|
The tendency is to lose muscle as you age, a condition known as sarcopenia. If you don’t do anything to stop it you can expect to lose about 15% of your muscle mass between your 30s and your 80s.1 An estimated 10% to 25% of seniors under the age of 70 have sarcopenia and as many as half those over the age of 80 are impaired with it.2 Enforced bedrest, due to hospitalization, for example, can also have a dramatic impact on your muscle mass, even if you’re younger. According to a 2015 review3 in Extreme Physiology & Medicine, you can lose 5.2% of your muscle mass in the first two weeks of bedrest. By Day 23, you can have lost up to 10% of your quadriceps muscle mass. Not only are strong muscles a requirement for mobility, balance and the ability to live independently, but having reserve muscle mass will also increase your chances of survival4 when sick or hospitalized. Since muscle is lost far more easily and quicker than it’s built, finding ways to continuously promote and maintain your muscle mass is of utmost importance. The Crucial Role of NAD+As reported by Science Daily,5 scientists recently discovered that Alzheimer's-like protein aggregates underlie the muscle deterioration commonly seen in aging, and that nicotinamide adenine dinucleotide (NAD+) is essential for combating this condition. Their study,6 published in the journal Cell Reports, showed that protein aggregates (amyloid) could be blocked by boosting the levels of NAD+, a biomolecule that is also essential for maintaining mitochondrial function. Higher levels of NAD+ were found to turn on the defense systems of the mitochondria and restore muscle function. Aggregated proteins have long been thought to be a contributor to brain aging, and this study proves aggregated proteins also contribute to muscle aging.
The study points out that NAD+ homeostasis is required to maintain proteostasis, i.e., the regulation of protein creation, folding, trafficking and degradation. It turns out that boosting NAD+ in later life will reduce amyloidosis (the buildup of amyloid) and mitochondrial dysfunction. The importance of NAD+ for healthy muscle function is also reviewed in “Sarcopenia and Muscle Aging: A Brief Overview,”7 published in the journal Endocrinology and Metabolism. The paper highlights:
As indicated by the Cell Report study, this Endocrinology and Metabolism paper highlights the connection between sarcopenia and mitochondrial dysfunction in both skeletal muscle and motor neurons. People with sarcopenia have been found to have both reduced mitochondrial oxidative capacity and inhibited NAD+ biosynthesis, and several studies have proposed that mitochondrial dysfunction in your neurons actually drive the development of sarcopenia.8 What Is NAD+?NAD+ is a substrate for a number of important enzymes, including poly(ADP-ribose) polymerase (PARP) and sirtuin 1 (SIRT1), which is known as a classic longevity protein. NAD+ is also essential in metabolic processes such as creating ATP in your mitochondria. It accepts and donates electrons and is used in oxidation-reduction reactions in the mitochondrial electron transport chain. Interestingly, what scientists have observed is that NAD+ levels decline in most tissues over time, and is associated with aging in general and is therefore thought to play an important role in many age-related diseases. According to the Endocrinology and Metabolism paper,9 researchers have shown that when the NAD+ salvage pathways in muscle are impaired, mitochondrial dysfunction and decreased muscle mass ensues. NAD+ boosting molecules such as nicotinamide riboside (NR), nicotinamide mononucleotide (NMN), nicotinamide (a form of vitamin B3 or niacin) and nicotinic acid (niacin) have all been shown to protect against age-related muscle disease. How to Boost NAD+Of those four, NMN is my personal favorite as it activates the NAD+ salvage pathway. As explained by Siim Land in a recent interview, featured in “Simple Strategies That Will Improve Your Immunity,” which also reviews the importance of NAD+ in COVID-19:
I’ve previously recommended the use of NR over NMN but have since changed my stance. NR used to be considered superior because no NMN transporter — required to get it into cells — had been detected. We now know there is such a transporter, which gives NMN the advantage as it’s also a more direct NAD+ precursor. 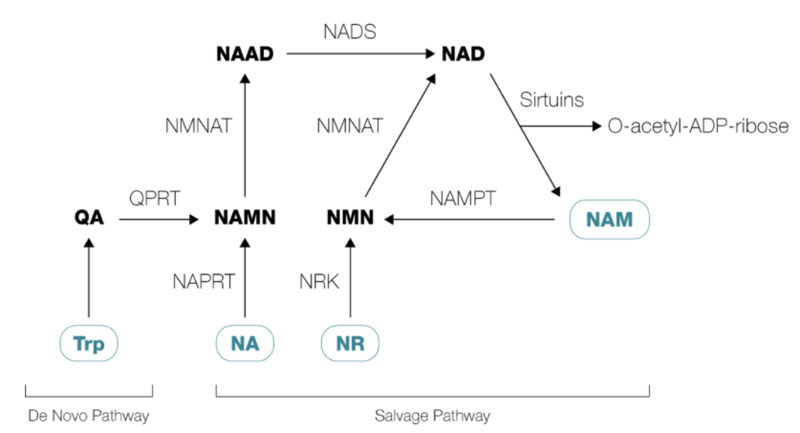
Most of the NAD+ precursor research is done with NR and that used to be my primary choice. However, as you can see from the image above, NMN converts to NAD+ whereas NR must first be converted into NMN before it can be converted into NAD+,10 so it makes more sense to use NMN for NAD+ augmentation. The image above also shows how niacin (NA) also finds its way to become NAD+. Niacin is also a useful supplement to use in increasing NAD+ levels. You just need to limit the dose to about 25 mg, which most is a dose low enough not to cause any flushing. Higher doses are not likely as effective as NMN and exercise in producing NAD+. The NMN transporter was discovered11,12 shortly before my interview with David Sinclair, Ph.D., a professor of genetics and co-director of the Paul F. Glenn Center for the Biology of Aging at Harvard Medical School. Interestingly, NMN is also Sinclair’s favorite NAD+ precursor. Sinclair is generally acknowledged for bringing the importance of NAD+ to the world with his experiments at MIT in the late ‘90s which connected NAD+ to sirtuin activation. We discuss these issues in “The Revolutionary Science of Aging and Longevity,” the interview from which is embedded above for your convenience. I believe one of the most effective ways of boosting your NAD+ level is to use NMN in suppository form, as this allows you to avoid most of the methylation of the supplement. Other alternatives include subcutaneous or intranasal administration, all of which are more effective than oral supplements. Unfortunately, NMN is not sold in suppository form, so you would need to get silicone candy molds and use coconut oil to serve as binder for the NMN. The suppositories would need to be refrigerated as coconut oil tends to melt at 75 degrees Fahrenheit. Additionally, NMN is quite perishable, which is another reason to refrigerate it. As for the other NAD+ boosters, I do not recommend using high-dose niacinamide because in high doses it inhibits Sirt1, an important longevity protein. As mentioned above, low-dose niacin (vitamin B3) of 25 mg can be used. Low doses of niacin, along with NMN in suppository form — both of which are precursors to NAD+ — are typically sufficient. As an added boon, raising your NAD+ also appears protective against severe COVID-19, as detailed in “Is Niacin a Missing Piece of the COVID Puzzle?” There are also NAD+ supplements available, but their price tags can be prohibitive. Lifestyle Strategies Can Address Underlying Cause of Low NAD+While supplements such as NMN can certainly be helpful, if your NAD is low, your best bet is really to address the underlying cause. The good news is that this can be done through simple lifestyle strategies such as exercise, sauna bathing, fasting, realigning your circadian rhythm and minimizing electromagnetic field (EMF) exposure. One of the reasons exercise, heat exposure and fasting work to address low NAD+ levels is because they are catabolic stressors that activate AMP protein kinase (AMPK). AMPK, in turn, activates an enzyme called NAMPT, which governs the NAD+ salvage pathway. Blood flow restriction (BFR) training can be particularly beneficial in terms of exercise. It has been shown to naturally increase your NAD level and is very safe for the elderly. You can learn more about this in “BFR Training for Muscle Mass Maintenance.” Your circadian rhythm, meanwhile, plays a role because it is controlled by longevity genes called sirtuins, SIRT1 in particular. If your circadian rhythm is misaligned, then sirtuins are not expressed, which in turn inhibits NAMPT, thereby shutting down your NAD+ salvage pathway. Oxidative stress and inflammation also use up and deplete NAD+, and exercise, sauna and fasting all help to reduce these. As a result, less NAD+ is depleted. So, these strategies not only improve your NAD+ production, but also reduce your body’s NAD+ consumption. The end result is a higher NAD+ baseline. EMF exposure, which is the topic of my book “EMF*D,” is one common source of oxidative stress, so it too increases your NAD+ consumption. It does this by activating PARP, a DNA repairing enzyme. Each time PARP is activated, it uses up 150 molecules of NAD+. Hence, reducing your EMF exposure can also be an important strategy to preserve and protect your NAD+ level. Your body also uses up NAD+ to detoxify alcohol, so if nightly drinking is part of your routine, consider giving it up. To learn more about how healthy lifestyle strategies such as the ones mentioned here can improve your NAD+ level, consider reading through the paper “Healthy Lifestyle Recommendations: Do the Beneficial Effects Originate from NAD+ Amount at the Cellular Level?”13 NAD+ Is a Crucial Antiaging ComponentSo, to summarize, raising your NAD+ level and keeping it high has many important health benefits, from supporting mitochondrial function, which is crucial for general health and longevity, to protecting against severe COVID-19 and age-related muscle loss. The great news is that this can easily be done by implementing the healthy lifestyle strategies reviewed above — exercise, sauna, fasting and recalibrating your circadian rhythm — while simultaneously avoiding things that deplete your body of NAD+, such as EMF exposure and excessive alcohol consumption. On top of that, supplements such as NMN together with normal doses of niacin can help boost your NAD+ in the short term. from http://articles.mercola.com/sites/articles/archive/2021/02/15/nicotinamide-adenine-dinucleotide-benefits-feb-2021.aspx
0 Comments
