetes. Your blood sugar is measured through a glucose test, of which there are four types:
You could also do 24-hour continuous glucose monitoring, which I've done in the past, although it's pricey and probably not necessary for most people. At the time, I used a Dexcom monitor, which involves inserting a sensor beneath your skin for a week, which takes continuous glucose readings every few minutes. It really helped me fine-tune and evaluate how different foods impacted my glucose levels, and helped me understand the importance of feast-famine cycling. Timing Your Meals to Resolve PrediabetesIntermittent fasting, i.e., the cycling of feast (feeding) and famine (fasting) mimics the eating habits of our ancestors and restores your body to a more natural state that allows a whole host of metabolic benefits to occur.19 With regard to insulin resistance, research shows intermittent fasting promotes insulin sensitivity and improves blood sugar management by increasing insulin-mediated glucose uptake rates.20 While there are a number of different intermittent fasting protocols, my preference is fasting daily for 18 hours and eating all meals within a six-hour window. If you're new to the concept of intermittent fasting, consider starting by skipping breakfast and have your lunch and dinner within a six-hour timeframe, say 11 a.m. and 5 p.m., making sure you stop eating three hours before going to bed. It's a powerful tool that can work even in lieu of making other dietary changes. In one study, when 15 men at risk of Type 2 diabetes restricted their eating to a nine-hour window, they lowered their mean fasting glucose, regardless of when the "eating window" commenced.21 What you eat is also important. I recommend adopting a cyclical ketogenic diet, which involves radically limiting carbs (replacing them with healthy fats and moderate amounts of protein) until you're close to or at your ideal weight, ultimately allowing your body to burn fat — not carbohydrates — as its primary fuel. Reverse Prediabetes and Type 2 DiabetesWhile many people — young and old alike — are facing prediabetes and Type 2 diabetes, these conditions can be turned around. Along with intermittent fasting and a cyclical ketogenic diet, the tips that follow will help you reverse prediabetes and prevent Type 2 diabetes, while helping you avoid the chronic diseases related to them:
from http://articles.mercola.com/sites/articles/archive/2019/12/17/prediabetes-in-teens.aspx A class-action lawsuit has been filed against Seattle Children's Hospital after six children died and many others were sickened from Aspergillus mold.1 The lawsuit claims the hospital knew about "systemic problems" with its air-handling system and the related risks as far back as 2000, but "engaged in a cover-up" that left vulnerable patients exposed to potentially dangerous Aspergillus mold. Since 2001, Seattle Children's has identified 14 patients who contracted Aspergillus infections during or after hospital stays; six of those patients died as a result.2 Attorneys suggest, however, that many more children were likely affected and the numbers could be as high as "dozens if not hundreds."3 As of December 4, 2019, all 14 operating rooms at the hospital's main campus remained closed as a new air handling unit was moved into place. "We are incredibly sorry for the hurt experienced by these families and regret that recent developments have caused additional grief," Seattle Children's said in a statement. "Out of respect for privacy, we do not intend to share details about our patients or comment on specific cases or legal action."4 Hospital's Air Handling System Led to Deadly Mold InfectionsPatients affected by the toxic mold at Seattle Children's Hospital range in age from 2 months to 17 years.5 The infections occurred from 2001 to 2019 as a result of the hospital's negligence at maintaining and testing its facilities, leading to the transmission of Aspergillus mold spores to hospitalized children, according to the suit.6 In 2019, the hospital admitted that it was contaminated with Aspergillus mold since 2001, sickening patients as a result. Air tests conducted in November 2019 also revealed the presence of Aspergillus in several operating rooms.7 However, this wasn't a new revelation, as the suit alleges that the hospital knew by at least 2005 its air-handling system could be transmitting Aspergillus, when a family sued them over the issue. "During the course of that lawsuit troubling information surfaced regarding the Defendant's failure to maintain and staff its air-handling systems," the complaint reads. The lawsuit was settled in 2008 under confidential terms, but the hospital continued to keep "a deadly secret" in assuring patients and the public that it was safe, when in fact the mold persisted.8 Further, as early as 2002, an engineering consultant as well as the hospital's lead engineer warned the hospital about "filthy conditions" of its air-handling units, including water leaks, birds in fan shafts, units "rotting out" and failure to test equipment.9 The hospital also published an internal investigation in 2007 looking into three Aspergillus infections, but concluded they were isolated incidents. Seattle Children's CEO Dr. Jeff Sperring said in a statement:10