Hyperbaric oxygen treatment may be a practical method for slowing down the hands of time. At its foundation, aging represents a progressive loss of physiological capacity, researchers from Tel Aviv University and the Shamir Medical Center in Israel explained in the journal Aging.1 The biological deterioration leads to impaired functions and increased vulnerability to diseases, including cancer, heart disease, diabetes, Alzheimer’s disease and others. Hyperbaric oxygen treatment (HBOT), the Aging study suggests, may target two cellular hallmarks of aging — shortening of telomeres and cellular senescence, or the loss of a cell’s ability to divide and grow — thereby reversing signs of the aging process in humans.2 Sixty Hyperbaric Oxygen Sessions Slow Down AgingThe research team has been exploring the benefits of exposure to high-pressure oxygen at different concentrations inside a pressure chamber for years, with studies showing such treatments improved stroke, brain injury and brain function that was damaged by aging.3 The current study looked at hyperbaric oxygen treatment on healthy adults aged 64 and over to determine its effects on the normal aging process at a cellular level. Thirty-five subjects were exposed to a series of 60 hyperbaric oxygen sessions over a 90-day period. Blood samples, which were analyzed for immune cells, were collected before, during and after the treatments. Two exciting results were found:4
In a Tel Aviv University news release, study author Dr. Shai Efrati of the university’s Sackler School of Medicine, explained:
Telomeres and Cellular Senescence: Keys to Aging?Telomeres are repetitive nucleotide sequences at the end of each chromosome. Sometimes compared to the plastic tip on a shoelace, telomeres help protect DNA, preserving chromosome stability and preventing “molecular contact with neighboring chromosomes.”5 Evidence suggests telomere length may predict morbidity and mortality, with shorter telomeres linked to an increased risk of premature death,6 but the link is controversial. “This uncertainty is actually due to a kaleidoscope of biological and technical factors, including preanalytical issues (e.g., sample matrix), poor standardization of techniques used for their assessment, and dependence of telomere structure upon genetics, epigenetics, environment and behavioral attitudes, which may be present at a variable extent in various physiological or pathological conditions,” researchers wrote in the Annals of Translational Medicine.7 Still, despite the controversy, telomere shortening has been associated with a 23% higher risk of all-cause death, along with increased risk of certain cancers, including glioma, neuroblastoma, ovarian, endometrial, lung, kidney, bladder, skin and testicular.8 Telomere shortening is also said to represent a “major measurable molecular characteristic of aging of cells in vitro and in vivo,” which may have developed as a mechanism to protect against tumors in long-lived species.9 Dr. Amir Hadanny, chief medical research officer of the Sagol Center for Hyperbaric Medicine and Research at the Shamir Medical Center, an author of the featured study, added that lifestyle modifications and intense exercise have previously been found to slow telomere shortening, but HBOT appears to be another viable option:10
Cellular senescence is also known to play a role in cellular aging, and the accumulation of senescent cells is believed to be an integral part of the aging process, even potentially acting as a causal factor in age-related disease.11 Research is underway to develop therapeutic strategies to interfere with cellular senescence, including eliminating senescent cells,12 and HBOT has emerged as one potential strategy. Not Necessarily a Clear-Cut Fountain of YouthIt’s important to take the study’s limitations into account when evaluating whether HBOT is truly a fountain of youth, as the researchers imply. It was a small study, which means the results should be replicated in a larger sample of subjects. Also, as mentioned, the use of telomere length as a marker for aging is in itself controversial. The study also measured telomere length on immune cells called T cells, which may fluctuate depending on a number of environmental conditions, such as exercise. It’s a positive sign that HBOT also decreased cellular senescence in T cells, but as noted by Steve Hill, who serves on the board of directors for LEAF, a nonprofit promoting increased healthy human lifespan:13
This isn’t to say that HBOT isn’t useful, as other experts agree HBOT can have significant benefits for longevity. One of the reasons I'm fascinated by HBOT, in particular, is because of its ability to improve mitochondrial function.14 However, it should be viewed as one component of healthy aging, not necessarily a magic bullet that will stop it in its tracks. How Does Hyperbaric Oxygen Therapy Work?HBOT has long been used as a treatment for decompression sickness that can occur among scuba divers. When you sit in a hyperbaric oxygen therapy chamber, you breathe air that has two to three times greater air pressure than normal, which allows your lungs to absorb more oxygen. This, in turn, increases the amount of oxygen in your blood, which is transported throughout your body, fighting pathogenic bacteria and stimulating the release of healing growth factors and stem cells.15 In my interview in the video above with Dr. Jason Sonners, a chiropractor who has worked with HBOT for over 12 years, he explains that oxygen can be viewed as a nutrient. Your body needs it to carry out its regular functions and, when tissue is injured, it needs even more oxygen for healing.16 Most healthy individuals have somewhere between 96% and 98% oxygen in their hemoglobin, which means your capacity to increase your oxygen level is between 2% and 4%, were you to breathe medical-grade oxygen, for instance. However, you can increase your oxygen level far beyond that if your body is under pressure. According to Sonners:
HBOT Fights Mitochondrial and Oxidative Stresses, COVID-19HBOT can be used to help speed healing of any inflammatory condition, and it’s known to facilitate wound healing and cell survival. A small study involving 10 healthy men also revealed that a single 45-minute HBOT session reduced levels of metabolic stress-related biomarkers, including attenuating mitochondrial and oxidative stresses and relieving metabolic burdens, which suggests it may be useful for treating metabolic diseases.17 The fact that HBOT protects against mitochondrial dysfunction18 is a major benefit, considering most chronic and degenerative diseases involve mitochondrial dysfunction. Unfortunately, conventional medicine still reserves HBOT for a limited number of conditions, such as certain brain injuries and serious wounds, as well as the following:19
In the U.S., there are only 14 conditions for which insurance will pay for HBOT, whereas there are up to 100 approved indications for HBOT internationally, according to Sonners. From my perspective, it's medically reprehensible and inexcusable for a doctor to not treat patients with diabetic neuropathy, infections in the distal extremities or peripheral vascular disease with HBOT, as it will in most cases prevent the need for amputation. Other conditions that may benefit from HBOT include:
HBOT is also showing promise for treating COVID-19 via a number of beneficial effects, including reversing hypoxia, reducing inflammation in the lungs, increasing viricidal reactive oxygen species, upregulating HIF-increasing host defense peptides and reducing proinflammatory cytokines such as IL-6.20 Typically, hospitals will only provide HBOT if you have one of the 14 approved indications. If you’re interested in HBOT for other medical or longevity purposes, you’ll need to look into the private sector for treatment. The International Hyperbaric Association21 (IHA) and Hyperbaric Medical International22 (HMI) are two organizations that may direct you to more local centers. You can also learn more on HBOTusa.com, which is Sonner's primary education website where you can find a list of treated conditions, research, the benefits of HBOT in athletics, testimonials and much more. from http://articles.mercola.com/sites/articles/archive/2020/12/14/hyperbaric-oxygen-treatment-reverses-signs-of-aging.aspx Cardiovascular disease (CVD), or heart disease, is a term that refers to several types of heart conditions. Many of the problems associated with heart disease are related to atherosclerosis. This term refers to a condition in which there's a buildup of plaque along the walls of the artery, making it more difficult for blood to flow and for oxygen to reach the muscles, including the heart. This can be the underlying problem in cases of heart attack, stroke and heart failure. Other types of CVD happen when the valves in the heart are affected or there's an abnormal heart rhythm.1 Heart disease is the leading cause of death in the U.S. and it contributes to other leading causes including stroke, diabetes and kidney disease.2 It also ranks as the No. 1 cause of death around the world: Four out of five deaths are from heart attack or stroke.3 Heart disease accounts for 25% of deaths in the U.S. with a $219 billion price tag, based on data from 2014 to 2015.4 Scientists believe some of the key contributing factors are high blood pressure, smoking, diabetes, physical inactivity and excessive alcohol use. Cholesterol Levels in People Who Had Heart AttacksThere is ongoing disagreement over the levels at which cholesterol presents a risk for heart disease and stroke. Added to this, many doctors and scientists continue to recommend lowering fat consumption and using medications to lower cholesterol levels. A national study from the University of California Los Angeles showed that 72.1% of the people who had a heart attack did not have low-density (LDL) cholesterol levels, which would have indicated they were at risk for CVD. Their LDL cholesterol was within national guidelines and nearly half were within optimal levels.5 In fact, half the patients admitted with a heart attack who had CVD had LDL levels lower than 100 milligrams (mg), which is considered optimal; 17.6% had levels below 70 mg, which is the level recommended for people with moderate risk for heart disease.6 However, more than half the patients who were hospitalized with a heart attack had high-density lipoproteins (HDL) in the poor range, based on a comparison to national guidelines. The team used a national database with information on 136,905 people who received services from 541 hospitals across the U.S. They were admitted between 2000 and 2006 and, while they had their blood drawn upon arrival, only 59% had their lipid levels checked at that time. Of those who were checked, out of everyone who was admitted with a heart attack but didn’t have CVD or Type 2 diabetes, 72.1% had LDL levels less than 130 mg/dL, which was the recommended level at the time of the study (2009). In addition to this, researchers found the levels of HDL cholesterol (the “good” kind) had dropped compared to statistics from earlier years, with 54.6% having levels below 40 mg/dL.7 The desirable level for HDL is 60 mg/dL or higher.8 The findings led researchers to suggest that the guidelines for prescribing cholesterol medication should be adjusted — to lower the number at which drugs should be administered. In other words, they are suggesting that more people be put on cholesterol drugs. As explained by Dr. Gregg C. Fonarow, lead investigator:9
The study was sponsored by the Get with the Guidelines program that's supported by the American Heart Association, which promotes the use of statins for lowering LDL cholesterol.10 Fonarow has done research for GlaxoSmithKline and Pfizer, and has consulted for, and received honoraria from Merck, AstraZeneca, GlaxoSmithKline and Abbott — all of which manufacture cholesterol drugs, including statins. Cholesterol Myth May Be Kept Alive by Big PharmaWhile scientists and physicians continue to investigate the level of cholesterol that may affect heart attack risk, the theory that dietary cholesterol is a contributor has long been proven false. In the 1960s it may have been a conclusion that researchers made based on the available science, but decades later the evidence does not support the hypothesis.11 Yet, as some researchers have pointed out, the move toward removing dietary cholesterol limits has been slow. In the past 10 years, some have modified recommendations to address certain negative consequences of limiting dietary cholesterol, such as the risk of having inadequate levels of choline. Unfortunately, others have continued to promote low-fat diets and that could have hazardous results. Whether discussing cholesterol intake or serum cholesterol levels, the data do not support the hypothesis that it relates to heart disease. I believe it appears that the evidence supporting the use of cholesterol-lowering statin drugs is likely little more than the manufactured work of pharmaceutical companies. This also appears to be the conclusion of the authors of a scientific review published in the Expert Review of Clinical Pharmacology.12 The team identified significant flaws in three recent studies: “… large reviews recently published by statin advocates have attempted to validate the current dogma. This article delineates the serious errors in these three reviews as well as other obvious falsifications of the cholesterol hypothesis.” The authors present substantial evidence that total cholesterol and LDL cholesterol are not indicators of heart disease risk. In addition, statin treatment is doubtful as a form of primary prevention. In their analysis, they point out that if high cholesterol levels were a major cause of atherosclerosis, patients with high total cholesterol whose levels were lowered the most by statin drugs should see the greatest benefit. However, evidence does not show that to be the case. In another review of statin trials and other studies in which cholesterol was linked to heart disease, researchers could not find a correlation between cholesterol and the degree of coronary atherosclerosis, coronary calcification or peripheral atherosclerosis. They found no exposure response in which those with the highest level of cholesterol enjoyed the greatest benefit from reduction.13 These researchers propose the link between high LDL or total cholesterol and heart disease may be secondary to other factors that promote CVD, such as:14
Saturated Fat Is Crucial but Vegetable Oil Is DeadlyOne of the reasons so many people are sick is that we’re constantly told that animal fats are unhealthy and industrial vegetable oils are not, and people believe it. The authors of a recent paper in the Journal of the American College of Cardiology admits the long-standing nutritional guideline to limit saturated fat is incorrect. This is a tremendous step forward in righting a dietary wrong that started with Ancel Keys’ flawed hypothesis15 and has since had a significant impact on health and wellness. As the researchers note in the abstract:16
In a recent speech at the Sheraton Denver Downtown Hotel, titled "Diseases of Civilization: Are Seed Oil Excesses the Unifying Mechanism?" Dr. Chris Knobbe revealed evidence that seed oils, so prevalent in modern diets, are the reason for most of today's chronic diseases.17 His research charges the high consumption of omega-6 seed oil in everyday diets as the major unifying driver of the chronic degenerative diseases so prevalent in modern civilization. He calls the inundation of Western diets with harmful seeds oils "a global human experiment … without informed consent." You’ll find more, including a video of his presentation in “Are Seed Oils Behind the Majority of Diseases This Century?” Your Omega-3 Index Is More Predictive Than CholesterolThe combination of a diet high in omega-6 fats commonly found in vegetable oils and low in omega-3 fats, commonly found in fatty fish, is yet another risk factor for coronary heart disease. As the National Institutes of Health describes:18
Each of the three fats plays a unique role in cellular health. The authors of one study analyzed the risk of a cardiovascular event while taking icosapent ethyl.19 The medication is a "highly purified omega-3 fatty acid" that is "a synthetic derivative of the omega-3 fatty acid eicosapentaenoic acid (EPA)."20 Those who took the medication had a significantly lower number of ischemic events than those taking the placebo. An omega-3 deficiency leaves you vulnerable to chronic disease and lifelong challenges. The best way to determine if you're getting enough is to be tested, as it’s a good predictor of all-cause mortality.21 The omega-3 index is a measure of the amount of EPA and DHA in red blood cell membranes. This has been validated as a stable and long-term marker because it reflects your tissue levels. An index greater than 8% is associated with the lowest risk of death, while an index lower than 4% places you at the highest risk of heart disease-related mortality.22 Your best sources of fatty fish are wild-caught Alaskan salmon, herring, mackerel and anchovies. The larger predatory fish, such as tuna, have much higher amounts of mercury and other toxins. It's important to realize your body can’t convert enough plant-based omega-3 to meet your needs. That means that if you're a vegan, you must figure out a way to compensate for the lack of marine or grass fed animal products in your diet. If your test results are low, and you are considering a supplement, compare the advantages and disadvantages of fish oil and krill oil. Krill are wild-caught and sustainable, more potent than fish oil and less prone to oxidation. You’ll find more about the benefits of maintaining adequate levels of omega-3 fats in “Omega-3 Index More Predictive Than Cholesterol Levels.” Know Your Cholesterol RatiosThe cholesterol myth has been a boon to the pharmaceutical industry since cholesterol-lowering statins have become some of the more frequently prescribed and used drugs. In a report by the U.S. Preventive Services Task Force published in JAMA, evidence showed that 250 people need to take a statin drug for one to six years to prevent one death from any cause.23 When measuring cardiovascular death specifically, 500 would have to take a statin drug for two to six years to prevent even one death. As the evidence mounts that statin drugs are not the answer and simple cholesterol levels may not help you understand your risk of heart disease, it's time to use other risk assessments. In addition to an omega-3 index, you can get a more accurate idea of your risk of heart disease using an HDL/total cholesterol ratio, triglyceride/HDL ratio, fasting insulin level, fasting blood sugar level and iron level. You’ll find a discussion of the tests and measurements in “Cholesterol Does Not Cause Heart Disease.” from http://articles.mercola.com/sites/articles/archive/2020/08/26/cholesterol-levels-in-people-who-had-heart-attacks.aspx I've previously discussed the synergy between magnesium and vitamin D, and the importance of vitamin D for optimal immune function and overall health — especially as it pertains to lowering your risk of COVID-19. Previous studies have also highlighted the role this duo plays in cognitive function among older adults, as well as overall mortality. Vitamin D and Magnesium Protect Cognitive HealthOne such study,1 "Association of Vitamin D and Magnesium Status with Cognitive Function in Older Adults: Results from the National Health and Nutrition Examination Survey (NHANES) 2011 to 2014," points out that vitamin D not only protects neuronal structures and plays a role in neuronal calcium regulation, but also appears to impact your risk for neurodegeneration as you grow older. Magnesium, meanwhile, aside from being required for converting vitamin D to its active form,2,3,4 also plays a role in cognitive health, and magnesium deficiency has been implicated in several neurological disorders. Using NHANES data from 2,984 participants over the age of 60, the researchers compared serum vitamin D status and dietary magnesium intake against cognitive function scores. After adjusting for confounding factors, including total calorie consumption and magnesium intake, higher blood levels of vitamin D positively correlated with decreased odds of having a low cognitive function score on the Digit Symbol Substitution Test. The same trend was found when they looked at vitamin D intake, rather than blood level. The correlation of higher vitamin D levels and better cognitive function was particularly strong among those whose magnesium intake was equal to or greater than 375 mg per day. According to the authors:5
Magnesium Improves Brain PlasticityWhile magnesium intake by itself did not appear to have an impact on cognitive function in the study above, other research has highlighted its role in healthy cognition. Memory impairment occurs when the connections (synapses) between brain cells diminish. While many factors can come into play, magnesium is an important one. As noted by Dr. David Perlmutter, a neurologist and fellow of the American College of Nutrition:6