Dangers of Aspergillus InfectionAspergillus is a common type of mold found both indoors and outdoors, in decaying leaves and on plants, trees and compost.11 While most people come in contact with Aspergillus daily without any ill effects, certain strains can be dangerous for people with weakened immune systems or lung diseases. Disease caused by Aspergillus is known as aspergillosis, which can lead to allergic reactions and infections in the lungs or other organs.12 The CDC lists seven types of aspergillosis, which range in severity from mild to life threatening:13
Aspergillosis isn't a reportable disease in the U.S., which means numbers on its incidence are scarce, but the CDC estimates that nearly 15,000 aspergillosis-associated hospitalizations occurred in the U.S. in 2014, with costs of $1.2 billion.14 Further, they noted, "In a broad U.S. health care network of intensive care unit autopsy studies, aspergillosis was one of the top four most common diagnoses that likely lead to death."15 Aspergillosis Outbreaks in HospitalsWhile clusters of cases of dangerous invasive aspergillosis are rare in the general population, outbreaks have occurred previously in hospital settings, particularly among immunocompromised patients. Recently, lung infections caused by Aspergillus have been reported in people hospitalized with severe influenza and, in one study, invasive pulmonary aspergillosis occurred even in people without a compromised immune system.16 The CDC also reported:17
While it's virtually impossible to avoid exposure to aspergillus in the environment, hospitals have a responsibility to ensure they aren't exposing patients to this potentially dangerous fungus via an ill-maintained air handling system. As for Seattle Children's, they're installing new air handlers in an attempt to resolve the mold issues:18
Is There Mold in Your Home?Common health problems that can be attributed to poor and potentially toxic indoor air quality courtesy of mold growth include but are not limited to the following. If you have any of these issues, it may be worthwhile to consider your indoor air quality, and the possibility that your health problems may be related to mold.
To determine if mold is lurking in your home, first look for signs of visible mold or musty odors. However, not all mold is easily detectable, so if you can't see any visible traces of mold, take an air sample and use a moisture meter to determine the moisture level in the area. Wood flooring should have a maximum moisture content of 10% to 12%, for instance, as anything above that is a breeding ground for mold. Exterior walls should not have a moisture content above 15%. In addition to air sampling, proper lab testing of bulk samples of the mold growth is recommended. This will require cutting out a piece of the affected area. The U.S. EPA has a test called Environmental Relative Moldiness Index (ERMI), which tests for 31 different species of mold. If all you have is a small area of surface mold, you probably don't have to call in an expert. However, only attempt to clean it if it's limited to the surface of a small area. Any deep-rooted mold will require professional assistance to remediate. Mold Is Serious, Here's What You Can DoAspergillosis is an example of what Dr. Ritchie Shoemaker calls biotoxic illness. Most biotoxic illnesses are difficult to diagnose and treat as all of them, including mold, affect multiple systems in your body and produce a wide array of symptoms. Shoemaker, a pioneer in the field of biotoxin-related illness, explains that the underlying commonality, whether the disease is caused by dinoflagellates, mold or spirochetes, for example, is chronic inflammation. The inflammation induced by exposure to the toxins and metabolic products produced by these microorganisms is what wreaks havoc on your health. "In order to treat them, we need to both remove them from exposure and remove toxin from their body," Shoemaker said. Many of his patients have had success using cholestyramine (CSM), a rarely used cholesterol drug that binds to not just cholesterol, but just about everything of a particular molecular shape and size. "Binding CSM to the toxin prevents its reabsorption. There's another cholesterol-lowering resin called Welchol that also has these net positive charges … Even though people have used clays — and Bentonite is one — with some success, cholestyramine is so much better that people would put up with the common side effects of constipation and some reflux," he said. This is only the first step in his protocol, which includes 10 additional steps intended to stop the inflammatory process initiated by the mold (or other toxin) exposure. For more information, SurvivingMold.com is a great resource for medical practitioners and patients alike.19 I also discuss helpful tests and diagnostic tools for mold-related illness in "Mold: The Common Toxin That Can Be Far More Damaging Than Heavy Metals." Overall, your best approach is to find a well-informed physician with expertise in environmental medicine. Together you can devise an appropriate treatment plan. For a list of physicians with experience in treating mold-associated disease, see DrThrasher.org. from http://articles.mercola.com/sites/articles/archive/2019/12/17/seattle-childrens-hospital-mold.aspx |
Nia Pure NatureThe Provider of premium Quality Health Products To Live Better Lives Archives
March 2022
Categories |

 RSS Feed
RSS Feed