A specific form of magnesium called magnesium threonate was in 2010 found to enhance "learning abilities, working memory, and short- and long-term memory in rats."7 According to the authors, "Our findings suggest that an increase in brain magnesium enhances both short-term synaptic facilitation and long-term potentiation and improves learning and memory functions." COVID-19 Can Deprive Brain of OxygenWhile we're on the topic of the brain, a July 1, 2020, article8 in The Washington Post reviewed findings from autopsies of COVID-19 patients. Surprisingly, Chinese researchers have reported9 that COVID-19 patients can exhibit a range of neurological manifestations. A June 12, 2020, letter to the editor10 published in The New England Journal of Medicine also discusses the neuropathological features of COVID-19. As reported by The Washington Post:11
Interestingly, while doctors and researchers initially suspected that brain inflammation was causing the neurological problems seen in some patients, Solomon's autopsies found very little inflammation. Instead, these neurological manifestations appear to be the result of brain damage caused by oxygen deprivation. Signs of oxygen deprivation were present both in patients who had spent a significant amount of time in intensive care, and those who died suddenly after a short but severe bout of illness. I believe this is likely due to increases in clotting in the brain microvasculature. Solomon told The Washington Post he was "very surprised," by the finding. It makes sense, though, considering COVID-19 patients have been found to be starved for oxygen. As reported by The Washington Post:12
Magnesium and Vitamin D Impact MortalityGetting back to magnesium and vitamin D, previous research13 using NHANES data from 2001 through 2006 found the duo has a positive impact on overall mortality rates. This study also pointed out that magnesium "substantially reversed the resistance to vitamin D treatment in patients with magnesium-dependent vitamin-D-resistant rickets." The researchers hypothesized that magnesium supplementation increases your vitamin D level by activating more of it, and that your mortality risk might therefore be lowered by increasing magnesium intake. That is indeed what they found. According to the authors:
Magnesium Lowers Vitamin D Requirement by 146%According to a scientific review14,15 published in 2018, as many as 50% of Americans taking vitamin D supplements may not get significant benefit as the vitamin D simply gets stored in its inactive form, and the reason for this is because they have insufficient magnesium levels. Research published in 2013 also highlighted this issue, concluding that higher magnesium intake helps reduce your risk of vitamin D deficiency by activating more of it. As noted by the authors:16
More recently, GrassrootsHealth concluded17 you need 146% more vitamin D to achieve a blood level of 40 ng/ml (100 nmol/L) if you do not take supplemental magnesium, compared to taking your vitamin D with at least 400 mg of magnesium per day. 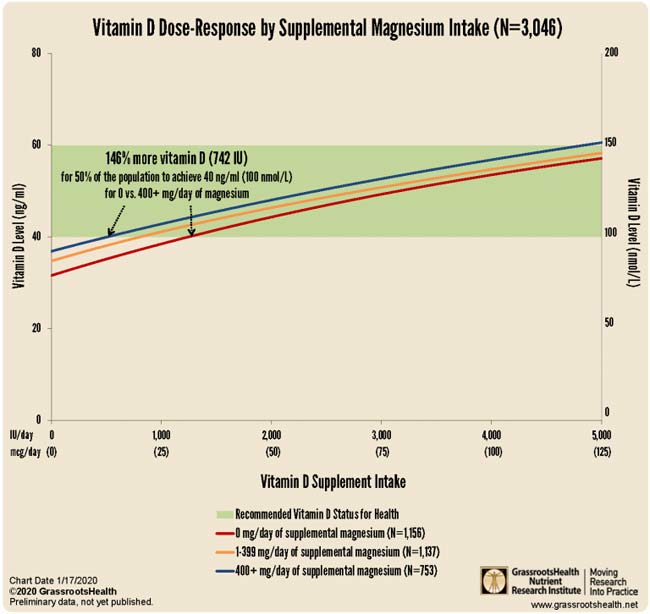
The interplay between magnesium and vitamin D isn't a one-way street, though. It goes both ways. Interestingly, while vitamin D improves magnesium absorption,18 taking large doses of vitamin D can also deplete magnesium.19 Again, the reason for that is because magnesium is required in the conversion of vitamin D into its active form. Magnesium + Vitamin K Lowers Vitamin D Requirement Even MoreMagnesium isn't the only nutrient that can have a significant impact on your vitamin D status. GrassrootsHealth data further reveal you can lower your oral vitamin D requirement by a whopping 244% simply by adding magnesium and vitamin K2. As reported by GrassrootsHealth:20
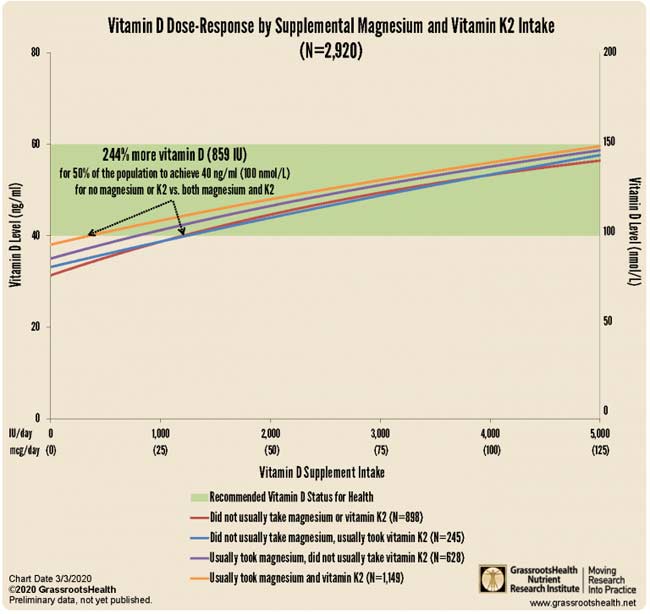
How to Boost Your Magnesium LevelThe recommended daily allowance for magnesium is around 310 mg to 420 mg per day depending on your age and sex,21 but many experts believe you may need anywhere from 600 mg to 900 mg per day.22 Personally, I believe many may benefit from amounts as high as 1 to 2 grams (1,000 to 2,000 mg) of elemental magnesium per day, as most of us have EMF exposures that simply cannot be mitigated, and the extra magnesium may help lower the damage from that exposure. My personal recommendation is that unless you have kidney disease and are on dialysis, continually increase your magnesium dose until you have loose stools and then cut it back. You want the highest dose you can tolerate and still have normal bowel movements. When it comes to oral supplementation, my personal preference is magnesium threonate, as it appears to be the most efficient at penetrating cell membranes, including your mitochondria and blood-brain barrier. But I am also fond of magnesium malate, magnesium citrate, and ionic magnesium from molecular hydrogen as each tablet has 80 mg of elemental magnesium. Eat More Magnesium-Rich FoodsLast but not least, while you may still need magnesium supplementation (due to denatured soils), it would certainly be wise to try to get as much magnesium from your diet as possible. Dark-green leafy vegetables lead the pack when it comes to magnesium content, and juicing your greens is an excellent way to boost your intake. Foods with high magnesium levels include:23
from http://articles.mercola.com/sites/articles/archive/2020/07/16/magnesium-cognitive-function.aspx The older you get, the more important your muscle mass becomes. Not only are strong muscles a requirement for mobility, balance and the ability to live independently, but having reserve muscle mass will also increase your chances of survival1 when sick or hospitalized. Muscle is lost far more easily and quicker than it’s built, so finding ways to continuously promote and maintain your muscle mass is really crucial, especially as you get older. Age-related loss of muscle mass is known as sarcopenia, and if you don’t do anything to stop it you can expect to lose about 15% of your muscle mass between your 30s and your 80s.2 An estimated 10% to 25% of seniors under the age of 70 have sarcopenia and as many as half those over the age of 80 are impaired with it.3 In the lecture above, Brendan Egan, Ph.D., associate professor of sport and exercise physiology at the School of Health and Human Performance and the National Institute for Cellular Biotechnology at Dublin City University in Ireland, reviews the latest research on exercise training for aging adults, which places a significant focus on building and maintaining muscle, and the nutritional components that can help optimize training results. Muscle Strength and Function in Relation to Muscle SizeWhile it’s true that larger muscle is indicative of stronger, more functional muscle, it’s not a true 1-to-1 relationship. As noted by Egan, “you can have situations where you can gain back function without necessarily gaining muscle size.” To illustrate this point, Egan presents data from the Baltimore Longitudinal Study of Aging, which looked at leg strength and lean muscle mass. While declines in muscle mass and strength are relatively well-synchronized in the 35- to 40-year-old group, strength dramatically drops off as you get into the 75-year-old and over groups, with 85-year-olds seeing dramatic declines in strength and function relative to the decline in muscles size. Speed as a Measure of Functional Muscle CapacityOne way to measure functional capacity in older adults is gait (walking) speed, which is a strong predictor of life expectancy. Data suggest that if you have a walking speed of 1.6 meters (about 5.2 feet) per second (approximately 3.5 mph) at the age of 65, your life expectancy is another 32 years, meaning you may live into your late 90s. Having a walking speed at or below the cutoff for sarcopenia, which is 0.8 meters (about 2.6 feet) per second, your life expectancy would be another 15 years, which means you’d be predicted to live to 80. At this speed, you would not be able to make it safely across a typical pedestrian crossing before the light changes to red. Strength as a Predictor of SurvivalStrength can also tell us a lot about an individual’s chances of survival. Egan presents data from a study in which people’s chest and leg press strength were measured to arrive at a composite score of whole body strength. The pattern is quite revealing, showing the strongest one-third of the population over 60 had a 50% lower death rate than the weakest. Exercise guidelines recommend getting 150 minutes of aerobics exercise and two strength training sessions per week. As noted by Egan, you need both. It’s not just one or the other. Research shows aerobic exercise in isolation reduces your all-cause mortality by 16% and strength training-only reduces it by 21%, whereas if you do both, you reduce your all-cause mortality by 29%.4 Disturbingly, U.K. data suggest only 36.2% of adults over the age of 30 meet aerobic guidelines, and a minuscule 3.4% meet strength training guidelines. Part of the problem may be that many don’t want to go to the gym. But there’s little difference between doing gym-based strength training and doing bodyweight resistance training at home. The Danger of Bedrest and Disuse AtrophyAs noted by Egan, enforced bedrest, such as acute hospitalization, can have a dramatic impact on your muscle mass. For example, a 2015 review5 in Extreme Physiology & Medicine notes you can lose 2.5% of your muscle mass in the first two weeks of bedrest. By Day 23, you can have lost up to 10% of your quadriceps muscle mass. As explained in this review:6
Research7 has shown even healthy young subjects in their 20s can lose 3.1 pounds of muscle mass in a single week of bedrest. This is why it is so important to have a reserve in case you wind up in the hospital and lose this much muscle mass. It may take you the better part of a year to regain that muscle, as gaining muscle mass is hard work and many elderly fail to do so. The loss of muscle mass also significantly decreases your insulin sensitivity. One of the reasons for this has to do with the fact that muscle tissue is a significant reservoir for the disposal of glucose. Your muscle tissue also produces cytokines and anti-inflammatory myokines that play an important role in health. Concurrent Exercise TrainingWhile three to five sessions of aerobic exercise and two or more strength sessions per week may sound like a lot, for many, the lack of time is a restricting factor. However, some of these sessions can be done together. “That’s called concurrent exercise training,” Egan says. He goes on to cite research looking at time matched concurrent exercise in the elderly, 65 and older, where an aerobic training group and a strength training group were compared to a group that spent half of their session doing aerobic exercise and the other half doing resistance training. All groups spent the same overall time exercising (30 minutes, three times a week for 12 weeks). In terms of leg strength, the concurrent training group had better responses to training than aerobic or strength training alone. There was little difference in lean body mass, meaning they didn’t necessarily bulk up, but they had a 50% increase in strength nonetheless. They also lost more body fat around the trunk area. In short, concurrent training appears to give you more bang for your buck. Blood Flow Restriction TrainingOne of the reasons I’m so passionate about blood flow restriction (BFR) training is because it has the ability to prevent and widely treat sarcopenia like no other type of training. There are several reasons why BFR is far superior to conventional types of resistance training in the elderly. Importantly, it allows you to use very light weights, which makes it suitable for the elderly and those who are already frail or recovering from an injury. And, since you’re using very light weights, you don’t damage the muscle and therefore don’t need to recover as long. While most elderly cannot engage in high-intensity exercise or heavy weightlifting, even extraordinarily fit individuals in their 60s, 70s and 80s who can do conventional training will be limited in terms of the benefits they can achieve, thanks to decreased microcirculation. This is because your microcirculation tends to decrease with age. With age, your capillary growth diminishes, and capillary blood flow is essential to supply blood to your muscle stem cells, specifically the fast twitch Type II muscle fiber stem cells. If they don’t have enough blood flow — even though they’re getting the signal from the conventional strength training — they’re not going to grow and you’re not going to get muscle hypertrophy and strength. BFR, because of the local hypoxia that is created, stimulates hypoxia-inducible factor-1 alpha (HIF1a) and, secondarily, vascular endothelial growth factor (VEGF), which acts as “fertilizer” for your blood vessels. VEGF allows your stem cells to function the way they were designed to when they were younger. What’s more, the hypoxia also triggers vascular endothelial growth factor, which enhances the capillarization of the muscle and likely the veins in the arteries as well. Building muscle and improving blood vessel function are related, which is why BFR offers such powerful stimulus for reversing sarcopenia. In short, BFR has a systemic or crossover training effect. While you’re only restricting blood flow to your extremities, once you release the bands, the metabolic variables created by the hypoxia flow into your blood — lactate and VEGF being two of them — thereby spreading this “metabolic magic” throughout your entire system. To learn more, please see my special report, “What You Need to Know About BFR,” and “BFR Training for Muscle Mass Maintenance.” Nutrition for Muscle MaintenanceIt should come as no surprise that there is an important synergy between nutrition and exercise. When it comes to muscle building and maintenance, amino acids, the building blocks of protein, are of particular importance. In the podcast above, Megan Hall, scientific director at Nourish Balance Thrive delves into this topic at greater depth and reviews the current recommended daily allowances of protein compared to the optimal levels needed to support muscle mass and strength in at various life stages.8 Research9 looking at post-prandial protein handling and amino acid absorption shows 55.3% of the dietary protein of a given meal is in circulation within five hours after eating, which significantly increases muscle protein synthesis. Research10 suggests healthy young adult men “max out the protein synthesis signal from a given meal” at a dose of 0.24 grams of protein per kilogram of total bodyweight, or 0.25 grams of protein per kilogram of lean body mass. The current U.S.-Canadian recommended dietary protein allowance is 0.8 g/kg/d (0,36/grams/pound/day), but healthy older adults may actually require about 1.20 g/kg/d or .55 grams/pound/day. According to this study:11
Amino acids also act as signaling molecules that trigger muscle growth. Leucine is a particularly potent signaling agent, although all of the amino acids are required to actually build the muscle. The richest source of leucine (which helps regulate the turnover of protein in your muscle), by far, is whey protein. In fact, it can be difficult to obtain sufficient amounts of leucine from other sources. The typical requirement for leucine to maintain body protein is 1 to 3 grams daily. However, to optimize its anabolic pathway, research shows12 you need somewhere between 8 and 16 grams of leucine per day, in divided doses.13,14 To reach the 8-gram minimum, you’d have to eat nearly 15 eggs.15 Whey, on the other hand, contains about 10% leucine (10 grams of leucine per 100 grams of protein).16 So, 80 grams of whey protein will give you 8 grams of leucine. Time-Restricted Eating Adds BenefitsOne of the problems with Egan is that he’s not very literate on time-restricted eating. During the question and answer portion, an audience member asks him about it and he admits he hasn’t studied it. This is important because restricting your eating window to six to eight hours, which means you’re fasting 14 to 18 hours each day, would make it far easier for each of the meals to be over the leucine threshold. It will also activate autophagy, which is another factor essential for optimal muscle growth. Autophagy is a self-cleaning process in which your body digests damaged cells, which in turn encourages the proliferation of new, healthy cells. The harder your workout, the more autophagy you will activate. So, I recommend fasting for as long as you can before your morning workout, and then, shortly thereafter, have your largest meal of the day with plenty of high-quality protein, making sure you get several grams of leucine and arginine, both of which are potent mTOR stimulators. The mTOR pathway is an important key for protein synthesis and muscle building. As explained in David Sabatini’s excellent review paper “mTOR at the Nexus of Nutrition, Growth, Ageing and Disease,” published in Nature Reviews Molecular Cell Biology:17
In summary, fasting activates autophagy, allowing your body to clean out damaged subcellular parts. Exercising while fasted maximizes autophagy even further. In fact, exercising while you are fasting for more than 14 to 18 hours likely activates as much autophagy as if you were fasting for two to three days. It does this by increasing AMPK, increasing NAD+ and inhibiting mTOR. Refeeding with protein after your fasted workout then activates mTOR, thus shutting down autophagy and starting the rebuilding process. These two processes need to be cyclically activated to optimize your health and avoid problems. Muscle Health Is Central to an Active LifestyleAs noted by Egan, “Hopefully I've convinced you that muscle health is central to active lifestyles. There's been this increased awareness of muscle size, but I think we need to emphasize the idea about strength and function. These are the things that are easiest to change with the right type of training.” In short, if you want to increase muscle size and strength, then there’s no getting around resistance training. It simply must be part of your exercise prescription, and concurrent training, where you’re combining aerobic and strength training in a given session is a time-efficient model. BFR is also a particularly excellent way to ensure you’re getting effective strength training without the risks of conventional strength training using heavy weights, and is easy to combine with exercises such as walking and swimming. You simply wear the BFR bands while walking or exercising as normal. Defy Aging by Improving Your Muscle MassIn my February 2020 interview with Ben Greenfield, author of “Boundless: Upgrade Your Brain, Optimize Your Body & Defy Aging,” we discuss the importance of strength training and getting the appropriate amount of protein to build and maintain your muscle mass and optimize mitochondrial density and biogenesis. In summary, Greenfield recommends a fitness program that includes the following types of exercise in order to target the main pathways involved in health and aging: • High-intensity interval training once a week to boost mitochondrial density and biogenesis -- Brief spurts of exercise followed by longer rest periods. Greenfield recommends a 3-to-1 or 4-to-1 rest-to-work ratio. • Muscle endurance training two to three times a week to improve lactic acid tolerance -- An example is the classic Tabata set, which has a 2-to-1 work-to-rest ratio. • Longer training sessions twice a week to improve your VO2 max -- To target and improve your VO2 max, you’ll want your training sessions to be longer, about four to six minutes in duration with four to six minutes of recovery in between, for a 1-to-1 work-to-rest ratio. Examples include The New York Times' seven-minute workout18 and bodyweight training done in a fast explosive manner or with a very light medicine ball, sandbag or kettle bells. • Long walk once a week to improve your stamina -- Greenfield recommends taking a 1.5- to three-hourlong walk, bike ride or paddle session — anything where your body is engaged in chronic repetitive motion for a long period of time — preferably in a fasted state. Alternatively, do 20 to 30 minutes of fasted cardio followed by a cold shower. • Super-slow weight training once or twice a week to improve muscle strength — Alternatives include elastic band training systems and blood flow restriction (BFR) training. You can also combine BFR with super-slow training. from http://articles.mercola.com/sites/articles/archive/2020/03/14/skeletal-muscle-aging.aspx The ketogenic diet is beneficial for many people as it helps with weight control and management and offers protection against a number of health ailments. Approached incorrectly, however, it can actually be harmful. In this short video Dr. Eric Berg warns, "The last thing you want to do is get the benefits of the ketogenic diet but then have deficiencies of omega-3 fatty acids." If you're following a standard ketogenic nutrition plan I recommend you focus on eating healthy fats and 1 gram of protein for every kilogram of body mass. You should also keep your net carbohydrates to not more than 10% of your daily calories. However, if you're not getting enough omega-3 fat it can be detrimental to your health. As Berg describes, your body uses fat for many reasons, including the lining and protection of cell membranes, the processing of fat soluble vitamins, the catalyzation of chemical reactions, and the production of hormones and bile. Without enough healthy fat, and the right kinds of fat, you may increase your risk for negative health conditions. Omega-3 fats are one type of polyunsaturated fats (PUFAs) you must get from your food since your body doesn't make them.1 The second type of PUFAs are omega-6 fats. Your body needs both in a balanced ratio for optimal health. As the National Institutes of Health describes,2 "The three main omega-3 fatty acids are alpha-linolenic acid (ALA), eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA). ALA is found mainly in plant oils such as flaxseed, soybean and canola oils. DHA and EPA are found in fish and other seafood." Omega-3 Fats Are Crucial to Heart HealthEPA, DHA and ALA each have unique functions. DHA is particularly important for your brain,3 as about 90 percent of the fat in your brain is DHA, while EPA appears to be of particular importance for heart health.4 ALA, found in plants, is the "parent fatty acid" and is used as a source of energy. However, while some may be converted to EPA and DHA in the body, conversion to EPA is restricted and unreliable, and conversion to DHA is severely restricted.5 Making lifestyle changes, such as exercising, stopping smoking and improving your diet, have a significant impact on your heart health. The authors of one study published in the New England Journal of Medicine6 analyzed the risk of a cardiovascular event while taking icosapent ethyl. The medication is a "highly purified eicosapentaenoic acid ethyl ester" that is "a synthetic derivative of omega-3 fatty acid."7 The data8 were based on information gathered from 8,179 participants who were followed over a period of 4.9 years. The researchers identified end points of the study as death from a cardiac event, or a nonfatal heart attack or stroke. The participants either had heart disease or risk factors for it and were taking statins. They were given either a placebo or 2 grams of icosapent ethyl twice a day. Those who took the medication had a significantly lower number of ischemic events than those taking the placebo. Although the drug had previously been approved in 2012 for people with high triglycerides, in December 2019 the FDA approved it for use alongside statins.9 Its mechanism of action has not been completely identified, but the American Heart Association lists the following reasons natural omega-3 may have an impact on lowering the risk of heart disease:10
As explained in a meta-analysis published in Circulation,11 scientists concluded there was a growing body of evidence that omega-3 fats can prevent sudden cardiac death by "modulating ion channels so as to stabilize the cardiomyocytes electrically." EPA and DHA Lowers Inflammation, Pain and DepressionEPA and DHA have been shown to improve blood pressure,12 reduce overall inflammation, reduce the effects of rheumatoid arthritis13 and depression14 and help to slow the progression of Alzheimer's disease.15 Other conditions linked to inflammation that are positively affected by omega-3 fatty acids are Hashimoto's disease and inflammatory bowel disease. Nutritionist Steph Lowe spoke with Starts at 60 about omega-3 fats, saying:16
Your Body Needs Cholesterol for Vital FunctionsFor decades you've been told that high cholesterol levels will increase your risk for heart disease. In fact, some in the health community continue to stress your level of cholesterol as a biomarker for heart risk, when in fact it's smarter to take a global view of cholesterol — how it affects your body and what you can do to reduce your risk of heart disease beyond the simple narrative which focuses on cholesterol as some kind of culprit. Cholesterol is vital to your overall health, as it helps with the manufacturing of hormones and vitamin D. About 80% of the cholesterol in your body is made in your liver and intestines, while the rest has to come from your food.17 There are two categories of cholesterol: The first is high density lipoprotein (HDL), which many know as the "good" type that moves cholesterol out of your arteries.18 The second is low-density lipoprotein (LDL) or what many know as the "bad" type that may build up and form plaque in the arteries. The American Heart Association focuses on your total cholesterol number, which they recommend you keep at 150 milligrams per deciliter (mg/dL).19 In the 2015-2020 Dietary Guidelines for Americans, it's noted that the Institute of Medicine recommends20 "… individuals should eat as little dietary cholesterol as possible while consuming a healthy eating pattern." However, in the Scientific Report of the 2015 Dietary Guidelines Advisory Committee, it was acknowledged that "… cholesterol is not considered a nutrient of concern for overconsumption."21 It's troubling to know that the public hears one thing and something completely different is discussed at a medical advisory meeting. Using cholesterol as a sole marker for the risk of heart disease is inaccurate because, like most things related to your body, its mechanisms are complex and interrelated. Increasing amounts of evidence show that people with higher levels of cholesterol live longer lives.22 As summarized by the authors of one study:
While evaluating your heart disease risk, consider your fasting insulin and blood sugar levels, waist circumference and iron levels. I discuss the relationships of these factors to your heart health and the importance of differentiating the types of LDL in "Important Facts About Cholesterol and Heart Disease." There are a number of ways higher levels of cholesterol may have a protective effect on your health; these are discussed in "Higher Cholesterol is Associated With Longer Life." Instead of looking at simple levels, there are two indicators that are important: your HDL/total cholesterol ratio and your triglyceride/HDL ratio. Why Testing Your Omega-3 Level Is so ImportantAn omega-3 deficiency leaves you vulnerable to several chronic diseases and lifelong challenges. Optimizing your levels is truly a foundational strategy to attaining and maintaining good health. The best way to determine if you're eating enough food with omega-3 is to get tested. In fact, research23 supported by the National Institutes of Health suggests that an omega-3 test is a good predictor of overall health and all-cause mortality.24 Leaders of the study measured the omega-3 index in 2,500 participants; they found that those with the highest omega-3 index had lower risks of heart problems. The omega-3 Index is a measure of the amount of EPA and DHA in the membranes of your red blood cells (RBCs). As Berg mentioned, fat is a component of cell membranes. Your index is expressed as a percent of your total RBC fatty acids. The omega-3 index has been validated as a stable, long-term marker of your omega-3 status, and it reflects your tissue levels of EPA and DHA. I just had my omega-3 index done last week from GrassrootsHealth and it was 11.1% and my 6:3 ratio was 2.7. An omega-3 index over 8% is associated with the lowest risk of death from heart disease, while an index below 4% places you at the highest risk of heart disease-related mortality. Given its importance to your health, it is absolutely worth your time to complete the simple blood test required to determine your omega-3 index. I firmly believe an omega-3 index test is one of the most important annual health screens that everyone needs. Please note I make no profit from these tests. I merely supply them as a convenience for my readers. It's the same price whether you buy it from me or directly from GrassrootsHealth.25 Protect Your Heart and Brain With Animal-Based Omega-3You can get all three types of omega-3 fats from your food, but EPA and DHA come mostly from fatty fish, seafood and grass fed beef and dairy products. Grass fed beef and dairy products, incidentally, offer a nearly 1-to-1 ratio of omega-3 to omega-6 fatty acids.26 Lowe points out the importance of where you source your fish:27
Your best sources of fatty fish are wild-caught Alaskan salmon, herring, mackerel and anchovies. The larger predatory fish, such as tuna, have much higher amounts of toxins such as mercury. As Berg stated in the video, steer clear of grain-finished beef as the omega-3 fatty acids are significantly reduced. As I touched on above, it's important to realize your body doesn't convert enough plant-based omega-3 to meet your needs. This means that if you're vegan, you must figure out a way to compensate for the lack of marine or grass fed animal products in your diet. While the authors of some studies28 suggest that algae products may be an effective alternative, the only way to know if you're on the right track is to test. If you are pregnant I urge you to check your vitamin D and omega-3 levels, as these two nutrients are vital for healthy fetal development and can dramatically reduce your risk of complications during pregnancy and delivery. If your test results are low, and you are considering a supplement, compare the advantages and disadvantages of fish oil and krill oil as you'll see in the infographic below. Krill are wild-caught and sustainable; krill oil is also more potent than fish oil and is less prone to oxidation. 
Embed this infographic on your website: Click on the code area and press CTRL + C (for Windows) / CMD + C (for Macintosh) to copy the code from http://articles.mercola.com/sites/articles/archive/2020/02/24/omega-3-index-more-predictive-than-cholesterol-levels.aspx Youthfulness, vitality and a long, prosperous life have been sought after throughout human history. And now, it seems scientists may have discovered one of the keys to turning back the hands of time. Researchers from Arizona State University and Texas A&M University have made a breakthrough discovery in plant DNA that could lead to stopping cancer cold and slowing the aging process, ABC affiliate News 15 Arizona reports.1 The research involves telomerase, an enzyme that produces the DNA of telomeres, which have been shown to play a role in the aging process. As your telomeres lengthen, they protect your cells from aging. Take It From the Experts: Centenarians Share Their SecretsWhile direct applications from the study to human health are distant, there are a number of things you can do now to improve your health span, according to one of the co-authors. In interviews and surveys with centenarians, certain themes came up time and time again when they explained why they've lived so long. The 10 most common reasons they gave for their long lives were:
Centenarians are the fastest growing segment of the U.S population, with numbers doubling every decade; by the year 2050, the number of people who will have reached the century mark is expected to pass 1 million. Centenarians have 60% lower rates of heart disease, stroke and high blood pressure, yet scientific explanations for their health and longevity remain elusive. As a group, they are happy and optimistic and have extremely low rates of depression and other psychiatric problems, suggesting you may live longer by maintaining the right attitude. Hopefulness and Positivity Affect the HeartThere are compelling links between cardiac health and mental health. For example, having untreated depression or anxiety disorder increases your odds of having a heart attack or developing heart disease. Stress hormones are again a primary culprit. According to Julia Boehm, author of earlier Harvard studies looking at optimism and cardiovascular disease (CVD):2
With a later study,3 author Eric Kim told The Harvard Gazette:
The Significance of Sound SleepGetting adequate sleep is an important part of both mental and physical health. Too much or too little can lead to metabolic issues, as well as changes in mood and your ability to focus. Your circadian rhythm, which affects your sleep/wake cycle, holds implications for your brain, body temperature, hormones and cell regeneration among other things.4
Italian researchers found that deletion of a specific gene related to aging also affects glucose homeostasis. According to their article, published in the journal Glia, "Disruption of the circadian cycle is strongly associated with metabolic imbalance and reduced longevity in humans."6 Telomeres and telomerase activity are also controlled by your circadian rhythm,7 making proper sleep an important part of longevity. In a 2007 study involving 21,268 adult twins, Finnish researchers found that adults who slept more than eight hours per night, or less than seven, showed increased risk of death.8 Of course, the quality of your sleep is also important, not just the quantity. Good quality sleep, in the appropriate amount, can improve how you think and adapt to the demands on your time and changes throughout your day. There is evidence suggesting that a calm mind and active body are two important ingredients for longevity. The meditative technique known as "mindfulness" has even been shown to have a beneficial effect on genetic expression. According to a 2018 article in Brain, Behavior, and Immunity,9 meditation has also been found to affect the enzyme telomerase, which some researchers believe is actively involved with the process of aging. After Resting, Be Sure to RefuelAdditionally, there are many other strategies you can implement to improve your health and extend your life span. To live longer, you need to counteract the progressive loss of muscle mass by increasing your protein intake as you age. The elderly, bodybuilders and endurance athletes typically have higher than normal protein requirements for their age group. It's also important to cycle high and low protein intake. Ideally, combine protein restriction with time-restricted eating, followed by increased protein intake on strength training days. Fasting 16 to 20 hours each day is likely ideal, as this allows your body to more thoroughly deplete the glycogen stores in your liver. Benefits of fasting include the suppression of mammalian target of rapamycin (mTOR) and the activation of autophagy, both of which play decisive roles in disease prevention and longevity. You'd also be wise to avoid eating two to three hours before bed, as late-night eating will decrease your nicotinamide adenine dinucleotide (NAD+) level, which is crucial for health and longevity. Late-night eating will also make you pack on unwanted pounds, as the excess calories will not be burned but stored as fat. Preventing Cognitive DeclineNaturally, if you're going to live longer, you'll want to be healthy for the remainder, and that includes maintaining your cognitive function. Specific nutrients that can help prevent dementia and cognitive decline include vitamin D, DHA, folate and magnesium. Additional nutrients of notable interest, which are readily available in supplement form, include:
Kick the Chemicals to the CurbNaturally, there's also the issue of toxic exposures, which can take a toll on your health, so avoiding toxins is a given, right along with eating a wholesome diet of organic, unprocessed foods. This includes tossing out your toxic household cleaners, soaps, personal hygiene products, air fresheners, bug sprays, lawn pesticides and insecticides, just to name a few, and replacing them with nontoxic alternatives. A group of scientists from Southeast University and Changzhou No. 7 People's Hospital in China recently published a study10 about the role of plastics in our environment and how long-term exposure affects our health. They found that high concentrations of nanoplastic particles reduced the life span of roundworms. They believe that different levels of exposure may have effects on locomotion and immune response, indicating that nanopolystyrene is likely toxic to all types of organisms. "Our results highlight the potential of long-term nanopolystyrene exposure in reducing longevity and in affecting health state during the aging process in environmental organisms," they wrote. Next week I will post my interview with leading researcher James Clement on his book, "The Switch," that will go into far more fascinating details on this topic. from http://articles.mercola.com/sites/articles/archive/2019/12/24/10-ways-to-live-longer.aspx The celery juice phenomenon is often attributed to Anthony William, who considers himself the originator of the Global Celery Juice Movement.1 The movement has received both social media and major media attention in The New York Times2 and LA Times3 among others. You can easily grow your own organic celery at home when you keep it cool, give it an unfailing supply of water and plant it in good soil.4 It’s important to choose organically grown celery as it’s one of the more contaminated vegetables available at the grocery store. Choose Organic Celery for Your TableEach year the Environmental Working Group (EWG),5 a nonprofit organization aimed at protecting health and the environment, publishes a guide to pesticides in produce. This document is called “The Dirty Dozen;” celery usually makes an appearance on the list. In 2012, it was No. 2 on the list and the one most likely to contain multiple pesticides, with 96% of the samples testing positive and nearly 90% retaining more than one pesticide.6 By 2019, celery had dropped to number 11, having been overtaken by strawberries, spinach and kale.7 Before testing the fruits and vegetables, the produce was washed and peeled as consumers may be expected to at home.8 The Shopper’s Guide, which the EWG has published since 2004, ranks contamination in 47 fruits and vegetables based on more than 40,900 samples.9 Carla Burns, EWG Research Analyst, commented:10
The American Academy of Pediatrics11 emphasizes children's exposure should be limited. Pesticide exposure is linked with poor mental development, pervasive developmental disorders and attention deficit hyperactivity disorder. Their data also suggest an association with physical birth defects, fetal death and neurodevelopmental effects. The EWG evaluated the U.S. Department of Agriculture's tests, which found 225 different pesticides on fruits and vegetables.12 Dr. Philip Landrigan is director of the Global Public Health Initiative at Boston College and one of the writers of the 1993 National Academy of Sciences study, “Pesticides in the Diets of Infants and Children.”13 He underscores the implications of pesticide exposure and stresses that when possible, steps should be taken to lower a child's exposure while continuing to offer a diet full of fresh produce.14 The dangers of pesticide exposure continue into adulthood. The Pesticide Action Network reports long-term toxicity at low doses has been associated with Parkinson's disease, depression, anxiety, asthma and certain cancers.15 Celery Juice Trending: Rising Cost Is a Perfect StormMichael Karsch is the CEO of a New York chain of juice bars, Juice Press,16,17 and he tracks juice trends. In 2018 he noticed a rise in celery juice interest and decided to offer a 12-ounce, one ingredient drink for $7. Karsch spoke to The New York Times about the shortage and his take on the future, saying:18
Vandana Sheth,19 spokesperson for the Academy of Nutrition and Dietetics, finds these trends are often driven by social media and may be enticing because she believes many people are looking for a quick fix for their health. She noted moving back and forth between different trending eating plans may be dangerous, and said:20 “I'm seeing a lot more of a disordered way of eating in my practice. It's not sustainable long-term.” Sammy Duda,21 senior vice president of Duda Farm Fresh Foods, one of the largest celery growers in the world, spoke to The New York Times about his family’s familiarity with the supply and demand issue when celebrities endorse a specific type of vegetable juice. Out of 10 items listed on their products page, three of those are packaged celery and one is fresh celery.22 The cost not only is affected by demand from the juice trend, but also by the weather. The New York Times23 reports a warm, dry fall in Palm Beach, Florida, where some of the crop is grown, and a cold, wet winter on the west coast where other fields are located, have affected growth and harvest. The crop on Duda Farm was also impacted by a soil-borne disease, which together added up to a shorter than normal supply in an environment with a greater than normal demand. Phytonutrients Promote Health BenefitsAlthough there’s been a push to promote celery as a cure for many different health conditions, scientific evidence supports a more limited number. One cup of raw celery contains 40% of your daily value of vitamin K.24 In addition to this it contains 11% of your daily value of molybdenum,25 a trace mineral your body uses for the detoxification of heavy metals. Some of the larger threats from heavy metal are associated with cadmium, mercury, arsenic and lead.26 Long-term exposure may result in neurological damage, skin cancers, kidney damage and bone fractures. Toxicity will depend on several factors including the route of exposure and duration.27 You can read more about how molybdenum functions in heavy metal detoxification in my past article, “The Three Pillars of Heavy Metal Detoxification.” Celery also contains measurable amounts of folate, potassium and vitamin B2. Celery stalks are a great source of antioxidants, phytosterols, flavanols and flavones, many of which provide anti-inflammatory benefits.28 But, one of the more advantageous compounds found in celery may be apigenin, gaining interest for its potential to fight cancer.29 Apigenin is a flavonoid found in several fruits and vegetables and some Chinese medicinal herbs. It has strong anti-inflammatory, antibacterial and antiviral properties and is now being reported as subduing different forms of cancer. This has been found in vitro and in vivo by initiating apoptosis and autophagy, as well as stimulating an immune response.30 Apigenin is associated with stimulating the growth of nerve cells. One animal study demonstrated learning and memory improvements when apigenin was injected or taken orally.31 Studies have also linked apigenin with activating AMP-activated protein kinase (AMPK) in human skin cells. The results suggest that “one of the mechanisms by which apigenin exerts its chemoprotective action may be through activation of AMPK and induction of autophagy in human keratinocytes.”32 In another published study, scientists looked at the anticarcinogenic properties on the regulation of oxidative stress and DNA damage. They wrote:33
Large Amounts May Interfere With Kidney FunctionAlthough not high in oxalates, celery has between 11 and 20 mg for every 3 1/2 ounces of the vegetable. Oxalates are found in plant and animal foods with some of the more concentrated sources including spinach, almonds and beet greens.34 Oxalates are related to kidney stone formation and calcium absorption. Your gut bacteria play a role in how available oxalate will be for absorption. A combination of oxalate and nonoxalate-containing foods will also impact how much soluble oxalate gets absorbed from the digestive tract.35 Calcium oxalate kidney stones are among the more common types of stones. However, it's not high amounts of calcium that cause the stones but, rather, oxalate.36 Oxalates are compounds that protect plants from predators.37 The oxalic acid binds with calcium to make it less bioavailable and insoluble, increasing the risk of kidney stones. Oxalates are broken down by gut bacteria, but when your microbiota are compromised the compounds enter the bloodstream and get stored in the kidneys. While 11 to 20 mg of oxalate in one 3 1/2-ounce serving of celery is minor, drinking 16 ounces of celery juice each day may not be. One 16-ounce glass of celery juice requires one large bunch of celery,38 which often contains 10 stalks39 and weighs about 16 ounces or more.40 Drinking this much celery juice is roughly equivalent to 90 mg of oxalates every day. In addition to other foods, including chocolate, berries, nuts, legumes and grains,41 this may increase your risk for kidney stones. Soothing Chamomile Tea — An Option With Similar BenefitsHerbal teas are a rich source of polyphenols and flavonoids with antioxidant and anti-inflammatory properties. One of the most soothing is chamomile tea, belonging to the Asteraceae family42 containing a large number of herbs, shrubs and trees.43 In addition to being used as a tea, chamomile has been praised for many health benefits, including those in the volatile oils found in the flowers. One of the major constituents in the flower is apigenin, primarily found as a glycoside.44 Adults can use the volatile oils from the flower in a bath, as a cream for flaky skin, as an inhalant or tincture to relieve menstrual cramps and to improve sleep. For more information about the benefits of chamomile and how to make a tincture at home, see my past article, “What Are the Benefits of Chamomile?” from http://articles.mercola.com/sites/articles/archive/2019/09/23/celery-juice-benefits.aspx Your entire body takes direction from your hormones. Hormones are secreted by your endocrine system and are responsible for telling your organs what to do and when to do it.1 They are essentially chemical messengers that travel throughout your bloodstream, working slowly over time to affect processes like growth and development, metabolism and reproduction. Sometimes, these chemical messengers may get out of balance, and this leads to chronic disorders such as Type 2 diabetes, weak bones and infertility.2 Hormones may be secreted by your adrenal glands, endocrine-related organs, hypothalamus, sex glands and other organs.3 Progesterone is important to fertility and supporting a pregnancy. It’s a steroid hormone secreted by the corpus luteum and then by the placenta if you become pregnant.4 In some cases, when couples suffer from infertility, they choose in vitro fertilization (IVF). This is a complex series of procedures in which eggs are retrieved from the ovaries, fertilized by sperm in a lab and then transferred into the uterus.5 One full cycle can take up to three weeks6 and cost $12,000.7 In response to her struggles with infertility, Amy Galliher-Beckley, Ph.D.,8 co-founded MFB Fertility and the progesterone test Proov.9 The Estrogen and Progesterone RelationshipEach of your bodily systems maintains a balance to help you maintain optimal health. Your reproductive system is no different. For a woman, there are several hormones affecting a complex system to mature an egg follicle and release an egg where it travels to the uterus. If fertilized, the egg must implant into the uterus, called the endometrium, where it begins to develop into a baby. These events are controlled by hormones secreted from several sources in the body. The ovaries produce the eggs and are the main source of estrogen. The adrenal glands sit on top of each kidney and also make a small amount. Estrogen plays a role in physical changes during puberty; it also controls the menstrual cycle, protects bone health and affects your mood.10 The second hormone essential to fertility is progesterone, a steroid hormone that is first secreted by the corpus luteum. After the egg is released, the corpus luteum is left attached to the ovary, which functions as a temporary gland.11 These two hormones are controlled by the release of other hormones. During the menstrual cycle gonadotropin-releasing hormone is secreted from the hypothalamus, triggering the secretion of follicle-stimulating hormone (FSH) from the pituitary gland.12 This begins follicle development and triggers a rise in estrogen. Luteinizing hormone (LH), also secreted by the pituitary gland, supports the maturation of the follicle and a trigger to cause the egg to be released. When estrogen levels get sufficiently high it signals a sudden release of LH, around mid-cycle, which triggers a set of events that ultimately release the mature egg from the follicle.13 Once released, the empty follicle becomes the corpus luteum, which produces progesterone. The release of progesterone triggers the uterus to develop a highly vascularized bed suitable for implantation of a fertilized egg. Without fertilization, the corpus luteum begins to degenerate, the secretion of progesterone drops off and menstruation occurs. If pregnancy occurs then the corpus luteum produces progesterone for the first 10 weeks until production is taken over by the placenta.14,15 Not About Getting Pregnant, but Staying PregnantAs Beckley explains in her interview with Forbes magazine,16 her test is not about getting pregnant, but rather staying pregnant. Progesterone not only prepares the uterus for the egg to implant; it also protects the endometrium from degeneration and menstruation. While the body is producing high levels of progesterone during a pregnancy, a second egg will not mature.17 In order to maintain a pregnancy, the corpus luteum must continue to secrete progesterone. This maintains the blood vessels in the endometrium to feed the growing baby. It is in these early weeks that women with low levels of progesterone may have difficulty, both conceiving and developing the right environment for a fertilized egg to grow. Some women who do get pregnant are at a high risk for miscarriage.18 The test Beckley developed comes with sticks used in much the same way ovulation and pregnancy tests are used. These sticks measure the amount of progesterone metabolites excreted in the urine. To date, this is the first at-home, over-the-counter test used to evaluate a woman's ability to produce progesterone.19 Beckley explains:20
Luteal Phase Defect Increases Chances of MiscarriageThe luteal phase in a woman's cycle begins after ovulation and represents the second half of the menstrual cycle. The luteal phase is named after the corpus luteum. Luteal Phase Defect (LPD) results in an abnormal endometrial growth that may not support a pregnancy.21,22 While researchers struggle to identify the underlying dysfunction and efficacy of LPD in supporting fertility, experts report women undergoing IVF always have LPD present.23 LPD is marked with a luteal phase less than 11 days. However, not all physicians believe the condition exists; reliable tests are lacking.24 Beckley developed the Proov urine test to help women identify a reduction in progesterone during their cycle. According to Beckley,25 her test gives women more knowledge about how their body works and provides a foundation for asking their infertility doctors better questions. The test measures the presence of metabolites in the urine that should increase and remain elevated after ovulation. It may be used to confirm ovulation and confirm levels of progesterone afterward. A single negative test before ovulation followed by a single positive test will confirm ovulation for women trying to get pregnant.26 For women trying to conceive, the test is recommended four days after peak fertility and then for continued testing 10 days past ovulation.27 When questions arise about levels of progesterone to maintain a pregnancy, they recommend testing six days after peak fertility and as needed during the pregnancy since the test should remain positive. Other Functions of ProgesteroneAlthough LPD has a significant impact on a woman's ability to carry a pregnancy, it is the subject of debate.28 In some cases, the ovaries release enough progesterone but the uterine lining does not respond.29 LPD has been linked to other health conditions, including:30
In some circumstances, when these conditions are treated, the LPD resolves.31 Later in life, if levels of progesterone decline, a woman’s period may become irregular, heavier and longer,32 increasing her chance of experiencing anemia, depending on the amount and length of her period.33 Variations in hormone levels after menopause may also influence cognition and mood.34 In a study of 643 healthy postmenopausal women, researchers found that while estrogen had little effect on tests of executive function or global cognition, progesterone concentrations were associated with verbal memory. The researchers suggest this positive association merits additional study. Bioidentical progesterone, also known as micronized progesterone in the oral form, has been successful in helping relieve hot flashes and night sweats during menopause. Dr. Jerilynn Prior from the University of British Columbia Vancouver presented her study at an endocrine society meeting during which she compared the use of progesterone to placebo.35 The study assigned 114 postmenopausal women into one of two groups, a placebo group and another who took 300 mg of micronized oral progesterone daily. To be eligible for the study, the women had to be off hormone therapy for at least six months.36 At the end of the 12-week study, researchers found that the group taking micronized progesterone demonstrated a 56% decrease in a score reflecting the number and intensity of symptoms, while the women taking the placebo reported a 28% decrease.37 Age Does Affect Hormone BalanceAs is borne out by the number of women struggling with hormonal imbalances as they age and those requiring fertility assistance to become pregnant after 40,38 Beckley is vocal about the difficulty women may have supporting a pregnancy after she turns 40.39 Beckley says,40 “The closer a woman gets to menopause, the least likely her body is going to be able to support a pregnancy.” Much of this is related to the imbalance of hormones required to successfully support a pregnancy that occurs as women age. Her research in designing the progesterone urine test led Beckley to believe 30% to 40% of women who undergo IVF treatment to become pregnant ultimately do not need IVF.41 Instead, they may require progesterone to develop a healthy endometrial lining and support early pregnancy. Overall Fertility Is on the DeclineCouples experience infertility for a number of reasons. In a study42 released in 2017, researchers evaluated 38 years of information and found sperm counts declined significantly between 1973 and 2011. The sperm counts declined 52% to 59% in men located in North America, Europe and Australia. The Australian Department of Health reports 1 in every 6 Australian couples suffers from fertility problems, which they attribute to the decision to have children later in life as well as declining sperm count. Quality and lifestyle factors such as smoking, not eating healthfully, consuming excessive amounts of alcohol and not having a healthy BMI also affect fertility.43 In May 2019, the Pew Research Center reported that for the fourth year in a row, key fertility indicators for U.S. couples declined, reaching a record low.44 Two of the three indicators used to determine fertility reflected a decline in numbers. The total fertility rate, or the estimation of the number of children a woman would have in her lifetime, was 1.73 children in 2018. This was lower than the estimate of 1.74 from the mid-1970s.45 Research suggests men’s fertility is affected by environmental toxins and chemicals you may find in your own home, which I discuss in a past article, “50 Percent Fertility Reduction Because of These Household Chemicals.” Additionally, as described in the past article, “Birth Rate Reaches Record Low as Premature Deliveries Rise,” statistics from the CDC show the number of new births was down 2% in 2018 as compared to 2017, but the number of premature births was rising. Infertility and pregnancy are complex conditions that likely need a comprehensive approach to experience a successful outcome. from http://articles.mercola.com/sites/articles/archive/2019/09/18/ivf-treatment.aspx More than 80 percent of schools in America use toxic pesticides as a preventative measure, whether it‘s needed or not. from http://articles.mercola.com/sites/articles/archive/2007/08/16/80-percent-of-schools-are-applying-pesticides.aspx |
Nia Pure NatureThe Provider of premium Quality Health Products To Live Better Lives Archives
March 2022
Categories |

 RSS Feed
RSS Feed
